How Exercise Reprograms Your Hormones to Burn Fat, Lower Cortisol & Boost Metabolism
What happens to testosterone, insulin, cortisol, and thyroid hormones during exercise? Learn how workouts transform metabolism and fat loss
EXERCISE
Dr. T.S. Didwal, M.D.(Internal Medicine)
3/21/202618 min read
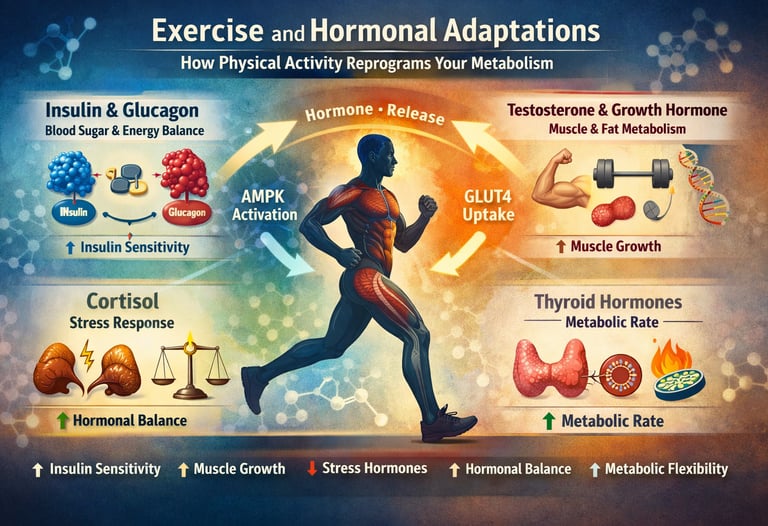
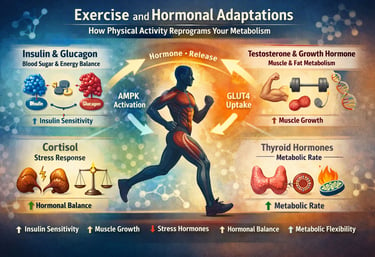
Exercise reprograms hormones by improving insulin sensitivity, increasing testosterone and growth hormone, regulating cortisol, and optimizing thyroid function. These adaptations enhance fat loss, muscle growth, and metabolic health, making exercise one of the most powerful non-pharmacological therapies for chronic disease.
Exercise is often reduced to calories burned or steps counted. But beneath this simplistic view lies a far more sophisticated reality: physical activity is a master regulator of the endocrine system, capable of reshaping insulin sensitivity, anabolic signaling, stress hormone balance, and thyroid-driven metabolic rate. In essence, every bout of movement acts as a precision hormonal intervention, reprogramming how your body stores fat, builds muscle, and manages energy (Mennitti et al., 2024).
At the core of this adaptation is the dynamic interplay between key hormones—insulin and glucagon, which regulate glucose metabolism; testosterone and growth hormone, which drive muscle protein synthesis and fat oxidation; cortisol, which orchestrates the stress response; and thyroid hormones, which determine basal metabolic rate and mitochondrial efficiency. Exercise does not act on these systems in isolation—it integrates them into a coordinated metabolic network that enhances metabolic flexibility, insulin sensitivity, and energy homeostasis (Lee et al., 2025).
Crucially, these effects occur both acutely and chronically. A single exercise session can increase insulin-independent glucose uptake via AMPK activation, while long-term training induces structural and molecular adaptations—such as increased GLUT4 expression, improved mitochondrial density, and enhanced hormonal receptor sensitivity—that persist for months (Mennitti et al., 2024). Emerging research further suggests that hormones traditionally viewed narrowly—like glucagon—have broader roles in lipid metabolism and systemic energy regulation, expanding our understanding of exercise endocrinology (Li et al., 2025).
For clinicians and patients alike, this reframes exercise not as lifestyle advice, but as foundational endocrine therapy—with profound implications for obesity, type 2 diabetes, sarcopenia, and healthy aging.
Exercise Prescription by Hormonal Goal
Insulin resistance → Zone 2 + resistance
Sarcopenia → resistance + protein
Fat loss plateau → HIIT + thyroid support
Clinical pearls
I. Independent" Glucose Gate
Scientific Perspective: Exercise stimulates GLUT4 translocation to the sarcolemma via the AMPK pathway, bypassing the need for insulin signaling.
