Vitamin K2 Benefits for the Heart: New Research on MK-7, Arterial Calcification, and Brain Health
Discover vitamin K2 benefits for heart health. Learn how MK-7 may reduce arterial calcification, support brain health, and regulate calcium metabolism.
NUTRITION
Dr. T.S. Didwal, M.D.(Internal Medicine)
3/15/202617 min read
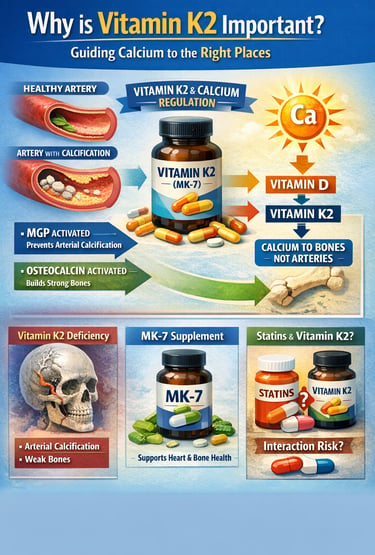
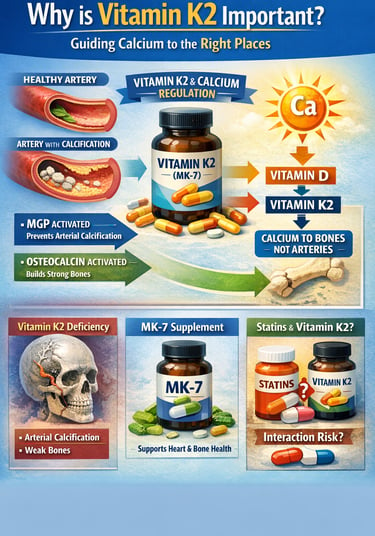
Vitamin K2 is a fat-soluble nutrient that helps regulate calcium metabolism in the body. It activates proteins such as osteocalcin and matrix Gla protein that direct calcium into bones and prevent it from accumulating in arteries, supporting heart health, bone strength, and healthy vascular function.
Calcium is essential for life. It strengthens bones, powers muscle contractions, and supports nerve signaling. But calcium in the wrong place can become dangerous. When calcium deposits accumulate in artery walls instead of bones, they contribute to arterial stiffening, coronary artery disease, and heart attacks. The key question modern nutritional science is asking is surprisingly simple: what directs calcium to the right place in the body?
A growing body of research suggests that the answer may lie in a nutrient that most people have never heard of—vitamin K2.
The benefits of vitamin K2 extend far beyond its traditional association with blood clotting. Unlike vitamin K1, which primarily functions in the liver, vitamin K2 works throughout the body to activate proteins that regulate calcium metabolism. Two of the most important are osteocalcin, which binds calcium into bone, and Matrix Gla Protein (MGP), which prevents calcium from accumulating inside arteries (Yan et al., 2023; Zhang et al., 2024). Without adequate vitamin K2, these proteins remain inactive, potentially allowing calcium to drift into soft tissues instead of skeletal structures.
This is why researchers increasingly view vitamin K2 for arteries as a critical component of cardiovascular health. Observational studies and clinical trials suggest that higher vitamin K2 intake is associated with lower coronary artery calcification and improved arterial flexibility (Zhao et al., 2024). In other words, vitamin K2 may help keep blood vessels elastic rather than turning into rigid, calcium-laden pipes.
The story becomes even more interesting when we consider the relationship between vitamin K2 and calcium regulation. Vitamin D increases calcium absorption from the intestine, but vitamin K2 helps determine where that calcium ultimately ends up—in bones rather than arteries. This Vitamin D + K2 synergy mechanism is increasingly recognized in metabolic and bone research (Yan et al., 2023).
Modern diets, however, contain far less K2 than traditional diets rich in fermented foods. As a result, vitamin K2 deficiency symptoms—such as vascular calcification, bone fragility, and impaired calcium metabolism—may be far more common than most clinicians realize (Zhang et al., 2024).
For people who struggle to obtain enough through food, MK-7 supplements, a long-acting form of vitamin K2, are now being widely studied for their potential role in protecting cardiovascular and skeletal health (Zhao et al., 2024).
Key Takeaways
Vitamin K2 activates proteins that direct calcium into bones.
Low K2 levels may allow calcium buildup in arteries.
