How Exercise Boosts Nitric Oxide and Blood Flow: The Endothelial Shear Stress
Exercise boosts nitric oxide and blood flow through endothelial shear stress, improving vascular health and reducing heart disease risk.
EXERCISEHEART
Dr. T.S. Didwal, M.D.(Internal Medicine)
4/10/202613 min read
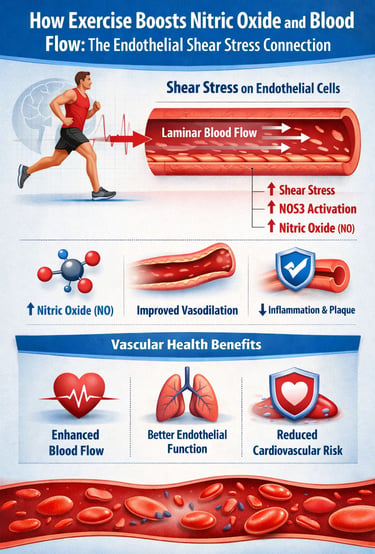
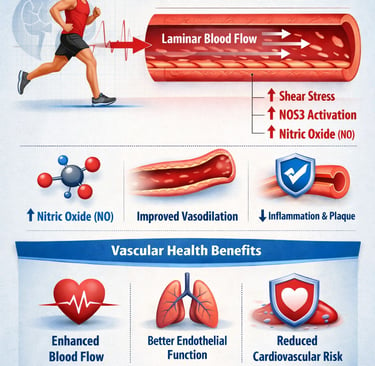
Exercise protects your heart not just by improving cholesterol or blood pressure, but also by generating endothelial shear stress—a frictional force created as blood flows along the vessel wall. This mechanical signal activates the NOS3 pathway, increasing nitric oxide production, improving vessel dilation, and reducing inflammation. Even a single workout can enhance endothelial function, measured by flow-mediated dilation, while regular training builds long-term vascular resilience. In simple terms, movement directly “talks” to your blood vessels—keeping them flexible, healthy, and resistant to disease.
Clinician’s Editorial: Why Endothelial Shear Stress Should Reshape How We Prescribe Exercise
We have overemphasized risk factors and underemphasized mechanisms.
For decades, cardiovascular prevention has revolved around cholesterol, blood pressure, and glucose. Yet these are downstream markers. The upstream regulator—endothelial shear stress—is rarely discussed in clinical practice, despite being fundamental to vascular homeostasis.Exercise is not just metabolic—it is mechanotherapy.
When patients engage in aerobic activity, they are not simply “burning calories.” They are generating laminar shear stress that directly signals endothelial cells to produce nitric oxide via the NOS3 pathway. This reframes exercise as a targeted vascular intervention rather than a lifestyle add-on.Endothelial dysfunction is reversible—if we act early.
We often encounter patients at the stage of established atherosclerosis, where structural disease dominates. However, endothelial dysfunction precedes plaque formation by years. Evidence shows that even a single exercise session can improve vascular responsiveness, highlighting a critical window for early intervention.Intensity and dose matter more than we admit.
Generic advice such as “walk more” is insufficient. Data on cerebral and systemic circulation demonstrate that higher intensity and adequate duration are required to activate shear-mediated pathways fully. Exercise prescription should be as precise as pharmacotherapy.VO₂ max should be treated as a vital sign.
Improvements in cardiorespiratory fitness are tightly linked to endothelial recovery. Yet VO₂ max remains underutilized in routine practice. It is not merely a fitness metric—it is a surrogate for vascular resilience.The future of cardiovascular care is integrative.
Pharmacological advances remain essential, but they do not replace the biological signals induced by movement. The convergence of molecular biology, exercise physiology, and clinical cardiology makes one conclusion unavoidable: structured exercise is a first-line therapy acting directly at the level of the endothelium.Building on the basics of how exercise restores endothelial function and reverses vascular aging (see companion article: Exercise and Vascular Health: How Nitric Oxide and Endothelial Function Keep Your Arteries Young
Every heartbeat does more than circulate blood—it generates a powerful mechanical signal that determines whether your arteries remain healthy or silently progress toward disease. This signal, known as endothelial shear stress, is the frictional force exerted by flowing blood on the inner lining of blood vessels. While often overlooked in traditional discussions of cardiovascular health, emerging research between 2024 and 2026 suggests that this force may be one of the most critical mediators of how exercise protects against heart disease.