Think of exercise as a "back door" into your cells. Even if your "front door" (insulin) is stuck due to insulin resistance, a brisk walk or strength session unlocks a side entrance, allowing your muscles to soak up blood sugar naturally.
2. Muscle as a "Metabolic Sink"
Scientific Perspective: Hypertrophy increases the total volume of metabolically active tissue, improving whole-body glucose disposal and increasing the Basal Metabolic Rate (BMR).
Your muscles are like a sponge for extra energy. The more muscle you carry, the larger your "sink" becomes. This means your body burns more fuel even while you are sleeping, making it much easier to manage your weight long-term.
3. The Hormonal "Afterburn" (EPOC)
Scientific Perspective: High-intensity exercise creates a significant Excess Post-exercise Oxygen Consumption (EPOC), driven by the need to restore ATP, clear lactate, and recalibrate the HPA axis.
The workout doesn't end when you stop moving. High-intensity intervals trigger a hormonal "repair mode" that keeps your metabolism elevated for hours. You are essentially paying for the workout in installments long after you’ve left the gym.
4. The Testosterone-to-Cortisol (T:C) Ratio
Scientific Perspective: The physiological value of a workout is defined by the T:C ratio; chronic elevation of cortisol without a reciprocal anabolic signal leads to systemic catabolism and overtraining syndrome.
It’s not about how hard you can push; it’s about how well you can recover. If you are always stressed and underslept, more exercise can actually backfire by keeping your stress hormones too high. Rest is an active part of the "prescription" for muscle growth.
5. Peripheral Thyroid Optimization
Scientific Perspective: Physical activity enhances the peripheral conversion of T4 to the biologically active T3, optimizing mitochondrial efficiency and thermogenesis.
Exercise acts as a "tuner" for your thyroid. Even if your thyroid gland is producing enough hormone, exercise ensures that the hormone is actually being converted into the active form your cells need to produce energy and keep your "engine" running hot.
1. Insulin and Glucagon: The Master Regulators of Metabolism
What These Hormones Do
Insulin and glucagon are the two central hormones that regulate how your body manages blood sugar and fuel. Insulin, released by the pancreas in response to rising blood glucose, acts like a key that unlocks your cells to absorb glucose. Glucagon does the opposite — it signals the liver to release stored sugar when your blood glucose drops.
Together, these two hormones orchestrate every meal and every fast. But exercise adds a fascinating third dimension to this conversation.
What Happens During Exercise
During physical activity, insulin levels actually drop, even as your muscles are absorbing glucose at a much higher rate. This seems paradoxical — how are your muscle cells taking in glucose without insulin? The answer lies in a molecular switch called AMPK (AMP-activated protein kinase), which is activated by the energy demands of exercise. AMPK triggers the movement of GLUT4 transporters to the cell surface, allowing glucose entry completely independently of insulin (Mennitti et al., 2024).
This is medically significant. For people with insulin resistance or type 2 diabetes, this pathway offers a way to improve glucose uptake even when the insulin signaling system is impaired.
At the same time, glucagon rises during prolonged exercise to ensure the liver keeps supplying glucose to working muscles. It activates two hepatic pathways: glycogenolysis (breaking down liver glycogen) and gluconeogenesis (manufacturing new glucose from amino acids and lactate). Recent research has expanded our understanding of glucagon's role significantly — it is no longer seen as a one-trick sugar-releasing hormone. Lee et al. (2025) highlight that glucagon exerts multi-organ effects including roles in lipid metabolism, amino acid turnover, and even cardiovascular function. In parallel, Li et al. (2025) describe the newly characterized hormone famsin, a glucagon-related peptide that appears to mediate fasting adaptation and energy sensing, opening an entirely new chapter in exercise endocrinology.
After Exercise: The Insulin Sensitivity Window
One of the most clinically valuable effects of exercise is the post-exercise improvement in insulin sensitivity that can last 24 to 72 hours after a session. During this window, your muscles are primed to absorb glucose with minimal insulin required. This is sometimes called the "metabolic window," and it has profound implications for meal timing, especially in people managing blood sugar levels.