MK-7 supplements have the longest half-life and strongest clinical evidence.
Vitamin D and K2 work together to regulate calcium metabolism.
Clinical Pearls
1. The Vascular Calcification Paradox
Scientific Perspective: Vitamin K2 is the essential cofactor for the $\gamma$-carboxylation of Matrix Gla Protein (MGP). In its active form, MGP binds free calcium in the bloodstream, preventing it from depositing in the tunica media of arterial walls. Recent data (Ahmed et al., 2025) confirms that low K2 status is a direct correlate of obstructive coronary artery disease.
Think of Vitamin K2 as a "traffic cop" for calcium. Without it, calcium is "unsupervised" and ends up hardening your arteries like old PVC pipes. K2 makes sure the calcium stays out of your heart and goes where it’s actually needed.
2. Osteoblast Protection via Ferroptosis Inhibition
Scientific Perspective: Beyond mineralization, K2 acts as an antioxidant regulator. Tao et al. (2025) demonstrated that K2 upregulates CBR1 via the Nrf2/Keap1 pathway. This prevents ferroptosis—an iron-dependent form of cell death—in osteoblasts, particularly under inflammatory stress from PGE2.
Bone health isn't just about "building" bone; it’s about keeping your bone-building cells alive. Inflammation (from age or illness) can "rust" and kill these cells. K2 acts like an anti-rust coating, protecting your bone-building crew so they can keep working.
3. The D3-K2 Synergistic Axis
Scientific Perspective: Vitamin D3 increases the production of Vitamin K-dependent proteins (VKDPs) like osteocalcin and MGP. However, D3 alone cannot activate them. Without sufficient K2, these proteins remain undercarboxylated (inactive), potentially leading to "hypervitaminosis D" effects where calcium is absorbed but mismanaged.
Vitamin D3 is the "loader" that brings calcium into the body, but K2 is the "driver" that takes it to the destination. Taking high doses of Vitamin D without K2 is like hiring a delivery crew that leaves the packages on the sidewalk instead of putting them inside the house.
4. Neurological Epigenetics & Sphingolipids
Scientific Perspective: K2 (specifically the MK-4 subtype) is highly concentrated in the brain. It is involved in the synthesis of sphingolipids, which form the myelin sheath. Emerging research (Roumeliotis et al., 2025) suggests K2 also acts as an epigenetic modulator, altering DNA methylation to suppress neuroinflammatory genes.
K2 helps maintain the "insulation" on your brain's wiring. It also speaks to your genes, telling them to "turn down the volume" on inflammation that leads to brain fog and memory loss as you age.
5. Insulin Sensitivity and Metabolic Health
Scientific Perspective: Carboxylated osteocalcin acts as a hormone that travels from the bone to the pancreas and adipose tissue. It enhances insulin secretion from $\beta$-cells and improves the insulin sensitivity of muscle cells. K2 deficiency is increasingly linked to metabolic syndrome and insulin resistance (Zhang et al., 2024).
Your bones actually talk to your metabolism. When K2 activates your bone proteins, they send a signal to your body to help process sugar more efficiently. This makes K2 a quiet but powerful ally in managing weight and blood sugar.
6. The Half-Life Advantage: MK-4 vs. MK-7
Scientific Perspective: While MK-4 is critical for rapid tissue use (brain/skin), its half-life is only 1–2 hours. MK-7 has a half-life of roughly 72 hours, allowing for stable blood levels and better distribution to peripheral tissues like the vasculature and bones. Meta-analyses (Zhao et al., 2024) favor MK-7 for long-term cardiovascular stiffness reduction.
Not all K2 is the same. MK-4 is like a "quick snack" for your cells, while MK-7 is like a "slow-cooker meal" that stays in your system for days. For protecting your heart and bones long-term, the long-lasting MK-7 form provides much more consistent coverage.
1. What Exactly Is Vitamin K2?
Vitamin K is a fat-soluble vitamin that exists in two principal forms. Vitamin K1 (phylloquinone) is found abundantly in leafy green vegetables like kale, spinach, and broccoli, and its primary role is supporting blood clotting through activation of clotting factors in the liver. Vitamin K2 (menaquinone), on the other hand, is found mainly in fermented and animal-based foods, and its primary roles lie outside the liver — particularly in the cardiovascular system, bones, and, as we now know, the brain.