When blood flow increases during physical activity, shear stress rises in a highly organized, laminar pattern. This mechanical stimulus is detected by endothelial cells and rapidly converted into biochemical signals that influence vascular tone, inflammation, and gene expression. One of the most important downstream effects is the activation of the NOS3 pathway, which drives the production of nitric oxide—a molecule essential for vasodilation and vascular protection (Conde et al., 2024). In parallel, exercise-induced shear stress enhances cerebral blood flow, with higher intensity and longer duration exercise producing greater increases in cerebrovascular shear and perfusion (Moir et al., 2024).
Importantly, these effects are not limited to elite athletes. Even a single bout of moderate-intensity exercise can significantly improve endothelial responsiveness, as measured by flow-mediated dilation, particularly in previously sedentary individuals (Zhang et al., 2024). Over time, repeated exposure to shear stress contributes to structural and functional vascular adaptations, closely linked to improvements in cardiorespiratory fitness and reductions in cardiovascular risk (McLellan et al., 2025).
Taken together, these findings reframe exercise not merely as a tool for burning calories or strengthening the heart, but as a direct regulator of vascular biology—one that operates through the fundamental language of blood flow and mechanical force.
30%: CVD risk reduction with regular aerobic exercise
NOS3: Key gene activated by shear stress during exercise
2×I: increase in cerebral shear stress at vigorous intensity
FMD: Gold standard measure of endothelial function
1. What Is Endothelial Shear Stress?
Imagine running your hand along the inside of a garden hose while water rushes through it. The friction your hand would feel is analogous to what the endothelium — the single-cell layer lining every blood vessel in your body — experiences with each heartbeat. The frictional drag created by moving blood is called endothelial shear stress.
The endothelium is far from passive. It is one of the most metabolically active tissues in the human body, covering a surface area equivalent to several tennis courts. Its cells are equipped with mechanosensors — specialised proteins that detect changes in flow rate and direction. When shear stress rises (as it does during physical activity), these sensors trigger gene expression, enzyme activation, and the release of vasoprotective molecules.
Mechano-sensing: Endothelial cells detect blood flow changes through surface ion channels and integrins.
Nitric Oxide Release: Shear stress activates eNOS (NOS3), producing NO, which dilates blood vessels.
Anti-inflammatory Action: Laminar shear reduces oxidative stress and suppresses pro-inflammatory gene expression.
Vascular Remodeling : Chronic exercise-induced shear promotes healthy outward vessel remodeling over time.
The key distinction scientists make is between laminar (smooth, unidirectional) and disturbed (turbulent, oscillatory) shear stress. Laminar shear — the type generated during steady, rhythmic aerobic exercise — is overwhelmingly protective. Disturbed shear, common at artery branch points and in sedentary individuals, is associated with plaque formation and early atherosclerosis.
Key Takeaway
Endothelial shear stress is not simply a byproduct of blood flow — it is an active biological signal that keeps your blood vessels healthy, flexible, and plaque-free.
2. The NOS3 Gene: Exercise's Molecular Switch
One of the most exciting frontiers in exercise biology involves understanding exactly how shear stress translates into health benefits at the molecular level. A 2024 study by Conde et al., published in Medicine & Science in Sports & Exercise, has shed remarkable light on this question.
The researchers investigated what happens to the NOS3 gene — also known as endothelial nitric oxide synthase — when endothelial cells are exposed to the pattern of shear stress generated during acute exercise in a controlled laboratory setting.
NOS3 encodes the enzyme eNOS (endothelial nitric oxide synthase), which produces nitric oxide (NO) — a gaseous signaling molecule that causes blood vessels to relax and widen, reducing blood pressure and improving blood flow. What Conde and colleagues demonstrated is that exercise-induced shear stress does not merely activate existing eNOS protein; it triggers the translation of NOS3 mRNA itself — meaning exercise tells cells to manufacture more of this protective enzyme from scratch.
This finding is significant for several reasons. First, it suggests that the cardiovascular benefits of exercise operate partly through de novo protein synthesis in the endothelium, not just acute signaling. Second, it provides a cellular explanation for why regular exercise — not just a single bout — is required to achieve lasting cardiovascular protection. Every session reinforces the molecular machinery.
"Exercise doesn't just make your heart beat faster — it rewrites the instructions in your vessel walls for producing the molecules that keep arteries healthy."
What Does This Mean for You?
Think of each workout as a trigger that tells your endothelial cells to build more of their protective toolkit. The more consistently you exercise, the more NOS3-derived nitric oxide your vessels can produce — and the more resilient your cardiovascular system becomes.
