How SCFAs From Gut Bacteria Boost Metabolic Health
Can your gut bacteria control weight and blood sugar? Learn how SCFAs shape metabolism, inflammation, and long-term metabolic health.
NUTRITIONMETABOLISM
Dr. T.S. Didwal, M.D.(Internal Medicine)
2/26/202615 min read

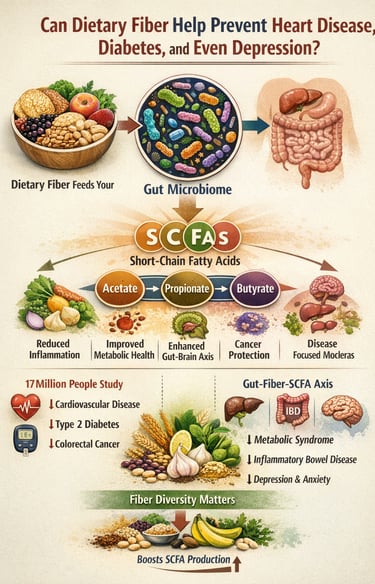
What if the most powerful tool for preventing heart disease, diabetes, colorectal cancer, and even depression isn’t a new drug — but the fiber already sitting on your plate?
For decades, dietary fiber was framed as little more than a digestive aid. Today, cutting-edge microbiome science tells a far more profound story. The fibers we consume are not simply roughage; they are metabolic substrates that feed the gut microbiome, reshape microbial diversity, and drive the production of short-chain fatty acids (SCFAs) — acetate, propionate, and butyrate — potent signaling molecules that regulate inflammation, insulin sensitivity, lipid metabolism, immune function, and even brain chemistry (Delzenne et al., 2025; Mukhopadhya & Louis, 2025).
Large-scale population data now reinforce these mechanistic insights. An umbrella review analyzing over 17 million individuals found that higher dietary fiber intake is consistently associated with lower all-cause mortality, reduced cardiovascular disease, decreased type 2 diabetes incidence, and diminished colorectal cancer risk (Veronese et al., 2025). Meanwhile, disease-focused molecular reviews show that impaired SCFA signaling is linked to metabolic syndrome, inflammatory bowel disease, and neuropsychiatric disorders — positioning the gut-fibre-SCFA axis as a master regulator of systemic health (Zhang et al., 2023).
Importantly, emerging evidence suggests that fiber diversity — not merely quantity — enhances microbial cross-feeding and synergistically amplifies SCFA production, particularly in metabolically compromised individuals (Galeano-Garcia et al., 2025).
In short, dietary fiber is no longer a peripheral nutrient. It is a cornerstone of precision nutrition, microbiome modulation, and evidence-based disease prevention — with implications that extend far beyond the gut
Clinical Pearls:
1. The "Diversity Over Dose" Rule
Scientific Insight: Research (Galeano-Garcia et al., 2025) shows that mixing fiber types creates a "synergistic boost." Different bacteria eat different fibers; when they work together, they produce more Short-Chain Fatty Acids (SCFAs) than they would alone.
Think of your gut like a crowded city. If you only provide one type of food (like only eating apples), only one group of people gets fed. If you provide a buffet of garlic, oats, beans, and seeds, the whole city thrives. Aim for 30 different plant types per week to keep the peace.
2. Butyrate: The Gut’s "Repair Cream"
Scientific Insight: Butyrate is the primary energy source for colonocytes (lining cells) and acts as a histone deacetylase (HDAC) inhibitor, which helps prevent DNA damage and cancer.
Butyrate is like a "premium fuel" and "repair cream" combined for your colon. To get more of it, eat resistant starch—potatoes that have been cooked and then cooled, green bananas, or lentils. This keeps your gut wall strong and prevents "leaks."
3. The 7-Gram "Safety Net"
Scientific Insight:The Veronese et al. (2025) umbrella review found that increasing fiber by just 7 to 8 grams per day significantly reduces the risk of chronic disease and all-cause mortality.
