Want to Live Longer? The #1 Science-Backed Habit Is Simpler Than You Think—Just Walk
Discover how daily walking boosts heart health, lowers diabetes and cardiovascular risk, and extends lifespan. Learn the science of steps, optimal pace, and how just 5 minutes a day can reduce premature death.
EXERCISEAGING
Dr. T.S. Didwal, M.D.(Internal Medicine)
4/18/202618 min read
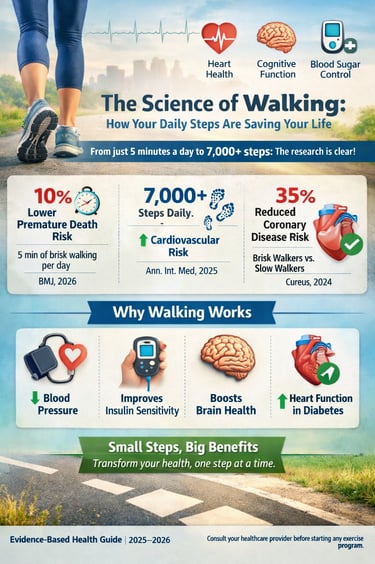

What are the health benefits of walking daily?
Walking daily is a scientifically proven way to improve cardiovascular health, reduce the risk of chronic diseases, and increase lifespan. Research shows that 7,000–9,000 steps per day significantly lowers cardiovascular risk, while even 5 minutes of brisk walking daily can reduce premature death (del Pozo Cruz et al., 2025; Feinmann, 2026). Walking enhances heart function, improves insulin sensitivity, lowers blood pressure, and reduces inflammation. Importantly, walking pace matters—brisk walking is associated with a ~35% lower risk of coronary artery disease compared to slow walking (Nurrobi et al., 2024).
Overall, walking is a low-cost, accessible, and evidence-based intervention that delivers substantial health benefits across all age groups, making it one of the most effective forms of daily physical activity for long-term health and disease prevention.
🩺 Clinician’s Perspective: Translating Walking Science into Practice
Prescribe walking as medicine, not advice
Walking should be framed as a first-line therapeutic intervention, particularly for patients with cardiometabolic disease. Evidence supports its role in reducing cardiovascular events, improving glycemic control, and lowering all-cause mortality (del Pozo Cruz et al., 2025).Target the “sedentary-to-active” transition
The greatest clinical benefit occurs when patients move from <4,000 to ~7,000–9,000 steps/day, making this the most impactful and realistic initial goal rather than arbitrary high targets.Incorporate walking into chronic disease management
In patients with type 2 diabetes, structured walking programs have demonstrated improvements in left ventricular function and diastolic parameters, suggesting reversal of early diabetic cardiomyopathy (Leischik et al., 2026).Emphasize intensity alongside volume
Encourage brisk walking (moderate intensity) using the “talk test.” Faster walking pace independently reduces coronary artery disease risk, even when total step count is similar (Nurrobi et al., 2024).Use “minimum effective dose” for low-adherence patients
For sedentary or time-constrained individuals, recommend ≥5 minutes/day of brisk walking as an entry point. Even this small dose is associated with meaningful mortality reduction (Feinmann, 2026).Break up prolonged sitting
Advise patients to interrupt sedentary time every 30–60 minutes with short walking bouts. This improves postprandial glucose, vascular function, and overall metabolic health.Leverage behavioral tools for adherence
Step counters, smartphone apps, and simple logs improve compliance. Setting incremental goals (+1,000–2,000 steps/day) is more sustainable than drastic changes.Individualize prescriptions
Adjust walking plans based on:Age and baseline fitness
Comorbidities (e.g., osteoarthritis, heart failure)
Medication use (e.g., insulin, beta-blockers)
Reinforce long-term healthspan benefits
Regular walking is associated not only with longevity but also with reduced frailty, better cognitive outcomes, and preserved functional independence.Integrate into routine consultations
Document physical activity as a vital sign, and revisit walking goals at each follow-up to reinforce its role as ongoing therapy.