3. Your Brain on Exercise: Cerebral Shear Stress and Blood Flow
Most discussions of exercise and cardiovascular health focus on the heart and peripheral arteries. But a 2024 study from Moir and colleagues draws attention to a critically important vascular territory that benefits from exercise-induced shear stress: the brain.
The researchers examined how both the intensity and duration (dose) of aerobic exercise independently and jointly influence shear stress in cerebral arteries — particularly the middle cerebral artery, a key supplier of blood to the brain's working regions.
Their findings were nuanced and important: higher intensity exercise produced greater increases in cerebral shear stress, but the dose (how long you exercise) also made a meaningful independent contribution. Crucially, the combination of moderate-to-vigorous intensity with adequate duration yielded the most robust cerebrovascular shear stress response.
Brain Health Implication
Regular aerobic exercise at adequate intensity promotes cerebral vascular health through shear-stress-driven mechanisms that may help delay cognitive decline and reduce stroke risk.
For patients concerned about brain aging, dementia, or stroke risk, this research provides direct, mechanistic justification for exercise prescriptions that prioritize both adequate intensity and sufficient duration — not just "some movement." The data suggests that leisurely walking, while beneficial, may not fully activate the cerebral shear stress pathways that vigorous walking or cycling can.
4. FMD & Vascular Health: How Exercise Affects Young Adults Differently
One question that often goes unexplored is how the vascular response to exercise differs between trained athletes and physically inactive young adults. A 2024 study by Zhang et al. in Scientific Reports investigated exactly this, using flow-mediated dilation (FMD) as the primary measure of endothelial function.
FMD measures how much an artery widens in response to increased blood flow (shear stress) after a brief period of restricted circulation. It is considered one of the gold-standard non-invasive assessments of endothelial health. A higher FMD response = healthier, more responsive endothelium.
Zhang and colleagues found that trained individuals had significantly better baseline endothelial function than untrained counterparts. But here is the clinically relevant twist: untrained participants showed greater acute FMD improvement after a single moderate-intensity exercise session, suggesting that previously sedentary individuals may experience more dramatic immediate vascular benefits when they begin exercising — even before chronic training adaptations set in.
This research carries a powerful message for healthcare providers and public health communicators: it is never too late to start. The vascular system responds rapidly and measurably to even a single bout of aerobic exercise, and those who have been inactive may see the most dramatic early gains.
5. Training Adaptations, Cardiorespiratory Fitness, and Endothelial Dysfunction
While acute exercise produces immediate shear-stress benefits, chronic training engraves these changes deeper into the cardiovascular system. A 2025 secondary analysis by McLellan and colleagues, published in the Journal of Science in Sport and Exercise, examined the relationships between training-induced adaptations, cardiovascular risk factors, fitness, and vascular health.
The analysis revealed that exercise training-mediated improvements in cardiovascular risk factors — including blood pressure, lipid profiles, and insulin sensitivity — were significantly associated with improvements in endothelial function. Importantly, cardiorespiratory fitness (VO₂ max) emerged as a key mediator: individuals who improved their fitness most through training showed the greatest vascular health gains.
This is powerful evidence that endothelial function is not a fixed biological trait — it is a dynamic, trainable parameter. The same pathways activated by shear stress during each workout gradually build a more capable, less inflamed, and more resilient vascular system over weeks and months of consistent training.
Clinical Insight
Improving VO₂ max through structured aerobic training is one of the most evidence-backed strategies for reversing endothelial dysfunction — a precursor to cardiovascular disease, stroke, and type 2 diabetes.
6. Practical Applications for Your Health
Start with 20–30 Min of Brisk Walking
Even a single moderate-intensity session significantly improves FMD. The untrained endothelium is highly responsive. Start today — you do not need a gym.
Include Vigorous Sessions Weekly
Higher intensity aerobic exercise generates greater cerebral and peripheral shear stress. Aim for at least 2 vigorous sessions per week (e.g., cycling, running, swimming).
Train Regularly to Build NOS3 Reserves
Because NOS3 mRNA translation requires repeated shear stress signals, regularity matters. Three to five aerobic sessions per week sustain the molecular machinery.
Don't Cut Workouts Short
Duration independently increases shear stress benefits (Moir et al., 2024). Aim for sessions of at least 30–45 minutes to maximise post-exercise vascular response.
Ask About FMD Testing
Flow-mediated dilation testing provides an early window into endothelial health. If you have cardiovascular risk factors, ask your doctor about this non-invasive screening.
Improve VO₂ Max for Vascular Gains
McLellan et al. (2025) confirm that gains in cardiorespiratory fitness mediate vascular health improvement. Track your fitness progress — it is a true cardiovascular biomarker.
