You Don’t Need 10,000 Steps: How Many Steps Per Day for Heart Health?
Find the optimal steps per day for heart health. Evidence shows benefits start at 4,000 steps and improve up to 10,000 with intensity.
HEARTEXERCISE
Dr. T.S. Didwal, M.D.(Internal Medicine)
4/12/202616 min read
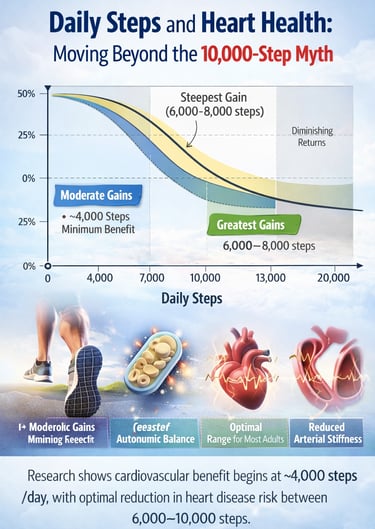
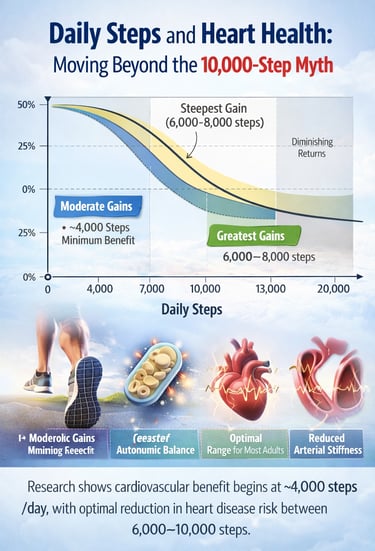
Research shows that cardiovascular benefits begin at around 4,000 steps per day, with the greatest risk reduction occurring between 6,000 and 8,000 steps. For most adults, 8,000 to 10,000 steps daily provides optimal heart health benefits, especially when combined with brisk walking intensity.
4,000 steps per day is where meaningful cardiovascular protection begins.
6,000 to 8,000 steps delivers strong, well-evidenced cardiovascular protection for most adults.
8,000 to 10,000 steps is the optimal zone for middle-aged adults.
Intensity amplifies benefit — brisk walking outperforms casual strolling at equivalent step counts.
Distributing steps throughout the day is more protective than accumulating them in a single block.
You do not need to reach 10,000 steps to protect your heart — starting from sedentary, every 1,000 additional steps you take is a meaningful investment in cardiovascular health.
Clinician Perspective: Reframing Step Count as a Cardiovascular Vital Sign
Step count should be viewed as a measurable clinical biomarker, not lifestyle advice.
In the same way we track blood pressure, HbA1c, and LDL-C, daily step count provides a quantifiable, reproducible indicator of cardiovascular risk. Wearable-derived activity data is increasingly reliable and scalable, making it suitable for routine clinical integration.The dose–response relationship is clinically actionable.
Evidence consistently shows the steepest reduction in cardiovascular and all-cause mortality occurs between ~2,000 and 8,000 steps/day. This is critical: the largest gains are seen in the most sedentary patients—those we often struggle to engage in traditional exercise prescriptions.Low baseline activity is a high-risk phenotype.
Patients consistently below ~4,000 steps/day represent a group with markedly elevated cardiometabolic risk, often paralleling profiles seen in obesity, insulin resistance, and early vascular dysfunction. Identifying and targeting this group should be a preventive priority.Step prescriptions are more adherent than exercise prescriptions.
Advising “walk 1,000 more steps per day this week” is behaviorally simpler and more sustainable than prescribing structured exercise programs, particularly in older adults or those with comorbidities.Intensity modifies benefit and should be incorporated pragmatically.
Encouraging brief bouts of brisk walking (≥100 steps/min) introduces moderate-to-vigorous stimulus without requiring formal exercise sessions, improving endothelial function and cardiorespiratory fitness.Sedentary time must be addressed independently.
A patient achieving 8,000 steps in a single bout but remaining sedentary for the rest of the day retains residual cardiovascular risk. Breaking sitting time is a distinct therapeutic target.Integration into routine care is the next frontier.
Step count can be incorporated into electronic health records, remote monitoring, and follow-up visits—transforming movement into a prescribable, trackable intervention alongside pharmacotherapy.