Why Walking Is More Powerful Than Most People Realise
Walking is often dismissed as a low-impact, low-value activity—but contemporary exercise science tells a very different story. Accumulating evidence from large-scale cohort studies, randomized trials, and meta-analyses now positions walking as a dose-responsive, physiologically potent intervention capable of modifying cardiovascular risk, metabolic health, and mortality outcomes across diverse populations (del Pozo Cruz et al., 2025; Nurrobi et al., 2024). At its core, walking is a form of moderate-intensity aerobic activity that engages multiple organ systems simultaneously—enhancing endothelial function, improving insulin sensitivity, and stimulating favorable autonomic adaptations that collectively reduce disease burden.
Recent data suggest that the relationship between walking and health is not linear but threshold-dependent, with the most significant gains occurring when individuals transition from sedentary behavior (<4,000 steps/day) to modest activity levels (~7,000–9,000 steps/day) (del Pozo Cruz et al., 2025). Importantly, even brief bouts of higher-intensity walking appear to confer measurable survival benefits; a contemporary population analysis reported that as little as five minutes of brisk daily activity may reduce premature mortality risk by approximately 10% (Feinmann, 2026). These findings challenge the traditional notion that meaningful health improvements require prolonged or high-intensity exercise.
Beyond epidemiological associations, mechanistic studies provide biological plausibility. Walking has been shown to improve cardiac function—including left ventricular ejection fraction—in high-risk populations such as individuals with type 2 diabetes, suggesting a direct role in reversing subclinical cardiovascular dysfunction (Leischik et al., 2026). Furthermore, walking pace independently predicts coronary artery disease outcomes, underscoring that intensity—not just volume—matters (Nurrobi et al., 2024).
Taken together, the emerging literature reframes walking from a simple daily habit into a clinically relevant, scalable intervention with profound implications for both individual health and public health policy.
10% reduction in premature deaths from just 5 min/day of vigorous walking, Feinmann, 2026 (BMJ)
7,000+ steps/day linked to significantly lower cardiovascular event risk del Pozo Cruz et al., 2025
35% reduced coronary artery disease risk for brisk walkers vs. slow walkers Nurrobi et al., 2024
↑ EF improved left ventricular ejection fraction in type 2 diabetes patients after walking, Leischik et al., 2026
Key insight: Walking is classified as "moderate-intensity physical activity" by the World Health Organisation and is uniquely accessible because it carries minimal injury risk, requires no equipment, and can be performed across virtually all demographics — from university students to elderly patients with chronic disease.
Walking and Your Heart: Landmark 2026 Findings
Perhaps the most striking recent study comes from Germany and Spain. Leischik et al. (2026) published a clinical trial in the Journal of Cardiovascular Development and Disease specifically examining what walking does to left ventricular (LV) function — the mechanical pumping capacity of the heart's most important chamber — in patients with Type 2 diabetes (T2D).
This matters because Type 2 diabetes is notorious for damaging the heart in subtle ways. Diabetic cardiomyopathy — a form of heart muscle disease driven by chronically elevated blood sugar — impairs the heart's ability to contract and relax efficiently, even before any symptoms appear. For millions of people living with T2D, this silent deterioration increases the long-term risk of heart failure, stroke, and sudden cardiac death.
What Leischik and colleagues found was both clinically significant and deeply encouraging: a structured walking programme meaningfully improved left ventricular ejection fraction (LVEF) — the percentage of blood the heart pumps out with each beat — in their T2D patient group. Improvements were also noted in diastolic function (how well the heart relaxes between beats) and indices of cardiac strain. The authors concluded that walking is a safe, cost-effective, and reproducible intervention for improving cardiac function in this high-risk population (Leischik et al., 2026).
What this means for you: If you have Type 2 diabetes — or a family history of it — a consistent daily walk is not merely a lifestyle choice. According to clinical evidence, it actively protects and rehabilitates your heart muscle. This is especially important because it can reverse damage that may have been accumulating silently for years.