With consistent training over weeks and months, these benefits compound. GLUT4 protein expression increases in skeletal muscle, mitochondrial density improves, and visceral fat — the metabolically active fat around your organs that drives insulin resistance — begins to shrink. The result is a fundamentally more insulin-sensitive body that handles carbohydrates, energy storage, and blood sugar regulation more efficiently.
Clinical takeaway: A combination of aerobic exercise (for insulin sensitivity) and resistance training (to build the muscle mass that acts as a "glucose sink") is the most effective exercise strategy for metabolic health.
Insulin facilitates glucose uptake into cells
Glucagon stimulates hepatic glucose release during fasting
Together, they maintain metabolic homeostasis, but exercise introduces an additional regulatory mechanism.
Combining aerobic exercise + resistance training provides the most effective strategy for improving insulin sensitivity and metabolic health.
2. Testosterone and Growth Hormone: Natural Anabolic Hormones
Testosterone: More Than a Male Hormone
Testosterone is produced primarily in the testes in men and in smaller amounts in the ovaries and adrenal glands in women. In both sexes, it plays a critical role in muscle protein synthesis, bone density, red blood cell production, and overall energy levels.
Resistance training is one of the most powerful natural stimulants of testosterone secretion. A heavy compound workout — think squats, deadlifts, rows — triggers a transient spike in testosterone, influenced by the volume of work performed, the intensity, the length of rest intervals, and the total muscle mass recruited. Larger, multi-joint movements involving more muscle mass tend to produce a greater hormonal response.
Ramadan et al. (2025) compared the hormonal responses of high-intensity interval training (HIIT) versus traditional resistance training in young women over a 10-week intervention. Both modalities produced significant hormonal adaptations, though their profiles differed: resistance training showed a stronger anabolic response in terms of testosterone and growth hormone, while HIIT produced greater improvements in metabolic hormones like insulin sensitivity markers. Importantly, both were effective — underscoring that the "best" exercise depends on the hormonal outcome you are targeting.
Over time, consistent resistance training does more than temporarily raise testosterone. It increases the sensitivity of androgen receptors in muscle tissue, meaning the same amount of testosterone produces a stronger anabolic effect. It also reduces visceral fat, which matters because adipose tissue contains the enzyme aromatase, which converts testosterone into estrogen. Less visceral fat means less unwanted testosterone-to-estrogen conversion, particularly relevant for men experiencing age-related hormonal decline.
For aging adults, this is especially important. Exercise represents one of the most evidence-supported strategies for mitigating late-onset hypogonadism — the gradual decline in testosterone that accompanies aging — without pharmaceutical intervention.
Testosterone plays a critical role in:
Muscle protein synthesis
Bone density
Energy metabolism
Clinical Relevance:
Exercise helps counter age-related testosterone decline (late-onset hypogonadism).
Growth Hormone: The Repair and Recomposition Hormone
Growth hormone (GH), secreted by the anterior pituitary gland in pulses, is a master regulator of body composition. It stimulates the liver to produce IGF-1 (insulin-like growth factor-1), which drives muscle repair, fat mobilization, and collagen synthesis.
High-intensity exercise — both resistance training and HIIT — is one of the most potent natural stimuli for GH secretion. The mechanism involves lactate accumulation and metabolic stress. When you push into the higher intensity zones of exercise, lactate production signals the pituitary to release GH. This is one reason that simply "going for a leisurely walk" — while valuable for general health — does not produce the same anabolic hormonal response as challenging your muscles and cardiovascular system.
The effects of GH include: accelerated lipolysis (fat breakdown, particularly of visceral and subcutaneous fat), enhanced muscle protein synthesis and remodeling, improved collagen turnover in joints and connective tissue, and faster recovery between training sessions.
With regular training, GH pulsatility improves — meaning the natural rhythmic bursts of GH release become more robust, contributing to better body composition and tissue regeneration even at rest. This has significant implications for anti-aging medicine, as declining GH pulsatility is a hallmark of the aging endocrine system.
Growth Hormone (GH) and Fat Loss
Growth hormone regulates:
Lipolysis (fat breakdown)
Tissue repair
Collagen synthesis
Regular training enhances GH pulsatility, supporting anti-aging and metabolic health.
3. Cortisol: The Stress Hormone in Exercise
Understanding Cortisol's Role
Cortisol, produced by the adrenal cortex in response to physical and psychological stress, often gets a bad reputation. In reality, it is not inherently harmful — it is contextually regulated. Cortisol mobilizes energy, maintains blood pressure, modulates immune function, and keeps blood glucose stable during periods of stress or prolonged exercise.