How Many Steps Per Day for Heart Health? What the Science Actually
For decades, one number has dominated the public imagination of physical activity: 10,000 steps per day. It appears in fitness trackers, workplace wellness programs, and even casual clinical advice. Yet this widely accepted benchmark was never born from cardiovascular science—it originated as a marketing concept in 1960s Japan, long before large-scale epidemiological data could define meaningful thresholds for health. Today, that gap between perception and evidence has finally closed. Advances in wearable technology and harmonized cohort analyses now allow us to quantify, with remarkable precision, how everyday movement translates into cardiovascular risk reduction.
What has emerged is not a single “magic number,” but a biologically coherent dose–response relationship. Across multiple large prospective datasets, including analyses published in Circulation and the Journal of the American College of Cardiology, daily step count demonstrates a steep early decline in both all-cause and cardiovascular mortality, followed by a gradual plateau at higher activity levels (Paluch et al., 2023; Stens et al., 2023). Crucially, the greatest relative gains occur among the least active individuals—those moving from profound sedentary behavior to even modest levels of daily walking. A recent dose–response meta-analysis in The Lancet Public Health further reinforces this paradigm, showing that substantial cardiovascular protection begins well below the traditional 10,000-step threshold, with the most efficient gains occurring between approximately 2,000 and 8,000 steps per day (Ding et al., 2025).
This shift reframes how clinicians should think about physical activity. Walking is no longer merely lifestyle advice—it is a quantifiable, scalable intervention with measurable effects on endothelial function, metabolic regulation, autonomic balance, and vascular aging. In an era where high-cost therapies dominate cardiovascular care, the simple act of accumulating steps may represent one of the most accessible and underutilized tools in preventive medicine (Lenharo, 2026).
The 10,000-Step Myth: Why It Persisted So Long
The appeal of 10,000 steps is understandable. It is a round number, easy to track, and just challenging enough to feel virtuous. Wearable companies built entire ecosystems around it. Healthcare providers casually repeated it. But no prospective study originally validated it as a specific cardiovascular threshold.
What changed? Large-scale harmonized data sets. Over the past five years, researchers have pooled data from hundreds of thousands of adults wearing accelerometers — not self-reporting exercise, but having it objectively measured — and tracked their cardiovascular outcomes over the years. The picture that has emerged is both more generous at the low end and more complex at the high end than 10,000 implied.
What the Evidence Actually Shows: A Dose-Response Relationship
The most important insight from modern research is that the relationship between steps and heart health is not linear — it is a curve with steep early benefits and a gentle plateau.
A 2023 meta-analysis published in the Journal of the American College of Cardiology (Stens et al., 2023) pooled data across multiple cohort studies and found that every 1,000 additional steps per day was associated with a measurable reduction in cardiovascular events and all-cause mortality. Critically, the largest gains occurred at the lower end of the step count spectrum.
A harmonized meta-analysis published in Circulation by the Steps for Health Collaborative, Paluch et al., 2023 which analyzed prospective data from multiple cohorts, found a clear inverse relationship between daily step counts and incident cardiovascular disease. The association was robust across age groups, sex, and geographic regions.
Perhaps most significantly, a systematic review and dose-response meta-analysis published in The Lancet Public Health (Ding et al., 2025) provided the most granular picture yet of how steps translate into health outcomes at a population scale. This study confirmed what earlier analyses had suggested: the cardiovascular protection from walking begins at far fewer steps than 10,000, and accumulates most rapidly between 2,000 and 8,000 steps per day.
A 2026 piece in Nature (Lenharo, 2026) captured the emerging consensus succinctly: even modest increases in daily movement — what researchers once considered too small to matter — are producing surprisingly large health benefits, particularly in previously sedentary populations. The implication is that getting off the sofa may be the single most impactful cardiovascular intervention available to the average adult.
The Step Count Thresholds Your Heart Cares About
Based on the cumulative weight of evidence, here is what we can say with reasonable confidence:
Around 4,000 steps per day appears to be the minimum meaningful threshold. Below this level, cardiovascular and mortality risks rise steeply. Above it, measurable protection begins. For adults who are currently largely sedentary, reaching 4,000 steps is a genuinely important first goal — and one that is achievable with two 20-minute walks.