The Cardiovascular Cascade: How Walking Helps the Heart
Improves arterial elasticity
Regular walking enhances vascular compliance, leading to lower resting blood pressure and reduced afterload.Strengthens cardiac muscle
Sustained ambulatory activity improves myocardial efficiency, resulting in a lower resting heart rate and improved stroke volume.Optimizes lipid profile
Walking increases HDL (good cholesterol) while reducing LDL and triglycerides, contributing to reduced atherosclerotic risk.Reduces systemic inflammation
Chronic low-grade inflammation—a key driver of atherosclerosis—is attenuated through regular physical activity.Enhances insulin sensitivity
Improved glucose uptake reduces hyperinsulinemia and metabolic stress, lowering cardiovascular burden in patients with insulin resistance or type 2 diabetes.Decreases overall cardiovascular load
Through combined metabolic and hemodynamic effects, walking reduces strain on the heart and improves long-term cardiovascular outcomes
How Many Steps Do You Actually Need?
The famous "10,000 steps per day" target has been so widely repeated that most people assume it has deep scientific roots. In fact, it originated as a marketing slogan for a 1960s Japanese pedometer. So what does modern science actually say about the optimal step count?
A major 2025 paper in the Annals of Internal Medicine by del Pozo Cruz and colleagues tackled this exact question. Their study, focused on "suboptimally active adults" — people who exercise some but not consistently enough to meet recommended guidelines — examined how different step accumulation patterns relate to cardiovascular event risk and all-cause mortality.
The findings were nuanced and important. The research found that adults who increased their daily steps from low baselines to modest targets saw meaningful, dose-dependent reductions in cardiovascular risk. Importantly, the protective benefits were visible well below the 10,000-step threshold: individuals reaching 7,000–9,000 steps per day showed substantially lower risk of cardiovascular events compared to those taking fewer than 5,000 steps. Beyond approximately 10,000 steps, the marginal gains diminished — good news for anyone who has felt defeated by the idea of hitting that arbitrary target (del Pozo Cruz et al., 2025). The study shows that among people with <8,000 steps/day, accumulating steps in longer continuous bouts (especially ≥10–15 minutes) is linked to meaningfully lower all-cause mortality and CVD incidence compared to many short scattered bouts.
The "step floor" principle: The biggest health gains from increasing your step count occur in the transition from very sedentary (under 4,000 steps/day) to moderately active (7,000–9,000 steps/day). You do not need to run a half-marathon in footsteps every day to reap cardiovascular rewards — but you do need to move consistently and meaningfully beyond baseline sedentary behaviour.
Five Minutes a Day: The Breakthrough Discovery
For anyone who feels overwhelmed by exercise recommendations, the findings summarised by Feinmann (2026) in the BMJ offer a message of remarkable accessibility. Reporting on a large-scale population study, the BMJ piece highlighted that adding just five minutes of higher-intensity physical activity — such as brisk walking up an incline or walking briskly while carrying grocery bags — to an otherwise sedentary day could cut the risk of premature death by approximately 10%.
Ten percent may not sound dramatic in isolation, but considered at a population level, this is an extraordinary finding. For every ten people in a sedentary population who adopted this single small habit, one premature death could be prevented. Applied across millions of people, the public health implications are staggering.
The "tiny habit" principle: You do not need to overhaul your life to begin capturing meaningful health benefits from walking. A 5-minute brisk walk — perhaps from the car park to the office, or around the block after dinner — represents a physiologically meaningful intervention according to emerging evidence. Start small. The science supports it.
This finding is particularly relevant for the many people who cite "lack of time" as their primary barrier to exercise. Five concentrated minutes of effort, inserted into a single part of the day, is achievable by almost anyone. The key word here is intensity: brisk or purposeful walking — not a casual stroll — is what drives the benefit.
Walking for a Longer Life: What the Systematic Reviews Show
A 2025 systematic review published in the International Journal of Research Publication and Reviews examined the accumulated body of evidence on walking habits and longevity. The review synthesised findings across multiple decades and populations, and its conclusions aligned powerfully with the individual clinical studies cited above.
Consistent walking habits were associated with reductions in all-cause mortality — that is, death from any cause — across virtually all age groups examined. The protective effects were particularly pronounced for cardiovascular mortality, which remains the leading cause of death globally. Regular walkers also showed lower incidence of certain cancers, reduced rates of cognitive decline, and better mental health outcomes compared to sedentary counterparts (International Journal of Research Publication and Reviews, 2025).
What makes these findings especially noteworthy is their consistency across diverse populations: men and women, different ethnicities, varying socioeconomic groups, and across cultures with dramatically different baseline activity norms. This breadth of evidence suggests that the benefits of walking are biological and universal — not contingent on any particular cultural or lifestyle context.