You don't have to overhaul your entire life overnight. Adding just one cup of raspberries or half a cup of black beans to your daily routine provides that "7-gram safety net" that statistically lowers your risk of heart disease and diabetes.
4. Precision Propionate for Heart Health
Scientific Insight: Beta-glucans (found in oats and barley) are specifically fermented into propionate, which travels to the liver to inhibit cholesterol synthesis and improve insulin sensitivity.
Not all fiber is for "regularity." Some fiber is "heart medicine." Eating a bowl of oatmeal or pearl barley is like sending a chemical messenger to your liver telling it to slow down cholesterol production. It’s nature’s version of a metabolic regulator.
5. The Polyphenol "Fiber-Partner"
Scientific Insight: Polyphenols (the colorful pigments in plants) are often bound to dietary fiber. When bacteria ferment the fiber, they "unlock" these polyphenols, converting them into highly bioavailable metabolites that lower systemic inflammation.
Colour is a signal for medicine. The "darkness" of a blackberry or the "red" of an onion isn't just for show; those colors are polyphenols. When you eat them with fiber, your gut bacteria turn them into powerful anti-inflammatory tools. Fiber is the "shuttle," and polyphenols are the "passengers" that protect your brain and heart.
1. The Gut Microbiome and Dietary Fibers: Implications in Obesity, Cardiometabolic Diseases, and Cancer
A comprehensive review by Delzenne et al. (2025) synthesises decades of mechanistic and epidemiological research on dietary fiber's effects through the gut microbiome. The authors make a compelling argument that the benefits of dietary fiber are not universal or automatic — they are profoundly dependent on the composition of an individual's gut microbiota.
The review explains that different types of dietary fibers — from inulin and fructooligosaccharides (FOS) to resistant starch and pectin — selectively nourish distinct communities of bacteria. These bacteria, in turn, ferment fibers into SCFAs (primarily acetate, propionate, and butyrate), which then circulate through the bloodstream and interact with host cells in far-reaching ways. In the context of obesity, SCFAs help regulate appetite hormones like GLP-1 and PYY, improve insulin sensitivity, and reduce fat accumulation. For cardiovascular health, propionate in particular appears to lower cholesterol synthesis in the liver and reduce blood pressure through free fatty acid receptor signaling.
In cancer biology, the study highlights the role of butyrate as a histone deacetylase (HDAC) inhibitor — a mechanism that can silence oncogenes and restore normal cell cycle regulation in colorectal epithelial cells. The review also acknowledges critical gaps: fiber type, dose, and microbiome baseline all interact to determine outcomes, explaining why clinical fiber trials sometimes yield inconsistent results.
Key Takeaway: The health benefits of dietary fiber are mediated predominantly through the gut microbiome and its SCFA output. Individual variability in microbiota composition means fiber type and baseline gut health must both be considered when making dietary recommendations.
2. New Insights Into Synergistic Boosts in SCFA Production Across Health Conditions Induced by a Fiber Mixture
Galeano-Garcia et al. (2025) | Nutrients
One of the most exciting applied studies of 2025, this research from Galeano-Garcia et al. (2025) moved beyond the question of whether fiber helps and asked a far more nuanced question: Does combining different types of dietary fiber produce synergistic SCFA benefits greater than the sum of its parts?
Using both in vitro fermentation models and human fecal inoculation experiments stratified across different health conditions — including healthy individuals, those with metabolic syndrome, and individuals with inflammatory bowel disease — the researchers tested a proprietary fiber mixture against individual fiber components. The results were striking. Not only did the fiber mixture consistently outperform individual fibers in SCFA yield, but the degree of synergy varied meaningfully by health condition. Individuals with metabolic syndrome, whose microbiomes are often dysbiotic and less efficient at fiber fermentation, showed particularly robust synergistic responses when given the mixture, suggesting that fiber diversity may be especially therapeutic precisely when gut microbial diversity is most compromised.