6,000 to 8,000 steps per day represents a zone of strong cardiovascular protection. Studies consistently show that adults in this range enjoy substantially lower rates of coronary artery disease, stroke, and cardiovascular mortality compared to those walking fewer than 4,000 steps. Older adults (over 60) appear to derive particularly strong protection in this range, with diminishing additional returns beyond 8,000 steps.
8,000 to 10,000 steps per day is the optimal target range for most middle-aged adults. The Circulation meta-analysis found that cardiovascular risk continued to decline meaningfully up to approximately 10,000 steps in adults aged 40 to 60 years. This is where the legacy 10,000-step guideline actually has some scientific grounding — not as a universal threshold for all ages, but as a reasonable ceiling for the most cardiovascular-active portion of the dose-response curve.
Beyond 12,000 steps per day shows diminishing cardiovascular returns. This does not mean more walking harms you — it almost certainly does not — but the marginal cardiovascular benefit per additional 1,000 steps becomes small. At this level, factors like cadence, intensity, and structured exercise training may add more value than raw step count alone.
Age Changes the Equation
One of the most important refinements to emerge from recent research is that optimal step targets are age-dependent.
For middle-aged adults between 40 and 60, the dose-response curve for cardiovascular events continues to decline meaningfully up to around 10,000 steps. This is the group for whom the 10,000-step target is most evidence-supported.
For younger adults under 40, metabolic optimization — insulin sensitivity, visceral fat reduction, blood pressure control — may require higher step counts and higher-intensity movement to achieve the same protective benefit, given the physiological resilience of younger cardiovascular systems.
It Is Not Just How Many — It Is How Fast
Step cadence (steps per minute) is emerging as an important secondary variable. Not all steps are created equal cardiovascularly.
Walking at fewer than 80 steps per minute is considered light-intensity activity. Between 80 and 100 steps per minute approximates moderate intensity. Above 100 steps per minute — what is sometimes called "brisk walking" or power walking — crosses into the moderate-to-vigorous physical activity (MVPA) range that international guidelines have long recognized as most protective for the heart.
A long-term cohort study published in Circulation (Joh et al., 2022) examining leisure-time physical activity intensity and all-cause mortality in US adults found that higher-intensity activity was independently associated with lower cardiovascular and all-cause mortality. The takeaway for daily walkers: if you have limited time, walking faster matters. A 20-minute brisk walk at 110 steps per minute confers meaningfully more cardiovascular stimulus than a 20-minute casual stroll at 70 steps per minute, even if the total step count is similar.
A practical cue: if you can hold a conversation but feel slightly breathless, you are in the right zone.
Why Walking Protects the Heart: The Biology
The mechanisms behind walking's cardiovascular benefits are now reasonably well understood.
When you walk — especially at moderate-to-brisk intensity — the mechanical shear stress of increased blood flow through your arteries stimulates the endothelium (the inner lining of blood vessels) to produce nitric oxide. Nitric oxide is a potent vasodilator: it relaxes blood vessel walls, reduces blood pressure, and inhibits the platelet aggregation that leads to clot formation. Over time, regular walking training improves endothelial function, reducing the stiffness and reactivity that underlie much of cardiovascular disease.
Beyond vascular effects, regular walking improves insulin sensitivity, reduces visceral (abdominal) adiposity, lowers circulating levels of inflammatory markers including CRP and IL-6, and modestly reduces LDL cholesterol and systolic blood pressure. These are not trivial effects — each represents a meaningful reduction in a major cardiovascular risk factor.
The British Heart Foundation's guidance (BHF, 2024) emphasizes that for patients with hypertension, regular brisk walking produces blood pressure reductions comparable in magnitude to low-dose antihypertensive medication in some studies. This is not an argument against medication — it is an argument for walking alongside it.
Advanced Mechanisms: Beyond Basic Cardiovascular Benefits
Regular walking stimulates mitochondrial biogenesis via activation of PGC-1α, enhancing cellular energy efficiency and metabolic resilience. It also improves autonomic balance, increasing heart rate variability (HRV) through greater parasympathetic (vagal) tone—an established marker of cardiovascular health and reduced mortality risk. In parallel, consistent step-based activity reduces arterial stiffness, reflected in lower pulse wave velocity, thereby improving vascular elasticity and lowering long-term cardiovascular risk.
Sedentary Time Is a Separate Risk Factor
Here is something that surprises many patients: you can walk 8,000 steps per day and still meaningfully elevate your cardiovascular risk if the remaining 22+ hours are spent sitting.