The "K2" family is not a single molecule. It includes a spectrum of subtypes, known as MK-4 through MK-13, named after the length of their side chain. Among these, MK-4 and MK-7 are the most biologically studied. MK-7, found abundantly in the Japanese fermented soybean dish natto, is notable for its long half-life in the bloodstream — roughly three days, compared to MK-4's one to two hours — which may make it more effective at reaching peripheral tissues like arteries and bones (Yan et al., 2023).
Key distinction: K1 vs K2
Vitamin K1 (phylloquinone) supports blood clotting in the liver. Vitamin K2 (menaquinone) directs calcium into bones and teeth, and keeps it out of arteries and soft tissues. They are absorbed, distributed, and used very differently in the body.
Dietary sources of vitamin K2 include fermented cheeses, egg yolks, chicken (especially dark meat), grass-fed butter, and natto. The average Western diet is noticeably sparse in these foods, which explains why deficiency is far more prevalent than most clinicians appreciate. Western populations who rely heavily on low-fat processed foods are especially likely to fall short (Zhang et al., 2024).
2. How Vitamin K2 Works Inside Your Body
Understanding why K2 matters requires a brief look at the molecular machinery it activates. The defining biochemical action of all K vitamins is their role as a cofactor in a process called gamma-carboxylation. Without adequate vitamin K, a class of proteins called vitamin K–dependent proteins (VKDPs) remain in an inactive, undercarboxylated form (Yan et al., 2023).
Key Proteins Activated by Vitamin K2
Two VKDPs deserve special attention here. The first is osteocalcin, produced by bone-building cells (osteoblasts). When carboxylated by K2, osteocalcin properly binds calcium into the bone matrix. Without K2, osteocalcin floats inactive in the bloodstream, unable to do its job, and calcium may end up deposited in arterial walls instead of bone (Zhang et al., 2024).
The second is Matrix Gla Protein (MGP) — arguably the body's most potent inhibitor of arterial calcification. MGP is produced locally in vascular smooth muscle cells and acts as a gatekeeper, preventing calcium crystals from forming in the arterial walls. This function is entirely dependent on K2-mediated carboxylation. Undercarboxylated MGP is essentially a broken lock on the calcium gate, and the consequence can be measurable calcification of coronary arteries over time (Yan et al., 2023).
Beyond carboxylation, K2 is now understood to influence gene expression, anti-inflammatory pathways, and mitochondrial function — particularly in neural tissue. Roumeliotis et al. (2025) describe K2 as an "epigenetic modulator," capable of altering DNA methylation and histone modification patterns that regulate how genes are switched on or off in the brain. This layer of complexity is only beginning to be understood.
3. Vitamin K2 Supplementation and Cardiovascular Risk: What the Research Shows
One of the most comprehensive analyses of vitamin K supplementation and heart health was published by Zhao Q.Y. and colleagues in 2024 in the Journal of Nutritional Science. This systematic review and meta-analysis examined multiple randomized controlled trials to understand how vitamin K affects cardiovascular risk factors.
Their findings suggest that vitamin K—particularly vitamin K2 in the form of MK-7—may have measurable benefits for vascular health.
Across the analyzed trials, researchers evaluated several important cardiovascular markers, including:
Arterial stiffness, measured by pulse wave velocity
Coronary artery calcification (CAC) scores
Blood pressure
Cholesterol and lipid profiles
The results revealed several important patterns.
First, supplementation with vitamin K2 (especially MK-7) was associated with slower progression of vascular calcification, particularly in people who already had elevated baseline calcification. This is important because calcified arteries lose their flexibility and become more rigid, increasing the risk of heart attack and stroke.
Second, several studies found that arterial stiffness improved modestly after six months to three years of MK-7 supplementation.
Third, the effects on cholesterol were more mixed. Some studies reported small reductions in LDL cholesterol and oxidized LDL, while others showed neutral results.
A simple way to understand it
Think of your arteries as flexible rubber hoses. Over time, calcium deposits can gradually turn them into stiff pipes. Vitamin K2 helps regulate calcium metabolism, guiding calcium away from artery walls and toward bones where it belongs.
Researchers emphasize that the optimal dose and duration of vitamin K2 supplementation for cardiovascular protection still need to be determined. Because the trials differed in dose, population, and study design, the exact magnitude of benefit remains uncertain. However, the overall trend of evidence is consistent and supported by well-understood biological mechanisms involving matrix Gla protein (MGP) and osteocalcin.