The mechanistic explanation centers on microbial cross-feeding: certain bacteria that ferment one type of fiber produce metabolic byproducts that serve as substrates for other bacteria to ferment complementary fibers. This ecological cascade amplifies SCFA production beyond what any single fiber could achieve alone. The study has profound implications for functional food and supplement design, pointing toward personalized, multi-fiber formulations as a next-generation approach.
Key Takeaway: Mixing dietary fiber types — rather than consuming a single fiber source — creates synergistic boosts in SCFA production, particularly in individuals with compromised gut health. Dietary fiber diversity may be as important as fiber quantity.
3. The Impact of Dietary Fiber Consumption on Human Health: An Umbrella Review of Evidence from 17,155,277 Individuals
When it comes to sheer evidential weight, no study in this collection comes close to the umbrella review by Veronese et al. (2025).which synthesizes the findings from multiple systematic reviews and meta-analyses — making it the highest possible tier of observational evidence. This one drew from data representing over 17 million individuals across dozens of health outcomes.
The results were sweeping. High dietary fiber intake was associated with statistically significant reductions in all-cause mortality, cardiovascular disease incidence and mortality, type 2 diabetes incidence, colorectal cancer risk, and a range of other chronic conditions. Dose-response analyses revealed that even modest increases in daily fiber intake — as little as 7 to 8 grams per day above baseline — corresponded to meaningful reductions in disease risk. The authors also observed that the effects of fiber were consistent across sexes, age groups, and geographic regions, suggesting that fiber's protective mechanisms are broadly applicable rather than population-specific.
Importantly, this review also evaluated fiber's impact on mental health outcomes, finding associations between higher fiber intake and reduced risk of depression, though the authors noted this literature is still maturing. The review strengthens the case for current dietary fiber guidelines and suggests that raising global fiber intake — which falls far short of recommended levels in most Western populations — could yield enormous public health dividends.
Key Takeaway: In the largest evidence synthesis on this topic to date, high dietary fiber intake was robustly associated with reduced all-cause mortality, cardiovascular disease, type 2 diabetes, and cancer. Even small increases in daily fiber intake produce measurable health benefits at a population level.
4. Gut Microbiota-Derived Short-Chain Fatty Acids and Their Role in Human Health and Disease
If Delzenne et al. (2025) provided the bird's eye view of fiber's microbiome effects, Mukhopadhya and Louis (2025) zoomed in to deliver the most detailed and current molecular account of how SCFAs actually function in the body. Published in the same high-impact journal, this review is an essential mechanistic companion piece.
The authors systematically dissect the roles of the three major SCFAs: acetate, propionate, and butyrate. Acetate, the most abundant SCFA, serves as an energy substrate and immune modulator, circulating systemically and crossing the blood-brain barrier where it influences appetite regulation via the hypothalamus. Propionate acts primarily in the liver, where it can inhibit cholesterol synthesis and modulate gluconeogenesis. Butyrate, the primary energy source for colonocytes, exhibits the most dramatic effects on colonic health — maintaining the intestinal epithelial barrier, suppressing inflammation via NF-κB pathway inhibition, and inducing apoptosis in colorectal cancer cells.
Mukhopadhya and Louis also address the underappreciated diversity of SCFA-producing bacteria, emphasizing that not all gut bacteria are equally capable of fiber fermentation. Keystone species like Faecalibacterium prausnitzii, Roseburia intestinalis, and Akkermansia muciniphila are highlighted as critical mediators of butyrate production. This has clinical relevance: depletion of these species in dysbiosis conditions (from antibiotic use, poor diet, or chronic illness) can dramatically reduce SCFA output even when fiber intake is adequate.
Key Takeaway: SCFAs are not passive byproducts of fermentation but active signaling molecules with distinct, well-characterized roles in metabolism, immunity, and gut barrier integrity. The diversity and abundance of SCFA-producing bacteria is as important as the SCFAs themselves.
