Exercise Unlocks a Hidden Glucose Pathway in Muscle — Independent of Insulin
Discover how exercise lowers blood sugar without insulin. Learn the hidden muscle glucose pathway, GLUT4 activation, and benefits for type 2 diabetes.
EXERCISEDIABETES
Dr. T.S. Didwal, M.D.(Internal Medicine)
3/18/202612 min read
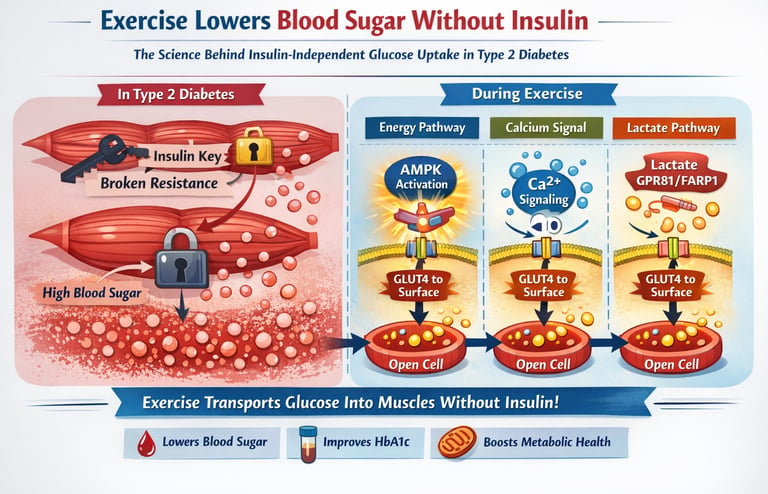
Exercise lowers blood sugar without insulin by activating muscle contraction pathways that move GLUT4 transporters to the cell surface. This allows glucose to enter muscle cells directly, even in insulin resistance. The effect begins within minutes and can improve glucose control for up to 24–48 hours after activity.
What if your body had a second, powerful way to lower blood sugar — one that works even when insulin fails? For millions living with type 2 diabetes, where insulin resistance blocks glucose from entering cells, this question is not theoretical — it is transformative. Emerging research in exercise physiology and metabolic health reveals that skeletal muscle contraction activates a completely separate pathway for glucose uptake, bypassing the defective insulin signal altogether (Richter et al., 2025).
At the center of this process is GLUT4 translocation, a mechanism traditionally associated with insulin action. However, during physical activity, contracting muscles stimulate AMP-activated protein kinase (AMPK) and calcium-dependent signaling pathways, which independently drive GLUT4 transporters to the cell membrane, allowing glucose to enter muscle cells efficiently — even in states of profound insulin resistance (Li et al., 2024; McGee & Hargreaves, 2024). This means that exercise lowers blood sugar within minutes, without requiring insulin to function properly.
Even more compelling, recent discoveries have expanded this paradigm. A 2026 study in Cell Research identified a novel lactate-mediated signaling pathway (GPR81/FARP1) that further enhances insulin-independent glucose uptake, particularly during high-intensity exercise (Niu et al., 2026). This positions exercise not merely as lifestyle advice, but as a form of molecular medicine capable of directly targeting the core defects of diabetes.
For patients and clinicians alike, the implication is profound: exercise is not just supportive therapy — it is a primary metabolic intervention. By activating multiple glucose-lowering pathways simultaneously, including AMPK activation, mitochondrial adaptation, and skeletal muscle glucose transport, physical activity offers a uniquely powerful strategy to improve glycemic control, reduce HbA1c, and combat the progression of metabolic disease (Peng et al., 2024).
Key Takeaways
Exercise lowers blood sugar without insulin
Activates GLUT4 translocation via multiple pathways
Works within minutes and lasts up to 48 hours
High-intensity exercise adds lactate-mediated benefits
Combined training provides maximum metabolic impact
Clinical pearls
1. The "Back Door" is Always Open
Scientific Tone: Contraction-stimulated GLUT4 translocation operates through an insulin-independent signaling pathway involving AMPK and CaMKII. This pathway remains functionally intact even in states of severe insulin resistance or receptor desensitization.
Think of insulin as the "front door" key to your cells. In Type 2 Diabetes, that lock is jammed. However, exercise is like a "back door" that doesn't need a key at all—the simple act of moving your muscles slides the door open manually.
2. Intensity "Unlocks" a Third Pathway
Scientific Tone: High-intensity exertion triggers the Lactate-GPR81-FARP1 axis. As discovered in 2026 (Niu et al.), lactate acts as a potent signaling ligand that amplifies glucose uptake beyond traditional aerobic thresholds.