4. Vitamin K2 Deficiency and Coronary Artery Disease
While supplementation studies examine what happens when people take vitamin K2, other research asks a different question: who is actually deficient in vitamin K2, and how does that relate to disease?
A case–control study by Ahmed et al.(2025 ) explored this question by comparing patients with confirmed coronary artery disease (CAD) to healthy individuals.
The results were striking.
People with coronary artery disease were far more likely to show signs of vitamin K2 deficiency than healthy controls.
Researchers measured two important markers of vitamin K2 activity:
Undercarboxylated Matrix Gla Protein (dp-ucMGP)
Undercarboxylated osteocalcin
Both markers indicate whether vitamin K–dependent proteins are properly activated in the body.
Patients with coronary artery disease had significantly higher levels of these inactive proteins, suggesting that vitamin K2 was insufficient to activate them properly.
Interestingly, the researchers also found that dietary vitamin K2 intake was lower in patients with CAD.
Importantly, these associations remained significant even after adjusting for major cardiovascular risk factors such as:
age
smoking
diabetes
hypertension
cholesterol-lowering medications
This suggests that vitamin K2 status may play an independent role in coronary artery health.
However, it is important to understand the limitations of this type of study. Case–control research can show associations but cannot prove causation. People with heart disease may have generally poorer diets, and vitamin K2 may be just one part of a broader nutritional pattern.
Nevertheless, the biological mechanism is compelling: when vitamin K2 is insufficient, matrix Gla protein cannot effectively block calcium buildup inside arteries, increasing the risk of vascular calcification.
Should you get tested?
A laboratory marker called dp-ucMGP is considered one of the most reliable indicators of vitamin K2 status. However, this test is not routinely included in standard blood panels. If you have cardiovascular risk factors, discussing vitamin K2 status with your healthcare provider may be worthwhile.
5. Where the Evidence Stands Today: A Clinical Perspective
A comprehensive review published in 2024 by Zhang T. and colleagues in the journal Foods examined the broader role of vitamin K2 in health and disease.
The authors reviewed evidence across several major health conditions, including:
cardiovascular disease
osteoporosis
chronic kidney disease
metabolic syndrome
cancer
Among these areas, the link between vitamin K2 and vascular calcification appears to be one of the most well-supported.
One of the most influential studies in this field is the Rotterdam Study, which followed thousands of participants over time. Researchers found that individuals with higher dietary intake of vitamin K2 had significantly lower rates of coronary artery calcification and cardiovascular mortality.
Vitamin K2 and kidney disease
Patients with chronic kidney disease, particularly those undergoing dialysis, often show extremely high levels of inactive MGP. This suggests severe vitamin K deficiency at the tissue level. Because these patients frequently experience accelerated vascular calcification, improving vitamin K2 status is an area of active research.
Safety profile of vitamin K2
The clinical review also highlighted an important point: vitamin K2 has an excellent safety record. Unlike some fat-soluble vitamins such as vitamin A or D, no clear toxicity threshold has been established for vitamin K2 at nutritional doses.
However, patients taking anticoagulant medications such as warfarin should always consult their physician before starting any vitamin K supplementation.
6. Vitamin K2 and Brain Health: A New Frontier
While vitamin K2 is widely known for its roles in cardiovascular and bone health, scientists are increasingly interested in its potential effects on the brain and nervous system.
Research summarized by Yan Q. and colleagues (2023) shows that the brain contains relatively high concentrations of MK-4, a form of vitamin K2.
This suggests that the brain actively absorbs and uses vitamin K2 for important neurological functions.
Vitamin K2 appears to support brain health in several ways:
helping produce sphingolipids, key components of the myelin sheath that insulates nerve fibers
activating Gas6 proteins, which promote neuron survival
reducing neuroinflammation
Low vitamin K2 levels have been linked in observational studies to increased neuroinflammation and poorer cognitive outcomes in older adults.
Animal studies further show that vitamin K2 deficiency can impair sphingolipid production and cognitive performance.
The Epigenetic Dimension
An especially intriguing development comes from research by Roumeliotis et al. (2025) published in Epigenomics.
This study explored how vitamin K2 might influence epigenetics, the biological mechanisms that control how genes are switched on or off.