Take Charge of Your Vascular Health Today
Every workout is an investment in your endothelial health. Speak to a cardiologist or exercise physiologist about a program tailored to your cardiovascular risk profile.Read the FAQs First ↓
Frequently Asked Questions
1. What is endothelial shear stress in simple terms?
Endothelial shear stress (ESS) is the frictional force or "dragging" sensation created by blood flowing across the inner lining of your blood vessels. Think of it as a mechanical massage for your arteries; when blood flows quickly and smoothly (laminar flow), it signals the vessel walls to release protective chemicals that prevent plaque buildup and keep arteries flexible.
2. How does exercise activate the NOS3 gene?
Exercise increases blood flow velocity, which boosts endothelial shear stress. This mechanical force triggers the NOS3 gene to translate mRNA into new eNOS proteins. These proteins are the "factories" that produce nitric oxide, a vital gas that dilates blood vessels, lowers blood pressure, and prevents arterial hardening.
3. Which exercise is best for endothelial health?
Rhythmic aerobic exercise—such as brisk walking, cycling, or swimming—is the gold standard for endothelial health. These activities create laminar shear stress, which is anti-inflammatory. While moderate intensity is effective, incorporating vigorous intensity (70–85% Max Heart Rate) provides superior benefits for cerebral (brain) blood flow and vascular remodeling.
4. Can heart disease patients benefit from shear stress?
Yes. Controlled exercise-induced shear stress is a powerful therapeutic tool for cardiovascular rehabilitation. It helps "re-train" the endothelium to produce nitric oxide, which can improve blood flow even in vessels narrowed by plaque. Note: Patients with diagnosed heart disease should only exercise under a physician's supervision using a heart-rate-monitored protocol.
5. What is Flow-Mediated Dilation (FMD) testing?
Flow-Mediated Dilation (FMD) is the non-invasive "gold standard" test for vascular health. It uses ultrasound to measure how much an artery widens (dilates) after a brief period of restricted blood flow. A high FMD percentage indicates a healthy, responsive endothelium, while a low percentage is a primary early warning sign of future cardiovascular disease.
6. How long does it take to improve vascular health?
You can see vascular improvements in as little as one exercise session. Research shows that "untrained" individuals experience an immediate spike in endothelial function (FMD) after a single workout. However, chronic adaptations—like permanent changes in gene expression and vessel structure—typically require 4 to 8 weeks of consistent training (3+ times per week).
7. How does shear stress research help kidney disease?
In regenerative medicine, researchers use microfluidic shear stress to grow functional blood vessels in kidney organoids (lab-grown mini-organs). Because kidney filters are highly dependent on healthy microvessels, understanding shear stress allows scientists to model kidney diseases more accurately and develop bioengineered tissues for future transplants.
Clinical Pearls
1. The "De Novo" Protein Pearl
Scientific Perspective: Acute laminar shear stress doesn't just activate existing eNOS; it triggers NOS3 mRNA translation. This signifies that exercise acts as a stimulus for de novo protein synthesis, fundamentally increasing the "nitric oxide factory" capacity of the vessel.
Think of exercise as a "software update" for your blood vessels. It doesn't just turn on the equipment you already have; it actually tells your body to build new tools to keep your arteries relaxed and open.
2. The "Untrained Sensitivity" Pearl
Scientific Perspective: Sedentary individuals often exhibit a higher relative magnitude of FMD (Flow-Mediated Dilation) improvement after an initial bout of exercise compared to trained athletes. This suggests the "vasculature of the inactive" has a high ceiling for immediate functional recovery.
You get the biggest "bang for your buck" right at the start. Even if you haven’t worked out in years, your very first session begins repairing your blood vessels immediately. You don't have to be an athlete to see life-saving changes.
3. The "Cerebral Dose-Response" Pearl
Scientific Perspective: While moderate intensity is beneficial, vigorous intensity combined with longer duration ($>30$ minutes) creates a synergistic increase in middle cerebral artery shear stress. This is critical for neurovascular coupling and long-term cognitive resilience.
To protect your brain from aging, intensity matters. A stroll is good, but getting "out of breath" (vigorous intensity) is what really sends a surge of protective fluid through the vessels in your brain, acting like a "deep clean" for your cognitive health.
4. The "Laminar vs. Disturbed" Pearl
Scientific Perspective: Only laminar (steady) flow is atheroprotective. Disturbed or oscillatory flow (often found at arterial junctions or caused by physical inactivity) promotes pro-inflammatory gene expression. Consistent aerobic rhythm is the primary driver of the laminar signal.