The problem arises when cortisol is chronically elevated, whether from overtraining, poor sleep, psychological stress, or inadequate nutrition. Under those conditions, cortisol promotes muscle breakdown, central fat accumulation, impaired insulin sensitivity, and suppressed immune function — the very opposite of what most people train for.
Acute vs. Chronic Exercise Effects
During exercise, especially high-intensity or prolonged sessions, cortisol rises appropriately to mobilize glucose and fat stores and maintain cardiovascular stability. This is normal and necessary.
A compelling recent study by Jaklová Dytrtová et al. (2026) demonstrated that repeated exercise in a cold environment produced a measurable increase in both testosterone and cortisol over one week. The anabolic signal (testosterone) was preserved even as the stress signal (cortisol) was activated — illustrating the important concept of hormonal balance, where the testosterone-to-cortisol ratio matters more than either hormone in isolation. A high ratio favors muscle building and recovery; a low ratio (more cortisol relative to testosterone) signals overreaching or overtraining.
The good news: with long-term consistent training, baseline cortisol levels tend to decrease. Regular exercisers develop a more resilient HPA (hypothalamic-pituitary-adrenal) axis, meaning they produce an appropriate cortisol response to stress but return to baseline more quickly. They also tend to sleep better, which is one of the most powerful natural regulators of cortisol.
Practical guidance: If you are experiencing symptoms of overtraining — persistent fatigue, poor sleep, mood changes, declining performance — your cortisol may be chronically elevated. Prioritizing rest days, sleep, and stress management is not weakness; it is hormonal intelligence.
Role of Cortisol
Cortisol regulates:
Energy mobilization
Blood glucose stability
Stress adaptation
.
Clinical Insight
Long-term exercise:
Reduces baseline cortisol
Improves HPA axis resilience
Enhances sleep quality
4. Thyroid Hormones and Metabolic Rate
The Thyroid's Role in Metabolism
The thyroid gland produces T4 (thyroxine), which is converted to the biologically active T3 (triiodothyronine) primarily in peripheral tissues like the liver and muscle. T3 is the main regulator of your basal metabolic rate (BMR) — how many calories your body burns at rest. It also governs mitochondrial activity, heart rate, body temperature, and cognitive function.
An underactive thyroid (hypothyroidism) slows metabolism, causes fatigue, promotes weight gain, and impairs physical performance. An overactive thyroid (hyperthyroidism) does the opposite, accelerating metabolism but at the cost of cardiovascular strain and muscle wasting.
How Exercise Influences Thyroid Function
Exercise has a bidirectional, favorable effect on thyroid health. In the short term, moderate-to-vigorous exercise produces mild increases in TSH (thyroid-stimulating hormone) and T4 levels. More importantly, regular exercise improves peripheral T4-to-T3 conversion, meaning more of your circulating thyroid hormone is converted into its active, metabolically useful form.
Sundus et al. (2025) conducted a systematic review and meta-analysis specifically examining long-term exercise-based interventions in hypothyroid patients. Their findings confirmed that consistent exercise improves thyroid function markers, reduces fatigue, and enhances metabolic rate — making physical activity a genuine therapeutic tool for hypothyroidism management, not merely a supplement to medication.
Adding another layer of complexity, Greenhill (2025) highlights that leptin — the satiety hormone produced by fat cells — directly interacts with the thyroid hormone axis to regulate energy expenditure in skeletal muscle. Exercise, by reducing body fat and modulating leptin signaling, may improve thyroid-muscle communication, helping to maintain metabolic rate even during caloric restriction. This finding has particular relevance for people who experience metabolic adaptation during weight loss programs.
EPOC: The Afterburn Effect
One of the most metabolically significant thyroid-related effects of exercise is the EPOC (Excess Post-Exercise Oxygen Consumption) — colloquially known as the "afterburn." After a high-intensity workout, your metabolic rate remains elevated for hours as your body restores oxygen levels, repairs tissue, and recalibrates hormone levels. HIIT is particularly effective at generating EPOC, making it a time-efficient strategy for improving both resting metabolic rate and overall caloric expenditure.