Longevity dividend: The systematic review evidence suggests that regular walkers can expect not just to live longer on average, but to live better — with more years of functional independence, lower rates of chronic disease burden, and better preservation of mobility and cognitive function into older age
.
Does Pace Matter? Walking Speed and Coronary Artery Disease
Yes, pace matters — perhaps more than most people realise. A 2024 systematic review and meta-analysis by Nurrobi and colleagues, published in Cureus, specifically investigated the relationship between walking pace and the risk of coronary artery disease (CAD) events — including angina, heart attacks, and cardiac deaths.
The meta-analysis pooled data from multiple prospective studies and found a significant inverse relationship between walking pace and CAD risk: people who walked at a brisk pace had substantially lower rates of coronary artery disease events compared to slow walkers, even after controlling for total walking volume. In other words, how fast you walk independently predicts heart health outcomes, over and above how far or how often you walk (Nurrobi et al., 2024).
Brisk walking elevates the heart rate into the moderate-intensity zone — approximately 50–70% of maximum heart rate for most adults — which delivers physiological adaptations similar to other aerobic activities: improved cardiac output, enhanced stroke volume, better vascular endothelial function, and more efficient oxygen extraction by muscles. Slow, leisurely walking, while better than pure sedentariness, does not reliably produce these adaptations.
How to Define "Brisk" Walking
A practical rule of thumb is the "talk test": you should be able to hold a conversation while walking briskly, but would find it difficult to sing. In terms of measurable pace, most health guidelines define brisk walking as approximately 4.5–5.5 km/h (roughly 100 steps per minute). On a standard smartwatch or step counter, this translates to a cadence you can consciously aim for and monitor.
Walking Interventions in Young Adults: Why It Matters for Everyone
It would be a mistake to assume that walking's health benefits are relevant only to middle-aged or older adults managing chronic disease. A 2025 randomised controlled trial protocol by Godoy-Cumillaf et al., published in JMIR Research Protocols, highlights a troubling and under-discussed public health reality: university students — typically aged 18–25 — are increasingly sedentary, and this sedentariness is already producing measurable deteriorations in health indicators including cardiovascular fitness, body composition, mental health markers, and metabolic parameters.
The trial protocol describes a walking-based physical activity intervention designed specifically for university students. Its primary goal is to examine whether structured walking programmes can reverse or prevent these health declines in young adults who are otherwise unlikely to engage in formal exercise (Godoy-Cumillaf et al., 2025).
The significance of this research extends well beyond the campus. Young adulthood is a critical window for establishing lifelong health behaviours. Sedentary habits formed at university tend to persist into adult working life, amplifying long-term cardiovascular risk. Conversely, embedding a walking habit during the early twenties creates a foundation that research consistently shows is carried forward — with compounding health benefits over decades.
For younger readers: You don't have to wait until your forties to start "taking health seriously." The evidence is clear that sedentary habits form early — and so do the chronic disease pathways they trigger. A walking habit started at 20 pays dividends at 60 in ways no medication can fully replicate.
Limitations & What We Still Don’t Know
Observational bias: Many step-count studies are observational, so healthier individuals may naturally walk more (reverse causation).
Measurement variability: Step counts and intensity can vary across devices and may not perfectly reflect true physical activity.
Individual variability: Responses to walking differ based on age, genetics, baseline fitness, and comorbidities.
Dose vs intensity uncertainty: The optimal balance between step volume and walking intensity is still being refined.
Bottom line: While the evidence is strong and consistent, walking should be viewed as a powerful but individualized intervention, not a one-size-fits-all prescription.
Practical Applications: How to Build a Walking Habit That Lasts
Understanding the science is only half the equation. Here is a structured, evidence-informed framework for building a consistent walking habit that delivers real health results — regardless of where you are starting from.
Start with your baseline — not someone else's target. Use a phone or basic pedometer to track your current daily steps for one week without changing behaviour. This gives you your personal baseline. Your first target should be adding 1,000–2,000 steps above that baseline, not jumping immediately to 10,000. Sustainable progress, not dramatic leaps, is what the research supports.