That "burning" feeling in your muscles during a brisk climb or a fast walk isn't just waste; it’s a signal. That burn (lactate) actually tells your body to vacuum up even more sugar from your blood.
3. The "Sink" Size Matters
Scientific Tone: Resistance training induces muscular hypertrophy and increases the total expression of GLUT4 protein content. This expands the volumetric "glucose sink," improving the body's glycemia-clearing capacity during both active and basal states.
Your muscles are like sponges for sugar. By lifting weights or using resistance bands, you aren't just getting stronger—you are building a "bigger sponge" that can hold and process more blood sugar 24/7.
4. The 48-Hour "Afterburn" Window
Scientific Tone: A single bout of exercise induces a transient increase in post-exercise insulin sensitivity that can persist for 24 to 48 hours, driven by sustained AMPK activity and the replenishment of intramuscular glycogen stores.
One workout doesn't just lower your sugar while you're doing it. Your muscles stay "extra hungry" for sugar for up to two days afterward as they work to refuel and repair themselves.
5. Timing: The "Post-Prandial" Power Hour
Scientific Tone: Engaging in light mechanical activity (e.g., walking) within 30 minutes of carbohydrate ingestion blunts the post-prandial glucose peak by activating immediate translocation of GLUT4 before the insulin response is overwhelmed.
The best time to move is right after you eat. A short 15-minute walk after dinner catches the sugar as it enters your blood and shoves it into your muscles before it has a chance to spike your levels.
6. The "Anti-Inflammatory" Shield
Scientific Tone: Chronic exercise reduces systemic levels of pro-inflammatory cytokines (like TNF-α) that normally interfere with the insulin signaling cascade (IRS-1 phosphorylation). This helps "repair" the damaged insulin pathway over time.
Inflammation is like "noise" that prevents your cells from hearing insulin's signal. Regular exercise acts like a noise-canceling headset, helping your body finally "hear" the insulin you still produce, making your natural system work better again.
Exercise and Insulin-Independent Glucose Uptake: How Physical Activity Lowers Blood Sugar Without Insulin
The Hidden Way Exercise Lowers Blood Sugar
If you have type 2 diabetes or insulin resistance, you’ve likely been told to exercise regularly. But why does exercise lower blood sugar—even when insulin isn’t working properly?
The answer lies in a powerful biological mechanism: exercise activates glucose uptake in muscle cells without requiring insulin (Richter et al., 2025).
In type 2 diabetes, insulin signaling is impaired, meaning glucose cannot efficiently enter cells. This leads to elevated blood sugar levels and long-term complications. However, exercise bypasses this defect entirely, activating a separate pathway that allows muscles to absorb glucose directly.
Key takeaway: Exercise lowers blood sugar through insulin-independent pathways, making it one of the most effective strategies for managing diabetes.
What Is GLUT4 and Why Is It Critical for Blood Sugar Control?
Glucose cannot enter muscle cells without a transporter. The most important of these is GLUT4 (Glucose Transporter Type 4).
At rest, GLUT4 is stored inside muscle cells
After a meal, insulin activates GLUT4 translocation to the cell membrane
This allows glucose to move from blood into muscle
In insulin resistance, this pathway is impaired, leading to chronic hyperglycemia.
How Exercise Triggers GLUT4 Without Insulin
1. Contraction-Induced Glucose Uptake
During physical activity, muscle contraction activates an alternative pathway known as:
Contraction-mediated GLUT4 translocation
This pathway:
Works independently of insulin
Begins within minutes of exercise
Remains active for up to 24–48 hours
Importantly, insulin and exercise pathways are additive, meaning they work together to enhance glucose uptake (Richter et al., 2025).
Molecular Mechanisms: How Exercise Lowers Blood Sugar
AMPK: The Energy Sensor
Exercise increases energy demand, reducing ATP levels and activating AMP-activated protein kinase (AMPK).
AMPK stimulates GLUT4 translocation
Improves glucose uptake and fat metabolism
Effects persist even after exercise ends (McGee & Hargreaves, 2024)
Calcium Signaling Pathway
Muscle contraction releases calcium (Ca²⁺), activating CaMKII.
Independent of insulin and AMPK
Enhances GLUT4 movement to the membrane
Links mechanical contraction to metabolic control
(Li et al., 2024)
Rac1 and Cytoskeletal Remodeling
Exercise also activates Rac1, which reorganizes the cytoskeleton.