The more muscle mass you carry — maintained and built through resistance training — the higher your resting metabolic rate remains long-term, since muscle is metabolically more active than fat tissue.
Thyroid Function and Metabolism
T4 → T3 conversion regulates metabolic activity
T3 controls:
Basal metabolic rate
Mitochondrial function
Thermogenesis
5. Hormonal Integration: The Systems Biology of Exercise
Viewing each hormone in isolation understates the beauty of how they work together. Exercise orchestrates a coordinated hormonal symphony:
Insulin falls + glucagon rises → fat oxidation increases, liver glucose is mobilized
Testosterone + GH rise → muscle protein synthesis is activated, fat is broken down
Cortisol rises acutely → energy substrate availability is maintained; over time, resilience builds
Thyroid function improves → resting metabolism increases, mitochondrial efficiency improves
At the molecular level, two key signaling pathways govern much of this hormonal integration: AMPK (activated by exercise, promoting fat oxidation and glucose uptake) and mTOR (activated by anabolic signals like insulin, IGF-1, and amino acids, promoting muscle protein synthesis). Exercise intelligently activates both pathways — sequentially and contextually — in a way that no pharmaceutical can fully replicate.
The PGC-1α pathway serves as a master regulator of mitochondrial biogenesis — the process by which your cells build new mitochondria. Both endurance and resistance training stimulate PGC-1α, improving cellular energy efficiency and metabolic flexibility.
AMPK → Fat oxidation & glucose uptake
mTOR → Muscle protein synthesis
PGC-1α → Mitochondrial biogenesis
6. Clinical Applications of Exercise Hormones
For Diabetes and Insulin Resistance
Combine aerobic exercise (3–5 days/week, 30–45 minutes at moderate intensity) with resistance training (2–3 sessions/week). The aerobic component improves insulin sensitivity and cardiovascular health; resistance training builds muscle mass that acts as a long-term glucose reservoir. Timing exercise 60–90 minutes after a meal can blunt postprandial glucose spikes.
For Fat Loss and Obesity
Target the hormonal milieu of fat mobilization: lower insulin (achieved through exercise-induced glucose clearance), raise GH (through HIIT and compound resistance exercises), and support the thyroid axis (through consistent exercise that prevents metabolic adaptation). Avoid chronic overtraining, which elevates cortisol and promotes central fat storage.
For Aging and Longevity
The age-related decline in testosterone, GH, and thyroid function — along with increasing insulin resistance — can be significantly slowed by a well-designed exercise program. Resistance training 2–3 times per week preserves lean muscle mass (critical for both metabolic rate and functional independence), while regular aerobic activity maintains cardiovascular and hormonal health.
Optimal Weekly Exercise Plan
Zone 2 Aerobic (3–4 sessions, 30–45 min): Walking, cycling, swimming at conversational intensity — builds mitochondrial base, improves insulin sensitivity
Resistance Training (2–3 sessions): Compound lifts with progressive overload — stimulates testosterone, GH, and preserves muscle mass
HIIT (1–2 sessions): Interval sprints, circuit training — maximises GH response, EPOC, and metabolic rate
Aerobic (Zone 2): 3–4 sessions/week
Resistance Training: 2–3 sessions/week
HIIT: 1–2 sessions/week
7. Special Populations
Women: Estrogen interacts closely with insulin sensitivity, GH, and thyroid function. Exercise recommendations should account for menstrual cycle phase and, in perimenopausal and postmenopausal women, the decline in estrogen that accelerates insulin resistance and bone loss. Resistance training is especially valuable for postmenopausal women.
Older Adults: The anabolic response to exercise is somewhat blunted with age — a phenomenon called anabolic resistance — but it is not eliminated. Higher protein intake combined with resistance training can largely overcome this limitation. Exercise also improves circadian cortisol rhythms, which tend to dysregulate with aging.
People with Thyroid Disorders: Those with hypothyroidism should engage in regular, progressive exercise under medical supervision, as evidence supports improved thyroid function markers over time (Sundus et al., 2025). Those with hyperthyroidism should avoid very high-intensity exercise until thyroid levels are controlled, due to cardiac risk.
Exercise modalities and their specific hormonal and metabolic impacts:
Understanding how different types of exercise influence hormones and metabolism is key to designing a targeted training strategy for fat loss, muscle growth, insulin sensitivity, and long-term metabolic health. Each modality—Zone 2 aerobic training, resistance training, and HIIT—activates distinct hormonal pathways and produces unique metabolic outcomes.