5. Effects of Dietary Fibers on Short-Chain Fatty Acids and Gut Microbiota Composition in Healthy Adults: A Systematic Review
This systematic review by Vinelli et al. (2022) remains foundational for understanding how specific dietary fibers differentially shape the gut microbiome and SCFA production in healthy adults. The review synthesized data from randomized controlled trials (RCTs) and observational studies focusing on fibers including inulin, FOS, guar gum, pectin, beta-glucan, psyllium, and resistant starch.
Key findings include the strong evidence supporting inulin-type fructans as potent prebiotics that selectively amplify bifidobacteria and increase fecal SCFA concentrations — particularly acetate and propionate. Resistant starch, in contrast, showed a stronger association with butyrate production, largely mediated through Ruminococcus bromii and subsequent cross-feeding to butyrate-producing species. Beta-glucan from oats demonstrated particularly robust effects on propionate levels, which aligns mechanistically with its established cholesterol-lowering effects.
The review also highlighted significant heterogeneity across trials, attributable to differences in fiber dose, food matrix, participant baseline microbiota, and study duration — underscoring that fiber science requires more sophisticated, personalized study designs to generate clinically actionable guidance. Despite this variability, the overall signal for fiber-driven SCFA augmentation was consistent and robust.
Key Takeaway: Different dietary fibers produce distinct SCFA profiles and selectively enrich different bacterial communities. Matching fiber type to desired physiological outcome (e.g., butyrate for gut integrity vs. propionate for cholesterol lowering) represents a rational approach to precision nutrition.
6. Short-Chain Fatty Acids in Diseases
Zhang et al. (2023) provided an expansive disease-focused account of SCFA biology, cataloguing the evidence across a remarkable breadth of conditions including inflammatory bowel disease, colorectal cancer, metabolic syndrome, type 2 diabetes, non-alcoholic fatty liver disease (NAFLD), cardiovascular disease, and — perhaps most provocatively — neurological and psychiatric conditions including Alzheimer's disease, Parkinson's disease, autism spectrum disorder, and depression.
The gut-brain axis features prominently in this review. The authors synthesize evidence that SCFAs, particularly butyrate and acetate, influence brain function through multiple routes: direct transport across the blood-brain barrier, vagal nerve signaling, modulation of microglial activation, and regulation of serotonin synthesis in enterochromaffin cells. In rodent models, SCFA supplementation has demonstrated antidepressant and anxiolytic effects — findings that, while requiring human validation, point to the gut microbiome as a meaningful contributor to mental health.
In metabolic disease, Zhang et al. present compelling evidence that reduced SCFA signaling through G-protein coupled receptors GPR41 and GPR43 is a consistent feature of insulin-resistant states, positioning SCFA deficiency — not merely its consequences — as a driver of metabolic dysfunction. The review also examines the therapeutic potential of SCFA supplementation itself, noting that direct administration of butyrate or its prodrugs has shown promise in early clinical trials for IBD and colorectal cancer.
Key Takeaway: SCFAs are implicated across a strikingly diverse range of chronic diseases — from metabolic and inflammatory conditions to neuropsychiatric disorders — suggesting that the gut-fibre-SCFA axis is a master regulator of whole-body health, not merely a localized digestive mechanism.
From Science to Table: Practical Fiber Guidance
Given what this research collectively establishes, how should individuals and clinicians act? Several evidence-based principles emerge:
Prioritize fiber diversity over any single source. Rotating between inulin-rich foods (garlic, onion, leeks), resistant starch sources (cooked-and-cooled potatoes, green bananas, legumes), beta-glucan foods (oats, barley), and pectin-rich fruits (apples, citrus) mirrors the synergistic fiber mixture approach that Galeano-Garcia et al. (2025) showed to outperform single-fiber consumption.
Increase fiber intake gradually. Rapid increases can cause gas and bloating as the microbiome adapts. A gradual increase of 3-5 grams per week is typically well tolerated.
Aim for 25-38 grams per day. Most adults in Western countries consume only 10-15 grams daily — far below recommendations. Even modest increases of 7-8 grams per day, as Veronese et al. (2025) showed, produce measurable risk reductions.