Prioritise pace over distance — at least for cardiovascular goals. Based on the Nurrobi et al. (2024) meta-analysis, walking pace independently predicts heart health outcomes. Aim for a brisk pace — use the "talk test" as your guide. Even 20 minutes of brisk walking produces measurable improvements in cardiovascular markers over time.
Distribute steps throughout the day, not just in one block. Del Pozo Cruz et al. (2025) found that step distribution patterns matter. Set an hourly movement reminder on your phone or smartwatch. A 5-minute walk every hour of a seated workday adds up to 40+ minutes of movement without requiring any dedicated "exercise time."
Use the "5-minute rule" on low-motivation days. Feinmann (2026) reports that even 5 minutes of brisk activity produces meaningful mortality benefits. On days when motivation is low, commit to only 5 minutes. More often than not, you'll continue — but even if you don't, you've still done something clinically meaningful.
Make it social or purposeful. Walking with a friend, colleague, or pet dramatically increases adherence. Alternatively, attaching your walk to a purpose — walking to the coffee shop, the post office, or a colleague's desk instead of emailing — removes the psychological friction of "going for a walk" as a separate chore.
If you have Type 2 diabetes, tell your doctor about your walking plan. The Leischik et al. (2026) trial specifically demonstrates that walking improves cardiac function in T2D patients. Your healthcare provider should know about your exercise plans because walking can affect blood glucose levels and may require adjustments to medication timing or dosage.
Track progress with simple self-monitoring tools. You don't need an expensive smartwatch. A free step-counting app on a standard smartphone, or even a basic pedometer clip (often under £10), provides enough data to monitor progress and maintain motivation. Research consistently shows that self-monitoring is one of the most powerful behavioural tools for sustaining physical activity habits.
Your Personal Walking Action Plan — Check Off As You Go
Track my steps for 7 days to establish my baseline
Set a first target: baseline + 1,500 steps/day
Enable hourly movement reminders on phone/watch
Identify 2 daily "walk substitutes" (e.g., taking stairs, walking to lunch)
Schedule one 20-min brisk walk into my weekly calendar
Tell one friend or family member about my walking goal (accountability!)
If I have diabetes or a heart condition, discuss walking with my doctor
Frequently Asked Questions: Clinical & Pathophysiological Perspectives
1. What is the evidence-based minimum effective dose for daily step accumulation?
Current longitudinal data, specifically from del Pozo Cruz et al. (2025), indicate a non-linear dose-response relationship. While the historical "10,000 steps" benchmark serves as a useful heuristic, the most significant reduction in cardiovascular (CV) event risk occurs when transitioning from a sedentary state (<4,000 steps/day) to a moderate threshold of 7,000–9,000 steps/day. Beyond this range, the marginal utility for all-cause mortality reduction diminishes, suggesting a "sweet spot" for primary prevention.
2. Through what mechanisms does walking improve cardiac function in metabolic patients?
In patients with Type 2 Diabetes (T2D), walking interventions address diabetic cardiomyopathy by improving left ventricular (LV) strain and systolic function. Research by Leischik et al. (2026) demonstrates that consistent ambulatory activity increases Left Ventricular Ejection Fraction (LVEF) and enhances diastolic filling pressures. This is likely driven by improved myocardial insulin sensitivity and reduced systemic inflammation, which mitigates the fibrotic remodeling of the heart muscle.
3. How does walking velocity independently influence Coronary Artery Disease (CAD) risk?
Meta-analytical evidence (Nurrobi et al., 2024) confirms that walking pace is an independent predictor of CAD outcomes, distinct from total volume. Brisk walking (defined as 4.5 km/h) induces higher shear stress on the vascular endothelium, which promotes the release of nitric oxide. This process enhances vasodilation and arterial elasticity, providing a more robust cardioprotective effect than slow-cadence walking, which may not reach the metabolic threshold required for these vascular adaptations.
4. What is the clinical significance of "micro-dosing" vigorous activity?
The concept of High-Intensity Incidental Physical Activity (HIIPA) suggests that even ultra-short bouts of exertion are physiologically meaningful. According to findings published in the BMJ (2026), integrating just five minutes of vigorous walking (e.g., incline walking or rapid-pace ambulation) into a sedentary routine can result in a 10% reduction in premature mortality. These brief intervals are sufficient to trigger acute improvements in cardiorespiratory fitness (VO2 max) and glycemic control.