1. Zone 2 Aerobic Exercise (Steady-State Cardio): The Foundation of Metabolic Health
Primary Hormonal Drivers: Insulin ↓, Glucagon ↑
Metabolic Effects:
Zone 2 aerobic exercise (moderate-intensity, conversational pace) is the most effective modality for improving fat oxidation and mitochondrial function. It enhances mitochondrial biogenesis, allowing cells to generate energy more efficiently while preferentially using fat as fuel.
Hormonal Adaptations:
Insulin Sensitivity: High → improves baseline glucose control and reduces insulin resistance
Glucagon Activity: Increased → promotes hepatic glucose output and fat utilization
Growth Hormone: Moderate elevation → supports fat metabolism
Testosterone: Minimal acute increase
Cortisol: Moderate (adaptive, not excessive)
Thyroid (T3) Activity: Moderate → supports metabolic efficiency
Clinical Insight:
Zone 2 training is ideal for type 2 diabetes, metabolic syndrome, and long-term fat loss, forming the aerobic base for metabolic flexibility.
2. Resistance Training (Strength Training): The Anabolic Engine
Primary Hormonal Drivers: Testosterone ↑, IGF-1 ↑
Metabolic Effects:
Resistance training is the most powerful stimulus for muscle hypertrophy and increased basal metabolic rate (BMR). By increasing lean muscle mass, it creates a long-term “metabolic sink” that enhances glucose disposal and energy expenditure—even at rest.
Hormonal Adaptations:
Testosterone: High acute increase → drives muscle protein synthesis
IGF-1: Elevated → promotes tissue repair and growth
Growth Hormone: High → supports fat loss and recovery
Insulin Sensitivity: Moderate to high → improved via increased muscle mass
Cortisol: Moderate → necessary for adaptation when balanced
Thyroid (T3) Activity: Moderate → supports metabolic rate
Clinical Insight:
Resistance training is essential for sarcopenia prevention, metabolic health, and sustainable fat loss, particularly in aging populations and insulin-resistant individuals.
3. HIIT (High-Intensity Interval Training): The Metabolic Accelerator
Primary Hormonal Drivers: Growth Hormone ↑↑, Catecholamines ↑
Metabolic Effects:
HIIT produces the most potent acute metabolic response, characterized by excess post-exercise oxygen consumption (EPOC)—the “afterburn effect”—which keeps metabolism elevated for hours after exercise.
Hormonal Adaptations:
Growth Hormone: Very high → drives lipolysis and metabolic remodeling
Catecholamines (Adrenaline/Noradrenaline): High → mobilize fat and glucose rapidly
Insulin Sensitivity: Very high → rapid glucose clearance from blood
Testosterone: Moderate increase
Cortisol: High (acute) → requires adequate recovery
Thyroid (T3) Activity: High → increases metabolic rate
Clinical Insight:
HIIT is highly effective for fat loss plateaus, improving insulin sensitivity, and time-efficient metabolic conditioning, but must be balanced to avoid chronic cortisol elevation.
Integrated Perspective: Matching Exercise to Hormonal Goals
For insulin resistance: Prioritize Zone 2 + resistance training
For fat loss: Combine HIIT (acute fat burn) + resistance (long-term metabolism)
For aging and muscle loss: Emphasize resistance training
For metabolic flexibility: Use all three modalities strategically
Key Takeaway
Each exercise modality acts as a targeted hormonal intervention:
Zone 2 → optimizes insulin and fat metabolism
Resistance training → drives anabolic hormones and muscle growth
HIIT → maximizes metabolic rate and fat-burning hormones
The most effective program is not choosing one—but strategically combining all three to create a comprehensive hormonal and metabolic advantage.
Exercise Is Endocrine Medicine: A Clinician’s Editorial Perspective
Exercise is not merely physical activity—it is a systemic endocrine intervention. Each session triggers coordinated hormonal signaling that regulates glucose metabolism, fat oxidation, muscle protein synthesis, and energy balance, functioning with a precision that rivals pharmacotherapy (Mennitti et al., 2024).