The "active couch potato" phenomenon — a person who exercises consistently but is sedentary for most of the day — is an independent cardiovascular risk factor. Prolonged sitting increases circulating triglycerides, reduces insulin sensitivity, and promotes low-grade inflammation through mechanisms that walking, done only in a single daily block, does not fully counteract.
The implication for how you accumulate steps matters. Distributing movement throughout the day — what researchers call "step snacking" — breaking up sitting time every 30 to 60 minutes with a 2 to 5 minute walk appears to confer additional cardiometabolic protection beyond total daily step count alone.
Practical Applications: How to Actually Increase Your Steps
The gap between knowing you should walk more and actually walking more is where most health behavior change fails. Here are specific, evidence-aligned strategies:
Start with your baseline, not someone else's target. If you currently average 3,000 steps, a goal of 10,000 is demotivating. Research supports incremental increases of approximately 1,000 extra steps per week as a sustainable and physiologically appropriate progression.
Use post-meal walks strategically. A 10-minute walk after meals is one of the most powerful tools for glycemic control — reducing postprandial blood glucose spikes that, over time, contribute to insulin resistance and vascular damage. It also adds roughly 1,000 to 1,500 steps to your daily count with minimal time investment.
Reframe "exercise" as "movement." Many patients feel they cannot exercise because they cannot get to a gym, cannot afford equipment, or have joint limitations. Walking requires none of these things. The therapeutic dose is achievable in everyday life: parking farther away, taking stairs, walking meetings, walking while on phone calls.
Break your sitting time deliberately. Set a phone reminder for every 45 minutes during sedentary work. Stand and take a 3 to 5 minute walk. This is not about fitness — it is about interrupting the physiological cascade triggered by prolonged sitting.
Use cadence as a quality signal. When you do walk, periodically push your pace to where you feel slightly breathless. You do not need to sustain this for the entire walk — even 5 to 10 minutes of brisk walking within a longer casual walk meaningfully increases cardiovascular stimulus.
Track consistently, not obsessively. Wearable accuracy varies, and step counts are approximations. What matters is the trend over weeks, not the precision of any single day's number.
Clinical Populations: Special Considerations
For patients managing specific conditions, step-based prescriptions carry particular weight:
Patients with hypertension benefit from regular brisk walking as an adjunct to pharmacotherapy, with studies showing modest but consistent reductions in systolic blood pressure with consistent daily walking.
Patients with type 2 diabetes benefit enormously from post-meal walks, which blunt postprandial glucose excursions through mechanisms independent of total daily activity.
Patients with established coronary artery disease require individualised step progression, typically through cardiac rehabilitation frameworks. The general population thresholds discussed here do not apply directly; any new exercise program should be discussed with a cardiologist or cardiac rehabilitation team.
For patients who are largely sedentary with multiple risk factors, a brief assessment — including resting ECG and blood pressure — before beginning a significant step increase is sensible, particularly for those over 50.
Frequently Asked Questions
Q1: Is 10,000 steps per day necessary for heart health?
No. The evidence shows meaningful cardiovascular protection beginning around 4,000 steps per day, with strong protection at 6,000 to 8,000 steps. 10,000 is a reasonable goal for middle-aged adults seeking optimal cardiovascular benefit, but it is not a universal requirement and was not originally derived from medical research.
Q2: What if I can only manage 3,000 to 4,000 steps per day?
This is a genuinely important starting point. The cardiovascular benefit curve is steepest at the low end — moving from 2,000 to 4,000 steps produces a larger proportional reduction in cardiovascular risk than moving from 8,000 to 10,000. Start where you are and build gradually.
Q3: Does walking intensity matter, or just the number of steps?
Both matter, but intensity adds meaningful cardiovascular stimulus. Walking at 100 or more steps per minute (brisk enough to feel slightly breathless) activates endothelial, metabolic, and cardiovascular benefits that leisurely strolling does not fully replicate.
Q4: Can I replace structured exercise with daily steps?
For most adults who cannot or do not engage in structured exercise, high daily step counts provide substantial cardiovascular protection. However, combining consistent daily walking with even 1 to 2 sessions per week of more structured activity (resistance training, swimming, cycling) provides additive benefits that steps alone cannot replicate — particularly for muscular strength and bone density.
Q5: How do I track my steps accurately?