Support SCFA-producing bacteria. Foods and lifestyles that preserve keystone species like Faecalibacterium prausnitzii and Akkermansia muciniphila — including fermented foods, adequate sleep, and reduced antibiotic exposure — amplify the benefits of dietary fiber, as Mukhopadhya and Louis (2025) emphasized.
Consider whole-food sources over supplements. The food matrix shapes how fiber is fermented and absorbed, and whole foods typically deliver fiber alongside polyphenols, vitamins, and minerals that may further synergize with SCFA-mediated pathways.
Short-chain fatty acids are not nutritional side notes — they are central metabolic regulators. Produced through microbial fermentation of dietary fiber, SCFAs integrate gut ecology with systemic physiology, influencing insulin sensitivity, inflammatory tone, mitochondrial efficiency, and cardiometabolic risk. The emerging evidence reframes fiber not merely as a digestive aid, but as a strategic substrate for metabolic signaling. In an era dominated by pharmacologic solutions for obesity and Type 2 diabetes, optimizing SCFA production through dietary diversity represents a low-cost, biologically elegant intervention grounded in molecular science. The clinical implication is clear: sustainable metabolic health begins not only with macronutrient quantity, but with microbial nourishment.
Here is the 30-Plant Diversity Checklist organized by functional fiber and nutrient groups. Aim to check off items from each category throughout the week to maximize your gut’s production of Short-Chain Fatty Acids (SCFAs).
1. Inulin & FOS (Prebiotics)
Focus: Boosts Bifidobacteria and Acetate production.
Garlic
Onions
Leeks
Asparagus
Chicory root
Jerusalem artichokes
2. Resistant Starch
Focus: The "King of Butyrate" for gut lining repair.
Potatoes (Cooked and cooled)
Green bananas / Plantains
Lentils
White beans (Cannellini, Navy)
Chickpeas
Cashews
3. Beta-Glucans
Focus: Heart health and Propionate production.
Oats (Steel-cut or rolled)
Barley
Shiitake mushrooms
Oyster mushrooms
Reishi mushrooms
4. Pectins & Soluble Fibers
Focus: Cholesterol management and blood sugar stability.
Apples (with skin)
Pears
Citrus fruits (Grapefruit, Oranges)
Carrots
Apricots
5. Polyphenol-Rich "Color" Plants
Focus: Anti-inflammatory "passengers" for fiber shuttles.
Blueberries / Blackberries
Red Onion
Dark Chocolate (85%+ cocoa)
Green Tea / Hibiscus Tea
Red Grapes
6. Cruciferous & Sulfur-Rich Vegetables
Focus: Detoxification and diversity.
Broccoli / Broccolini
Cauliflower
Brussels sprouts
Kale
Radishes
7. Seeds, Nuts & Whole Grains
Focus: Healthy fats and insoluble "bulking" fiber.
Chia seeds
Flaxseeds (Ground)
Walnuts
Pumpkin seeds (Pepitas)
Quinoa
Buckwheat
Rye / Farro
Frequently Asked Questions (FAQs)
Q1: What are short-chain fatty acids (SCFAs) and why are they important?
Short-chain fatty acids are organic acids — primarily acetate, propionate, and butyrate — produced when gut bacteria ferment dietary fiber. Far from being mere waste products, SCFAs function as signaling molecules that regulate immune function, metabolism, inflammation, gut barrier integrity, and even brain chemistry. As Mukhopadhya and Louis (2025) detail, each SCFA has distinct physiological roles: butyrate fuels colonocytes and suppresses colorectal cancer cell growth; propionate modulates cholesterol synthesis in the liver; acetate influences appetite regulation via the hypothalamus and provides systemic energy.
Q2: Does the type of dietary fiber I consume actually matter?