Insulin sensitivity improves immediately—even without weight loss. Through AMPK-mediated GLUT4 translocation, skeletal muscle becomes a powerful glucose sink, offering a non-pharmacological pathway to reverse insulin resistance and improve glycemic control in type 2 diabetes.
Glucagon is emerging as a multi-organ metabolic regulator. Beyond hepatic glucose output, it influences lipid metabolism and energy homeostasis, reframing its role in exercise physiology and metabolic disease (Lee et al., 2025).
Resistance training and HIIT act as natural anabolic therapies. They stimulate testosterone and growth hormone, enhance IGF-1 signaling, and improve androgen receptor sensitivity—critical for combating sarcopenia, frailty, and age-related metabolic decline.
Cortisol is not the enemy—chronic dysregulation is. Acute exercise-induced cortisol is adaptive, mobilizing energy substrates. However, persistent elevation from overtraining or poor recovery shifts the body toward catabolism, insulin resistance, and visceral fat accumulation.
Exercise optimizes thyroid function and metabolic rate. By improving peripheral T4-to-T3 conversion and mitochondrial efficiency, physical activity sustains basal metabolic rate and counters metabolic adaptation during weight loss (Sundus et al., 2025).
Hormonal effects are cumulative and synergistic. The integration of insulin, glucagon, anabolic hormones, and thyroid signaling enhances metabolic flexibility—a cornerstone of long-term cardiometabolic health.
Clinical takeaway: Exercise should be prescribed with the same intent as medication—dose, intensity, frequency, and progression matter—making it a foundational therapy for diabetes, obesity, aging, and endocrine dysfunction.
Frequently Asked Questions (FAQs)
1. Does exercise really increase testosterone naturally? Yes. Resistance training — especially compound movements involving large muscle groups — produces an acute testosterone spike and, with consistent training, improves androgen receptor sensitivity and reduces visceral fat that would otherwise convert testosterone to estrogen. While exercise-induced testosterone increases are modest compared to pharmaceutical therapy, they are clinically meaningful for long-term hormonal health (Mennitti et al., 2024).
2. Can exercise replace insulin medication for type 2 diabetes? Exercise is one of the most powerful tools for improving insulin sensitivity and managing blood glucose, but it should not replace insulin therapy without careful medical supervision. In early-stage type 2 diabetes or prediabetes, structured exercise combined with dietary changes may reduce or eliminate the need for medication in some individuals. Always consult your healthcare provider before adjusting medications.
3. Which type of exercise boosts metabolism the most? HIIT produces the greatest acute metabolic boost through the EPOC (afterburn) effect and strong growth hormone stimulation. However, resistance training builds the muscle mass that sustains a higher resting metabolic rate long-term. The most effective strategy combines both modalities, supported by a regular aerobic base.
4. Why do I feel mentally foggy and fatigued if I exercise too much? Overtraining chronically elevates cortisol, which impairs sleep, suppresses immune function, and can lower thyroid hormone activity. This creates a hormonal environment that drains mental and physical energy. Adequate rest, sleep, and progressive (not excessive) training loads are essential to maintain hormonal balance.
5. Is exercise beneficial for people with hypothyroidism? Yes. A systematic review and meta-analysis by Sundus et al. (2025) found that long-term exercise interventions improved thyroid function markers, reduced fatigue, and enhanced metabolic rate in hypothyroid patients. Exercise should complement — not replace — medical management, but it is a valuable and evidence-supported adjunct therapy.
6. How does exercise affect hormones differently in women versus men? Men tend to show larger acute testosterone spikes in response to resistance training, but women benefit equally from improvements in insulin sensitivity, GH responses, and cortisol regulation. In women, hormonal responses also interact with estrogen and progesterone levels across the menstrual cycle, with the follicular phase generally producing a more favorable anabolic environment.
7. How quickly do hormonal adaptations from exercise occur? Some benefits are immediate — a single session improves insulin sensitivity for 24–72 hours. Measurable improvements in resting cortisol, GH pulsatility, and GLUT4 expression typically emerge within 4–8 weeks of consistent training. More substantial changes in body composition, testosterone receptor sensitivity, and thyroid function develop over 3–6 months of sustained exercise.
Author’s Note
As a clinician in internal medicine, I have long observed a recurring pattern: patients often view exercise as optional—a lifestyle add-on rather than a therapeutic necessity. Yet, the science tells a very different story. Exercise is not simply about burning calories or improving appearance; it is one of the most powerful, evidence-based interventions we possess to modulate human physiology at a hormonal and molecular level.