Modern smartphones and wrist-worn accelerometers are reasonably accurate for walking, though they may over- or under-count in specific circumstances. Consistency matters more than precision — using the same device daily gives you a reliable relative measure of your activity trends.
Q6: Does step count matter if I sit most of the day?
Yes, but sitting time is an independent risk factor. Achieving a daily step goal in a single block while sitting for the rest of the day reduces — but does not eliminate — the cardiovascular risk from prolonged sedentary behavior. Distributing steps throughout the day is more protective.
Q7: At what point should I consult a doctor before increasing steps?
If you have known cardiovascular disease, have been sedentary for several years with multiple risk factors (hypertension, diabetes, smoking history, high cholesterol), are over 50 and starting a new activity program, or experience chest pain, unusual breathlessness, or palpitations during activity — speak with your GP or cardiologist before significantly increasing your step target.
Clinical Pearls
1. The "Glycemic Blunt" (Post-Prandial Walking)
Scientific Perspective: A 10–15 minute walk immediately following a meal facilitates "glucose disposal" via GLUT4 translocation in skeletal muscle, independent of insulin. This significantly blunts the post-prandial glucose spike, reducing systemic glycation and vascular inflammation.
Think of your muscles as a sponge. After you eat, your blood is full of sugar. Walking "squeezes the sponge," allowing your muscles to soak up that sugar for fuel before it has a chance to sit in your bloodstream and damage your "pipes."
2. The "Shear Stress" Benefit (Endothelial Health)
Scientific Perspective: Walking increases laminar shear stress on the vascular endothelium. This mechanical stimulus upregulates Endothelial Nitric Oxide Synthase (eNOS), increasing nitric oxide bioavailability, which lowers Pulse Wave Velocity (PWV) and improves arterial compliance.
Your arteries aren't just static tubes; they are living tissue that needs "exercise" just like your biceps. Brisk walking creates a gentle friction against the inner walls of your blood vessels, which signals them to release a natural "relaxant" that keeps your arteries flexible instead of stiff.
3. The "Vagal Brake" (Autonomic Balance)
Scientific Perspective: Consistent, low-to-moderate intensity walking enhances parasympathetic (vagal) tone. This improves Heart Rate Variability (HRV) by optimizing the "vagal brake" on the sinoatrial node, providing a systemic buffer against catecholamine-driven stress responses.
Walking is like a "reset button" for your nervous system. It strengthens your body’s ability to move from "fight-or-flight" mode into "rest-and-repair" mode. A higher HRV means your heart is more adaptable and resilient to the stresses of daily life.
4. The "Mitochondrial Signal" ($PGC-1\alpha$)
Scientific Perspective: Walking—particularly when varying intensity—activates the AMPK pathway, which triggers $PGC-1\alpha$. This is the master switch for mitochondrial biogenesis, ensuring that the cellular "engines" remain numerous and efficient, thereby delaying metabolic aging and sarcopenia.
Every step is a message to your cells to "upgrade the hardware." Walking tells your body to build brand-new, high-efficiency power plants (mitochondria) inside your muscles. This gives you more natural energy and helps keep your muscles from "rusting" as you age.
5. The "Step Snacking" Strategy (Sedentary Interruption)
Scientific Perspective: Breaking up sedentary time with "activity snacks" (3 minutes of walking every 45 minutes) prevents the suppression of Skeletal Muscle Lipoprotein Lipase (LPL) activity. This is critical for maintaining healthy triglyceride levels and insulin sensitivity, even if the total daily step count is otherwise met.
Doing one long walk but sitting the rest of the day is like brushing your teeth once a week for two hours—it doesn't work that way. You need "movement snacks" throughout the day to keep your fat-burning enzymes "turned on." A 3-minute stroll every hour is just as important as your morning exercise.
Author’s Note
This article was written to bridge a persistent gap between public health messaging and modern cardiovascular science. For decades, physical activity advice has been reduced to simplified targets that, while easy to communicate, often fail to reflect the true biology of risk reduction. The goal here is not to replace one arbitrary number with another, but to reframe walking as a measurable, evidence-based intervention grounded in dose–response physiology.
The insights presented are drawn from large-scale prospective cohort studies, harmonized meta-analyses, and leading cardiovascular journals, with an emphasis on translating population-level data into clinically meaningful guidance. Particular care has been taken to ensure that the recommendations are not only scientifically accurate but also practical for real-world patients—especially those who are sedentary, time-constrained, or managing chronic conditions.