Facilitates GLUT4 vesicle docking
Improves efficiency of glucose transport
Supports sustained glucose uptake
(Richter et al., 2025)
New Discovery: Lactate Enhances Glucose Uptake (2026 Breakthrough)
Recent research published in Cell Research has transformed our understanding of exercise metabolism.
Scientists identified the GPR81/FARP1 signaling pathway, where:
Lactate acts as a signaling molecule (not waste)
Activates receptors (GPR81) on muscle cells
Triggers additional GLUT4 translocation
Clinical insight: High-intensity exercise produces more lactate, amplifying glucose uptake (Niu et al., 2026)
Why Exercise Type Matters for Blood Sugar Control
Different forms of exercise activate different metabolic pathways:
Aerobic Exercise (Walking, Cycling)
Activates AMPK pathway
Improves mitochondrial function
Reduces HbA1c over time
Resistance Training (Strength Exercise)
Increases muscle mass
Expands glucose storage capacity
Enhances long-term metabolic health
High-Intensity Interval Training (HIIT)
Activates lactate signaling pathway
Produces rapid GLUT4 translocation
High efficiency for glucose control
Combined Training (Best Approach)
Integrates aerobic + resistance benefits
Most effective for:
HbA1c reduction
Insulin sensitivity
Body composition
(Lan et al., 2025)
Beyond Glucose: Exercise Repairs Insulin Resistance
Exercise does more than bypass insulin—it helps restore it.
According to research in the World Journal of Diabetes:
Reduces inflammation
Improves lipid metabolism
Enhances beta-cell function
Restores insulin signaling pathways
(Peng et al., 2024)
Mechanisms by Which Exercise Lowers Blood Sugar (Beyond Insulin)
• Insulin-Mediated Pathway (Post-Meal State)
Triggered by food intake, insulin activates the PI3K–Akt signaling pathway, which promotes GLUT4 translocation to the muscle cell membrane, enabling glucose entry.
• Energy-Sensing Pathway (Exercise-Induced)
During exercise, depletion of cellular energy (ATP) activates AMP-activated protein kinase (AMPK). This stimulates GLUT4 movement to the cell surface independently of insulin.
• Contraction-Induced Calcium Pathway
Muscle contraction increases intracellular calcium (Ca²⁺), activating CaMKII (calcium/calmodulin-dependent protein kinase II). This pathway independently enhances GLUT4 translocation.
• Cytoskeletal Remodeling Pathway
Mechanical stress during exercise activates Rac1, a protein involved in cytoskeletal reorganization. This facilitates GLUT4 vesicle docking and fusion with the cell membrane.
• High-Intensity Lactate Signaling Pathway
Intense exercise increases lactate production, which activates the GPR81/FARP1 signaling pathway. This emerging pathway further enhances insulin-independent glucose uptake.
These pathways operate in parallel and synergistically, making exercise one of the most powerful tools for improving glucose control—even in significant insulin resistance.
Rethinking Glucose Control in Type 2 Diabetes
• A paradigm shift in diabetes care
Type 2 diabetes has long been viewed primarily as a disorder of insulin deficiency or resistance. However, modern exercise physiology reveals a critical truth: glucose regulation is not exclusively insulin-dependent. Skeletal muscle possesses an intrinsic, contraction-driven mechanism that allows glucose uptake even when insulin signaling is impaired.
• GLUT4: The central therapeutic target
At the core of this process is GLUT4 translocation, traditionally activated by insulin. Exercise, however, independently mobilizes GLUT4 to the cell surface via AMPK activation, calcium–CaMKII signaling, and cytoskeletal remodeling pathways, effectively bypassing the metabolic defect central to type 2 diabetes.
• Multiple pathways, one outcome
Rather than a single mechanism, exercise activates a redundant network of glucose-lowering pathways. Energy depletion stimulates AMPK; muscle contraction triggers calcium signaling; and structural adaptations involve Rac1-mediated cytoskeletal changes. This redundancy explains the robustness and reliability of exercise as a metabolic intervention.
• Emerging science: Lactate as a signaling molecule
Recent discoveries, particularly the GPR81/FARP1 signaling pathway, suggest that lactate is not merely a byproduct but a potent metabolic signal. High-intensity exercise amplifies glucose uptake through this pathway, adding a new dimension to exercise prescription.
• Beyond acute effects: Remodeling metabolism
Exercise is not just an acute glucose-lowering tool. Chronic training increases mitochondrial density, GLUT4 expression, and insulin sensitivity, addressing both the symptoms and root causes of metabolic dysfunction.
• Clinical implications: From adjunct to cornerstone therapy
Exercise should no longer be framed as supportive care. It is a first-line, mechanism-driven intervention capable of lowering HbA1c, improving cardiometabolic health, and reducing long-term complications.