This article was written to reframe exercise through a clinical lens—as endocrine medicine in motion. The hormonal adaptations discussed here—spanning insulin, glucagon, testosterone, growth hormone, cortisol, and thyroid function—are not abstract biochemical concepts. They represent real, measurable pathways through which structured physical activity can prevent, manage, and even reverse chronic metabolic diseases.
In my practice, I have seen patients improve glycemic control, regain functional strength, reduce medication dependence, and enhance overall quality of life through well-designed exercise interventions. These outcomes are not incidental—they are the predictable result of targeted physiological adaptation.
However, it is equally important to recognize that exercise is not a one-size-fits-all prescription. The optimal “dose” varies based on age, metabolic health, hormonal status, and clinical context. Just as we individualize pharmacological treatment, we must also personalize exercise strategies to maximize benefit while minimizing risk.
My goal is to bridge the gap between emerging scientific evidence and practical clinical application—empowering both healthcare professionals and informed individuals to use exercise with intention, precision, and consistency.
When applied correctly, exercise is not merely preventive medicine—it is transformative therapy.
Medical Disclaimer
The information in this article, including the research findings, is for educational purposes only and does not constitute medical advice, diagnosis, or treatment. Before starting an exercise program, you must consult with a qualified healthcare professional, especially if you have existing health conditions (such as cardiovascular disease, uncontrolled hypertension, or advanced metabolic disease). Exercise carries inherent risks, and you assume full responsibility for your actions. This article does not establish a doctor-patient relationship.
Related Articles
Why Aerobic Exercise Is the Most Powerful ‘Drug’ for Heart, Fat Loss & Longevity | DR T S DIDWAL
Exercise Unlocks a Hidden Glucose Pathway in Muscle — Independent of Insulin | DR T S DIDWAL
No Time to Train? Science-Backed Workouts That Deliver | DR T S DIDWAL
References
Greenhill, C. (2025). Leptin–thyroid hormone axis affects energy use in muscle. Nature Reviews Endocrinology, 21, 268. https://doi.org/10.1038/s41574-025-01103-1
Jaklová Dytrtová, J., Jakl, M., Jebavý, R., Máčová, L., Horníková, D., Novák, F., Vodička, P., Navrátil, T., Bičíková, M., Elsnicová, B., Žurmanová, J., & Galatík, F. (2026). Increase in testosterone and cortisol one week after repeated exercise in a cold environment. Frontiers in Physiology, 16, 1731242. https://doi.org/10.3389/fphys.2025.1731242
Lee, S. H., Park, H. Y., Yun, J. H., & Do, E. K. (2025). Glucagon in metabolic disease: A mini-review of emerging multi-organ roles beyond glycemic control. Frontiers in Endocrinology, 16, 1645041. https://doi.org/10.3389/fendo.2025.1645041
Li, S., Meng, Z., & Lin, J. (2025). Famsin and fasting adaptation: A glucagon connection. Cell Metabolism, 37(3), 561–563. https://doi.org/10.1016/j.cmet.2025.01.030
Mennitti, C., Farina, G., Imperatore, A., De Fonzo, G., Gentile, A., La Civita, E., Carbone, G., De Simone, R. R., Di Iorio, M. R., Tinto, N., Frisso, G., D'Argenio, V., Lombardo, B., Terracciano, D., Crescioli, C., & Scudiero, O. (2024). How does physical activity modulate hormone responses? Biomolecules, 14(11), 1418. https://doi.org/10.3390/biom14111418
Ramadan, W., Xirouchaki, C. E., & El-Gilany, A.-H. (2025). The comparative effects of high-intensity interval training and traditional resistance training on hormonal responses in young women: A 10-week intervention study. Sports, 13(3), 67. https://doi.org/10.3390/sports13030067
Sundus, H., Khan, S. A., Zaidi, S., Chhabra, C., Ahmad, I., & Khan, H. (2025). Effect of long-term exercise-based interventions on thyroid function in hypothyroidism: A systematic review and meta-analysis of randomized controlled trials. Complementary Therapies in Medicine, 92, 103196. https://doi.org/10.1016/j.ctim.2025.103196