As a clinician, I see daily how overwhelming “perfect” health targets can become barriers to meaningful change. The evidence is clear: cardiovascular benefit begins well below traditional thresholds, and incremental improvements in daily movement can produce substantial reductions in risk. This is a message worth emphasizing—not just for individual patients, but for how we design preventive strategies at a population level.
Readers are encouraged to interpret step targets as flexible ranges rather than rigid goals, and to consider consistency, progression, and safety as central principles. For individuals with known cardiovascular disease or significant risk factors, step-based activity should be integrated thoughtfully within a broader, personalized care plan.
Ultimately, the science of movement is evolving. As wearable technology, digital health, and preventive cardiology continue to converge, step count may become one of the most accessible and actionable vital signs in modern medicine.
Talk to your healthcare provider about incorporating a step target into your cardiovascular risk management plan — it is a conversation increasingly supported by the highest-quality evidence in preventive cardiology.
Your heart responds to every step. Take more of them.
Medical Disclaimer: This article is intended for educational and informational purposes only. It does not constitute medical advice and should not be used as a substitute for consultation with a qualified healthcare professional. Always discuss exercise programmes and cardiac risk assessment with your doctor, particularly if you have existing cardiovascular disease or significant risk factors.
Related Articles
HIIT for Athletes: Boost VO₂ Max, Lactate Threshold, and Peak Performance – Science-Based Guide
Want to Live Longer? The #1 Science-Backed Habit Is Simpler Than You Think — Just Walk
Is Your Heart at Risk? How the TG/HDL Ratio Can Warn You Early | DR T S DIDWAL
How Exercise Boosts Nitric Oxide and Blood Flow: The Endothelial Shear Stress Mechanism
Exercise and Vascular Health: How Nitric Oxide and Endothelial Function Keep Your Arteries Young
How Exercise Boosts Nitric Oxide and Blood Flow: The Endothelial Shear Stress Mechanism
References
Paluch, A. E., Bajpai, S., Ballin, M., Bassett, D. R., Buford, T. W., Carnethon, M. R., Chernofsky, A., Dooley, E. E., Ekelund, U., Evenson, K. R., Galuska, D. A., Jefferis, B. J., Kong, L., Kraus, W. E., Larson, M. G., Lee, I.-M., Matthews, C. E., Newton, R. L., Nordström, A., Nordström, P., Palta, P., Patel, A. V., Pettee Gabriel, K., Pieper, C. F., Pompeii, L., Rees-Punia, E., Spartano, N. L., Vasan, R. S., Whincup, P. H., Yang, S., & Fulton, J. E. (2023). Prospective association of daily steps with cardiovascular disease: A harmonized meta-analysis. Circulation, 147(2), 122–131. https://doi.org/10.1161/CIRCULATIONAHA.122.061288
British Heart Foundation. (2024, May 7). How many steps a day should I walk for my heart health? https://www.bhf.org.uk/informationsupport/heart-matters-magazine/activity/how-many-steps-a-day-should-i-walk-for-my-heart-health
Ding, D., Nguyen, B., Nau, T., et al. (2025). Daily steps and health outcomes in adults: A systematic review and dose-response meta-analysis. The Lancet Public Health. https://doi.org/10.1016/S2468-2667(25)00164-1
Joh, H.-K., Keum, N., Ferrari, G., Rey-Lopez, J. P., Rimm, E. B., Tabung, F. K., & Giovannucci, E. L. (2022). Long-term leisure-time physical activity intensity and all-cause and cause-specific mortality: A prospective cohort of US adults. Circulation, 146(7), 523–534. https://doi.org/10.1161/CIRCULATIONAHA.121.058162
Lenharo, M. (2026). The surprisingly big health benefits of just a little exercise. Nature, 649(8099), 1092–1094. https://doi.org/10.1038/d41586-026-00237-0
Stens, N. A., Bakker, E. A., Mañas, A., Buffart, L. M., Ortega, F. B., Lee, D.-c., Thompson, P. D., Thijssen, D. H. J., & Eijsvogels, T. M. H. (2023). Relationship of daily step counts to all-cause mortality and cardiovascular events: A meta-analysis. Journal of the American College of Cardiology, 82(15), 1483–1494. https://doi.org/10.1016/j.jacc.2023.07.029