5. Are partitioned walking bouts as effective as continuous exercise sessions?
Evidence regarding step distribution patterns suggests that "movement snacking"—breaking activity into multiple bouts throughout the day—may offer superior metabolic benefits compared to a single continuous session. Frequent walking breaks mitigate the "sedentary paradox" by preventing prolonged periods of muscle inactivity, thereby maintaining higher levels of lipoprotein lipase activity and more stable postprandial glucose levels.
6. Can ambulatory interventions extend longevity in populations with pre-existing chronic conditions?
Yes. Systematic reviews (2025) indicate that walking reduces all-cause mortality even in "high-risk" cohorts. By improving the Body Mass Index (BMI), lipid profiles, and autonomic balance (increasing heart rate variability), walking serves as a secondary prevention strategy that slows the progression of established atherosclerotic and metabolic diseases, thereby extending the functional "healthspan" of the patient.
7. What is the primary takeaway from the 2025–2026 research synthesis?
The recent literature shifts the focus from volume-centric goals to intensity and consistency. The synthesis of recent trials highlights that walking is a potent, dose-dependent clinical intervention capable of reversing subclinical organ damage (such as LV dysfunction) and that even minimal increases in pace or duration (the "5-minute rule") yield statistically significant survival benefits across all age demographics
Clinical pearls
1. The LVEF Recovery Pearl
Scientific Perspective: Chronic hyperglycemia in Type 2 Diabetes (T2D) induces subclinical myocardial remodeling. Structured walking interventions significantly improve Left Ventricular Ejection Fraction (LVEF) and diastolic function, effectively serving as a non-pharmacological rehabilitative tool for diabetic cardiomyopathy.
Patient-Friendly Perspective: Diabetes can silently "stiffen" the heart muscle over time, making it less efficient at pumping blood. Walking acts like a tune-up for your heart's engine, helping it pump more blood with every beat and reversing some of the damage caused by high blood sugar.
2. The "Step Floor" Threshold
Scientific Perspective: The relationship between step volume and cardiovascular mortality is non-linear. The most significant reduction in Hazard Ratio (HR) occurs in the transition from a sedentary baseline (<4,000 steps) to a moderate threshold (7,000–9,000 steps), after which marginal gains begin to plateau.
Patient-Friendly Perspective: You don't need to hit the "magic" 10,000-step mark to save your life. The biggest health "bonus" happens when you move from doing almost nothing to doing a moderate amount (about 7,000 steps). After 10,000 steps, the extra health benefits are smaller, so don't stress if you can't reach elite numbers.
3. The Power of "Micro-Vigorous" Activity
Scientific Perspective: Short bursts of High-Intensity Incidental Physical Activity (HIIPA)—specifically as little as five minutes of vigorous walking—can trigger physiological adaptations that reduce premature mortality risk by up to 10%.
Patient-Friendly Perspective: Intensity beats duration when you're short on time. If you can only walk for five minutes, make them count by walking fast enough that you're huffing and puffing (like you're late for a bus). Those five "power minutes" are enough to significantly lower your risk of an early death.
4. The CAD Velocity Link
Scientific Perspective: Walking pace is an independent predictor of Coronary Artery Disease (CAD) risk. Brisk walking (4.5–5.5 km/h) improves vascular endothelial function and stroke volume more effectively than a slow, leisurely gait, regardless of the total distance covered.
Patient-Friendly Perspective: How you walk matters more than how far you walk. A short, brisk walk where you can talk but not sing is much better for your arteries than a long stroll. To protect your heart from blockages, try to pick up the pace and treat your walk like a purposeful workout.
5. The Early Intervention Mandate
Scientific Perspective: Sedentary behavior in young adults (ages 18–25) acts as a primary driver for early-onset metabolic dysfunction. Implementing walking protocols during this window mitigates the "cumulative physiological debt" that leads to chronic disease in later decades.
Patient-Friendly Perspective: Walking isn't just for seniors or people with heart problems; it's a "savings account" for young people. Habits built in your twenties prevent your body from "collecting debt" in the form of high blood pressure or weight gain that becomes much harder to fix when you're 50.