Yes, significantly. Vinelli et al. (2022) clearly demonstrated that different fibers produce distinct SCFA profiles and selectively nourish different bacterial communities. Inulin and FOS preferentially boost bifidobacteria and propionate/acetate production; resistant starch drives butyrate synthesis; beta-glucan from oats is particularly associated with propionate. Galeano-Garcia et al. (2025) further showed that consuming a mixture of fibers produces synergistic SCFA boosts that surpass any single fiber alone — making dietary fiber diversity a priority, not just total quantity.
Q3: How quickly can dietary fiber changes affect the gut microbiome?
Interestingly, the gut microbiome can begin responding to significant dietary changes within 24 to 48 hours, though stable, lasting changes to microbiome composition typically require weeks to months of sustained dietary shifts. Vinelli et al. (2022) found that most clinical trials showing robust SCFA and microbiome changes ran for 4 to 12 weeks of consistent fiber supplementation or dietary modification. Starting with gradual increases in fiber diversity and maintaining them over time is the most evidence-aligned approach.
Q4: Can dietary fiber help with weight management and metabolic disease?
Strongly yes, based on multiple levels of evidence. Delzenne et al. (2025) outline the mechanisms: SCFAs from fiber fermentation stimulate release of satiety hormones GLP-1 and PYY, slow gastric emptying, improve insulin sensitivity, and reduce hepatic fat accumulation. The umbrella review by Veronese et al. (2025) — drawing on data from over 17 million individuals — found statistically significant associations between high fiber intake and reduced risk of type 2 diabetes, metabolic syndrome, and cardiovascular disease. Zhang et al. (2023) additionally note that impaired SCFA signaling through GPR41 and GPR43 receptors is a feature of insulin resistance, suggesting SCFA deficiency may be causally involved, not merely correlational.
Q5: Is there evidence that dietary fiber benefits mental health?
Emerging evidence increasingly supports this connection, though the literature is still maturing compared to metabolic outcomes. Zhang et al. (2023) present a detailed analysis of how SCFAs influence the gut-brain axis: butyrate and acetate cross the blood-brain barrier, modulate microglial activation, regulate neuroinflammation, and influence serotonin synthesis in enteric neurons. Veronese et al. (2025) found associations between higher fiber intake and reduced depression risk in their umbrella review. Rodent models using SCFA supplementation have shown antidepressant and anxiolytic effects. While human RCT data specifically targeting mental health outcomes remain limited, the mechanistic and epidemiological signal is compelling.
Q6: Who benefits most from increasing dietary fiber intake?
While high fiber intake appears broadly beneficial across populations (Veronese et al., 2025), certain groups appear to benefit particularly. Galeano-Garcia et al. (2025) found that individuals with metabolic syndrome — whose gut microbiomes are often dysbiotic — showed the largest synergistic SCFA responses to fiber mixtures, suggesting that fiber diversity may be most therapeutically important precisely when gut health is most compromised. Individuals with inflammatory bowel disease, colorectal cancer risk factors, or insulin resistance also appear to stand to gain substantially from optimizing fiber intake and type, as documented across Delzenne et al. (2025) and Zhang et al. (2023).
Q7: Should I take fiber supplements or get fiber from whole foods?
Whole-food sources are generally preferable to isolated fiber supplements, though supplements have a role in specific clinical scenarios. Whole foods deliver fiber within a food matrix alongside polyphenols, vitamins, minerals, and additional phytochemicals that may synergize with SCFA-mediated pathways and independently support gut microbiome health. Isolated fiber supplements (such as inulin powders or psyllium husks) can meaningfully increase intake and have demonstrated efficacy in clinical trials (Vinelli et al., 2022), but they typically provide a narrower fiber type profile. For individuals with digestive conditions or those unable to achieve adequate intake through diet alone, fiber supplements — ideally combining multiple fiber types — represent a practical adjunct supported by the synergy data from Galeano-Garcia et al. (2025).