• The bottom line
Every bout of physical activity activates molecular pathways that directly remove glucose from circulation. In an era of precision medicine, exercise remains the most accessible and biologically powerful therapy for type 2 diabetes.
Monitoring and Safety Considerations
While the insulin-independent nature of exercise-induced glucose uptake is a powerful therapeutic tool, it also means that blood sugar can fall during or after exercise — even without taking insulin. People with type 2 diabetes, especially those on medications such as sulfonylureas or insulin itself, should monitor blood glucose before, during, and after exercise, particularly when trying a new type or intensity. Always work with your healthcare team to integrate an exercise programme safely into your diabetes management plan.
Getting Started: A Gentle Framework
For those who are new to regular exercise or managing physical activity with type 2 diabetes, a practical approach based on the current evidence might look like this:
Start with 10–15 minutes of brisk walking after meals. Post-meal walks are particularly effective because they use GLUT4-mediated uptake to clear the glucose rise that follows eating.
Gradually build toward 150 minutes of moderate-intensity aerobic activity per week, as broadly recommended by diabetes organisations worldwide — a target grounded in the mechanistic evidence reviewed above.
Add two to three sessions of resistance exercise weekly, focusing on major muscle groups. Even bodyweight exercises (squats, lunges, push-ups) provide meaningful stimulation.
Consider brief high-intensity intervals once you have a fitness base — for example, alternating 30 seconds of faster effort with 90 seconds of recovery during walks or cycling.
Avoid prolonged sitting. Breaking up sedentary time with short movement breaks every 30 minutes has been shown to blunt post-meal blood sugar spikes.
Frequently Asked Questions
❓ FAQ 1: How quickly does exercise lower blood sugar?
The glucose-lowering effect of exercise begins within minutes of starting physical activity. As soon as your muscles begin contracting, AMPK is activated and GLUT4 transporters start moving to the cell surface. Blood glucose typically begins to fall within 10–20 minutes of moderate aerobic exercise, and the enhanced glucose uptake continues for hours after you stop. A single 30-minute walk can produce a meaningful reduction in post-meal blood sugar.
❓ FAQ 2: If I exercise, does that mean I can reduce or stop my diabetes medication?
Never change or stop diabetes medication without first discussing it with your doctor. However, regular exercise does improve insulin sensitivity and glucose control, and many people with type 2 diabetes find that sustained exercise allows their healthcare team to adjust — or in some cases reduce — their medication over time. This should always be a medically supervised process, with careful blood glucose monitoring.
❓ FAQ 3: What is the best type of exercise for blood sugar control?
The current evidence, as summarised by Lan et al. (2025), suggests that combining aerobic and resistance training produces the best overall outcomes for blood glucose control, insulin sensitivity, and metabolic health in type 2 diabetes. Aerobic exercise improves GLUT4 function and mitochondrial capacity; resistance training builds the muscle mass that gives you more glucose storage capacity. If you can only do one, both aerobic and resistance exercise independently improve blood sugar — so any movement is better than none.
❓ FAQ 4: Why does high-intensity exercise sometimes raise blood sugar before lowering it?
During very intense exercise, the body releases stress hormones such as adrenaline and cortisol that temporarily stimulate the liver to release stored glucose into the bloodstream. This can cause a brief rise in blood sugar during or immediately after a hard effort. However, in the hours that follow, the powerful GLUT4-mediated uptake and lactate-activated GPR81 pathway described by Niu et al. (2026) typically result in a sustained and often significant reduction in blood glucose. This pattern is more common in people on insulin and should be discussed with your care team.
❓ FAQ 5: Can exercise help if I have been diagnosed with type 2 diabetes for a long time?
Yes. Because the contraction-activated GLUT4 translocation pathway is independent of insulin signalling, it remains largely intact even in long-standing type 2 diabetes with significant insulin resistance. The exercise-induced pathway bypasses the faulty insulin receptor signalling and directly moves glucose into muscle cells. Additionally, as reviewed by Peng et al. (2024), regular exercise initiates repairs to the insulin signalling machinery itself over time, offering benefits that compound with sustained engagement.
❓ FAQ 6: What does GLUT4 translocation actually mean in plain language?
Imagine GLUT4 transporters as revolving doors that let glucose enter a room (the muscle cell). In a resting, insulin-resistant muscle, most of these revolving doors are stored in a back room and not in use. When you exercise, a molecular signal goes out: 'Move the doors to the entrance!' The GLUT4 proteins travel from their storage compartment to the outer membrane of the cell and insert themselves as working channels. Glucose then flows through them from the bloodstream into the cell, lowering your blood sugar. When you stop exercising, the doors are gradually pulled back inside — which is why the effect is temporary and regular exercise is needed to maintain it.