Author’s Note
This article was developed with a clear objective: to bridge the gap between rapidly evolving exercise science and practical, real-world health application. In clinical practice, one of the most consistent challenges is not a lack of effective interventions, but a lack of accessible, sustainable, and scalable strategies that patients can realistically adopt. Walking stands out as a rare exception.
The evidence presented here is drawn from recent peer-reviewed research (2024–2026), including cohort studies, randomized trials, and systematic reviews. Every effort has been made to interpret these findings accurately and translate them into clinically meaningful insights without oversimplifying the underlying physiology. However, it is important to recognize that exercise science—like all fields of medicine—is continually evolving. New data may refine, expand, or even challenge current understanding.
While walking is remarkably safe and broadly applicable, it is not a one-size-fits-all prescription. Individual responses vary based on age, baseline fitness, comorbidities, and genetic factors. Readers with existing medical conditions—particularly cardiovascular disease, diabetes, or musculoskeletal limitations—should view this guide as a complement to, not a replacement for, personalized medical advice.
From a broader perspective, the goal of this work is not merely to highlight the benefits of walking, but to reframe how we think about health interventions. In an era often dominated by complex treatments and high-cost solutions, the most powerful tools are sometimes the simplest—provided they are applied consistently and informed by evidence.
If this article achieves anything, it should be this: to encourage a shift from all-or-nothing thinking toward incremental, evidence-based action. Because in the context of long-term health, small steps—quite literally—can produce profound outcomes.
Ready to Take Your First Step?
The research is clear — every step counts. You don't need perfection, you need consistency.
Download this article, share it with someone you care about, or simply lace up your shoes and begin today.
Always consult your healthcare provider before beginning a new exercise programme if you have existing health conditions.
Medical Disclaimer: This article is intended for educational and informational purposes only. It does not constitute medical advice and should not be used as a substitute for consultation with a qualified healthcare professional. Always discuss exercise programmes and cardiac risk assessment with your doctor, particularly if you have existing cardiovascular disease or significant risk factors.
Related Articles
You Don’t Need 10,000 Steps: How Many Steps Per Day for Heart Health?
HIIT for Athletes: Boost VO₂ Max, Lactate Threshold, and Peak Performance – Science-Based Guide
Is Your Heart at Risk? How the TG/HDL Ratio Can Warn You Early | DR T S DIDWAL
How Exercise Boosts Nitric Oxide and Blood Flow: The Endothelial Shear Stress Mechanism
Exercise and Vascular Health: How Nitric Oxide and Endothelial Function Keep Your Arteries Young
References
del Pozo Cruz, B., et al. (2025). Step accumulation patterns and risk for cardiovascular events and mortality among suboptimally active adults. Annals of Internal Medicine. https://doi.org/10.7326/annals-25-01547
Feinmann, J. (2026). 5 minutes of daily exercise could cut premature deaths by 10%, study says. BMJ, 392, Article s110. https://doi.org/10.1136/bmj.s110
Godoy-Cumillaf, A., Fuentes-Merino, P., Giakoni-Ramírez, F., Muñoz-Strale, C., & Merellano-Navarro, E. (2025). Effects of a walking-based physical activity intervention on health indicators in university students: Protocol for a randomized controlled trial. JMIR Research Protocols, 14, Article e83983. https://doi.org/10.2196/83983
International Journal of Research Publication and Reviews. (2025). The impact of walking habits on longevity: A systematic review. International Journal of Research Publication and Reviews, 5(8), Article IJRPR32592. https://ijrpr.com/uploads/V5ISSUE8/IJRPR32592.pdf
Leischik, R., Bank, P., Gerlach, C. E., & Sanchis-Gomar, F. (2026). Walking improves cardiac function: A trial on the effects of walking on left ventricular function in Type 2 diabetes patients. Journal of Cardiovascular Development and Disease, 13(3), 136. https://doi.org/10.3390/jcdd13030136
Nurrobi, Y. A. S., Winston, K., Rahman, A. L., Falakhi, M. F., Aristya, M. P., Toaha, A. F., Larasaty, I. N., & Dewangga, R. (2024). Footsteps to wellness: A systematic review and meta-analysis of walking pace and coronary artery disease event. Cureus, 16(3), e56926. https://doi.org/10.7759/cureus.56926