Your blood vessels love rhythm. Steady, rhythmic exercise like jogging, cycling, or swimming creates "smooth" blood flow that coats your arteries in protective chemicals. Sitting still too long makes blood flow "choppy," which can irritate the lining of your heart's pipes.
5. The "Fitness as a Mediator" Pearl
Scientific Perspective: VO₂ max is more than an aerobic metric; it is a surrogate marker for endothelial health. Improvements in cardiorespiratory fitness (CRF) are directly correlated with the reversal of endothelial dysfunction, independent of weight loss.
Don't just watch the scale; watch your "fitness score." As you get faster or stronger and your heart gets more efficient (VO₂ max), it’s a sign that the inner lining of your entire body is becoming more resilient and youthful.
6. The "Kidney-Vascular Link" Pearl
Scientific Perspective: Emerging organoid research confirms that shear stress is a morphogenetic requirement for functional vascularization. Without flow-induced stress, microvascular networks fail to mature, which has profound implications for chronic kidney disease (CKD) management.
Blood flow isn't just about moving oxygen; it’s about "shaping" your organs. The same forces you create during a workout are the same ones scientists are using in labs to try and grow healthy kidneys. Movement is a literal "building block" for organ health.
Author’s Note
As a clinician trained in internal medicine, my approach to cardiovascular disease has always been grounded in measurable risk factors—lipids, blood pressure, glycemic control. Yet over years of clinical practice and engagement with emerging literature, it has become increasingly clear that these markers, while important, do not fully capture the dynamic biology of vascular health. This article was written to highlight a less visible but fundamentally important regulator: endothelial shear stress.
What makes this concept compelling is its ability to connect multiple domains—molecular signaling, exercise physiology, and clinical outcomes—into a single, coherent framework. The activation of pathways such as NOS3 and the measurable improvements in flow-mediated dilation illustrate that vascular health is not static; it is continuously shaped by behavior, particularly movement.
The goal of this work is not to replace established therapies, but to reframe how we think about them. Exercise is often presented to patients as supportive or preventive. The evidence, however, suggests it functions as a direct biological intervention at the level of the endothelium—one that complements and, in some cases, amplifies pharmacological strategies.
This article synthesizes findings from recent studies (2024–2026), but it also reflects a broader clinical perspective: that meaningful cardiovascular prevention must begin earlier, target mechanisms rather than just markers, and empower patients with actionable insight. If this piece encourages even a shift in how exercise is prescribed or understood in practice, it will have served its purpose.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Individual circumstances vary, and treatment decisions should always be made in consultation with qualified healthcare professionals.
Related Articles
VO₂ Max in Cardiology: The Missing Vital Sign for Cardiovascular Risk and Longevity
Is Your Heart at Risk? How the TG/HDL Ratio Can Warn You Early | DR T S DIDWAL
Exercise and Vascular Health: How Nitric Oxide and Endothelial Function Keep Your Arteries Young
References
Conde, D., Garcia, M., Gomez, M., & Gurovich, A. (2024). Acute exercise-induced endothelial shear stress activates NOS3 mRNA translation in vitro. Medicine & Science in Sports & Exercise, 56(10S), 47–48. https://doi.org/10.1249/01.mss.0001052904.28406.57
McLellan, H. L., Dawson, E. A., Hopkins, N. D., et al. (2025). Relation between endothelial dysfunction and exercise training-mediated adaptation in cardiovascular risk factors, cardiorespiratory fitness, and vascular health in humans: A secondary analysis. Journal of Science in Sport and Exercise, 7, 197–205. https://doi.org/10.1007/s42978-023-00270-9
Moir, M. E., Corkery, A. T., Miller, K. B., Pearson, A. G., Loggie, N. A., Apfelbeck, A. A., Howery, A. J., & Barnes, J. N. (2024). The independent and combined effects of aerobic exercise intensity and dose differentially increase post-exercise cerebral shear stress and blood flow. Experimental Physiology, 109, 1796–1805. https://doi.org/10.1113/EP091856
Shioda, H., Tang, T.-H., Raykhel, I., Sakai, Y., & Nishikawa, M. (2026). Kidney organoid vascularization: Current advancements in the field. Regenerative Therapy, 32, 101087. https://doi.org/10.1016/j.reth.2026.101087
Zhang, Y., Chai, S., Dai, H., et al. (2024). Vascular endothelial function and its response to moderate-intensity aerobic exercise in trained and untrained healthy young men. Scientific Reports, 14, 20450. https://doi.org/10.1038/s41598-024-71471-7