❓ FAQ 7: How does the new lactate discovery change exercise recommendations?
The discovery by Niu et al. (2026) that lactate activates the GPR81/FARP1 signalling pathway — providing a third insulin-independent route for glucose uptake — adds scientific weight to the inclusion of higher-intensity exercise in diabetes management programmes. It does not mean that only intense exercise is beneficial; moderate exercise remains valuable through AMPK and calcium pathways. However, it does suggest that periodically pushing to a higher effort level — where muscles produce more lactate — may activate additional molecular mechanisms that amplify glucose clearance. This is one reason why HIIT protocols have shown such impressive results in clinical trials for type 2 diabetes.
Author’s Note
As a physician working at the intersection of metabolic disease, exercise physiology, and cardiometabolic health, I have seen firsthand how the narrative around type 2 diabetes is evolving. For decades, clinical management has focused predominantly on pharmacotherapy aimed at improving insulin secretion or sensitivity. While these approaches remain essential, emerging evidence makes one point unmistakably clear: exercise is not merely supportive—it is mechanistically therapeutic.
What distinguishes physical activity from most pharmacological interventions is its ability to activate multiple, overlapping biological pathways simultaneously. Through mechanisms such as GLUT4 translocation, AMPK activation, and contraction-mediated signaling, exercise enables skeletal muscle to uptake glucose independently of insulin, offering a powerful advantage in states of insulin resistance. The recent identification of the GPR81/FARP1 signaling pathway further expands our understanding, highlighting how exercise intensity can modulate metabolic responses at a molecular level.
In routine practice, one of the most important observations is this: even a single session of moderate exercise can significantly reduce postprandial glucose levels, often within hours. This effect is particularly valuable in patients with poorly controlled diabetes or those experiencing therapeutic inertia. Moreover, consistent engagement in both aerobic and resistance training not only improves glycemic control (reflected in reductions in HbA1c), but also addresses sarcopenia, visceral adiposity, and cardiovascular risk—key drivers of long-term morbidity.
However, it is equally important to individualize exercise prescriptions. Patients on insulin or insulin secretagogues require careful monitoring to avoid hypoglycemia, and those with comorbidities must follow tailored programs.
Ultimately, the goal is not just to treat diabetes, but to restore metabolic flexibility. Exercise remains one of the most potent, accessible, and underutilized tools we have to achieve this.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Individual circumstances vary, and treatment decisions should always be made in consultation with qualified healthcare professionals.
Related Articles
Is Your Heart at Risk? How the TG/HDL Ratio Can Warn You Early | DR T S DIDWAL
The Metabolic Triad: Why Diabetes, Obesity & CVD Are One Epidemic | DR T S DIDWAL
References
Lan, Y., Wang, Y., Wu, R., & Lv, P. (2025). Optimizing exercise for type 2 diabetes management: Comparative insights from aerobic, resistance, interval and combined training protocols. Metabolites, 15(11), 739. https://doi.org/10.3390/metabo15110739
Li, X., Zhang, Y., Wang, H., Liu, J., & Chen, Z. (2024). Exercise-induced molecular adaptations in skeletal muscle and their role in metabolic health. Journal of Exercise Science & Fitness, 22(4), 123–135. https://doi.org/10.1016/j.jesf.2024.06.004
McGee, S. L., & Hargreaves, M. (2024). Exercise performance and health: Role of GLUT4. Free Radical Biology and Medicine, 224, 479–483. https://doi.org/10.1016/j.freeradbiomed.2024.09.004
Niu, Y., Hu, S., Zhang, Y., et al. (2026). Lactate-activated GPR81/FARP1 signaling drives insulin-independent glucose uptake and metabolic control. Cell Research, 36, 137–151. https://doi.org/10.1038/s41422-025-01207-3
Peng, C. J., Chen, S., Yan, S. Y., Zhao, J. N., Luo, Z. W., Qian, Y., & Zhao, G. L. (2024). Mechanism underlying the effects of exercise against type 2 diabetes: A review on research progress. World Journal of Diabetes, 15(8), 1704–1711. https://doi.org/10.4239/wjd.v15.i8.1704
Richter, E. A., Bilan, P. J., & Klip, A. (2025). A comprehensive view of muscle glucose uptake: Regulation by insulin, contractile activity, and exercise. Physiological Reviews, 105(3), 1867–1945. https://doi.org/10.1152/physrev.00033.2024