Authors’ Note
This editorial synthesizes findings from high-impact peer-reviewed research published between 2022 and 2025 in leading journals including Nature Reviews Microbiology, Clinical Nutrition, Nutrients, and Cell Communication and Signaling. The discussion integrates mechanistic microbiome science, large-scale epidemiological data, and clinical implications related to dietary fiber, gut microbiota diversity, and short-chain fatty acid (SCFA) biology.
The purpose of this article is educational: to translate complex molecular and population-level research into clinically relevant insights for healthcare professionals and informed readers. While the evidence supporting dietary fiber’s role in cardiometabolic, inflammatory, oncologic, and neurobiological health is substantial and rapidly expanding, nutrition science remains dynamic. Individual responses to dietary fiber may vary based on baseline microbiome composition, genetics, metabolic status, and underlying medical conditions.
This article does not constitute individualized medical advice. Patients with gastrointestinal disorders (such as inflammatory bowel disease, irritable bowel syndrome, or post-surgical conditions) or metabolic disease should consult a qualified healthcare professional before making substantial dietary changes.
The author declares no conflicts of interest related to the content presented.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Individual circumstances vary, and treatment decisions should always be made in consultation with qualified healthcare professionals.
Related Articles
Can Omega-3 Boost Muscle Protein Synthesis? What the Latest Research Reveals | DR T S DIDWAL
Beyond the Low-Fat Myth: 6 New Studies Redefining Dietary Fat and Heart Health | DR T S DIDWAL
Can Plant-Based Polyphenols Lower Biological Age? | DR T S DIDWAL
Time-Restricted Eating: Metabolic Advantage or Just Fewer Calories? | DR T S DIDWAL
Can You Revitalize Your Immune System? 7 Science-Backed Longevity Strategies | DR T S DIDWA
References
Delzenne, N. M., Bindels, L. B., Neyrinck, A. M., & Walter, J. (2025). The gut microbiome and dietary fibres: implications in obesity, cardiometabolic diseases and cancer. Nature Reviews Microbiology, 23(4), 225-238. https://doi.org/10.1038/s41579-024-01108-z
Galeano-Garcia, G. S., Chen, T., Engen, P. A., Keshavarzian, A., Hamaker, B. R., & Cantu-Jungles, T. M. (2025). New Insights into Synergistic Boosts in SCFA Production Across Health Conditions Induced by a Fiber Mixture. Nutrients, 17(24), 3904. https://doi.org/10.3390/nu17243904
Mukhopadhya, I., & Louis, P. (2025). Gut microbiota-derived short-chain fatty acids and their role in human health and disease. Nature Reviews Microbiology, 23, 635-651. https://doi.org/10.1038/s41579-025-01183-w
Veronese, N., Gianfredi, V., Solmi, M., Barbagallo, M., Dominguez, L. J., Mandata, C., Di Palermo, C., Carruba, L., Solimando, L., Stubbs, B., Castagna, A., Maggi, S., Zanetti, M., Al-Daghri, N., Nucci, D., Gosling, C., & Fontana, L. (2025). The impact of dietary fiber consumption on human health: An umbrella review of evidence from 17,155,277 individuals. Clinical Nutrition, 51, 325-333. https://doi.org/10.1016/j.clnu.2025.06.021
Vinelli, V., Biscotti, P., Martini, D., Del Bo', C., Marino, M., Merano, T., Nikoloudaki, O., Calabrese, F. M., Turroni, S., Taverniti, V., Union Caballero, A., Andres-Lacueva, C., Porrini, M., Gobbetti, M., De Angelis, M., Brigidi, P., Pinart, M., Nimptsch, K., Guglielmetti, S., & Riso, P. (2022). Effects of Dietary Fibers on Short-Chain Fatty Acids and Gut Microbiota Composition in Healthy Adults: A Systematic Review. Nutrients, 14(13), 2559. https://doi.org/10.3390/nu14132559
Zhang, D., Jian, Y. P., Zhang, Y. N., et al. (2023). Short-chain fatty acids in diseases. Cell Communication and Signaling, 21, 212. https://doi.org/10.1186/s12964-023-01219-9