Epigenetic regulation includes processes such as:
DNA methylation
histone modification
These mechanisms influence whether certain genes are active or silent, affecting inflammation, aging, and disease risk.
Emerging evidence suggests that vitamin K2 may help regulate genes involved in neuroinflammation, neuronal survival, and neurodegeneration.
Although much of this research is still based on laboratory and animal studies, the findings suggest vitamin K2 could play an important role in brain aging and neurodegenerative diseases such as Alzheimer’s and Parkinson’s disease.
7. A New Discovery: Vitamin K2 and Ferroptosis in Bone Cells
A groundbreaking study by Tao et al (2025), published in Communications Biology, revealed a completely new way that vitamin K2 protects bone health.
Previously, vitamin K2 was mainly known for activating osteocalcin, which helps bind calcium into bone.
This study discovered another mechanism: vitamin K2 can protect osteoblasts (bone-building cells) from a destructive process known as ferroptosis.
What is ferroptosis?
Ferroptosis is a type of programmed cell death caused by the buildup of iron-driven oxidative damage inside cell membranes.
You can imagine it like a fire starting within the cell’s fatty membrane layers. If antioxidant defenses fail, the cell eventually collapses.
The study found that an inflammatory molecule called prostaglandin E2 (PGE2) can trigger ferroptosis in osteoblasts.
Vitamin K2 helps prevent this process by activating the Nrf2/Keap1 antioxidant pathway, which switches on protective genes. One of these genes produces carbonyl reductase 1 (CBR1), an enzyme that neutralizes toxic lipid oxidation products.
When vitamin K2 was present, osteoblasts were much more likely to survive inflammatory stress.
This discovery suggests that vitamin K2 supports bone health in three distinct ways:
Regulating calcium metabolism
Activating bone-building proteins
Protecting osteoblasts from oxidative cell death
8. Food Sources of Vitamin K2 and Supplementation
Unlike vitamin K1, which is abundant in leafy greens, vitamin K2 is found mainly in fermented foods and certain animal products.
Some of the richest natural sources include:
Natto (fermented soybeans) – the highest known dietary source of MK-7
Hard cheeses such as Gouda and Edam
Soft cheeses like Brie and Camembert
Egg yolks, particularly from pasture-raised chickens
Chicken liver
Grass-fed butter
Because these foods are less common in modern diets, many people may consume lower levels of vitamin K2 than traditional populations.
Vitamin K2 supplements
For individuals who struggle to obtain enough vitamin K2 through diet, supplements can be a convenient option.
The most widely studied form is MK-7, which remains in the bloodstream for several days and provides sustained biological activity.
Clinical trials have used doses ranging from 90 micrograms to 360 micrograms per day.
Since vitamin K2 is fat-soluble, it is best absorbed when taken with a meal containing some fat. Many supplements combine vitamin D3 and vitamin K2, reflecting their cooperative roles in regulating calcium metabolism.
Important precaution
Anyone taking blood-thinning medications such as warfarin should consult a healthcare professional before starting vitamin K supplementation.
How Vitamin D3, Vitamin K2, and Magnesium Work Together
Understanding calcium metabolism requires looking at three key nutrients that act in sequence. Each plays a different role in ensuring calcium is absorbed, transported, and used safely in the body.
1. Vitamin D3 – The Calcium Absorption Driver
Primary role: Enhances calcium absorption from the intestine.
Key mechanism: Activates calcium transport proteins such as TRPV6 in intestinal cells.
Physiological outcome: Increases the amount of calcium entering the bloodstream.
Clinical significance: Adequate vitamin D levels are essential for maintaining normal calcium balance and supporting bone mineralization.
2. Vitamin K2 – The Calcium Traffic Director
Primary role: Directs calcium to the correct tissues.
Key proteins activated:
Osteocalcin, which binds calcium into the bone matrix
Matrix Gla Protein (MGP), which prevents calcium deposition in arteries
Physiological outcome: Promotes strong bones while protecting arteries from calcification.
Clinical significance: Insufficient vitamin K2 may allow calcium to accumulate in soft tissues such as blood vessels.
3. Magnesium – The Metabolic Cofactor
Primary role: Serves as a cofactor for hundreds of enzymatic reactions involved in mineral metabolism.
Key mechanisms: Supports ATP-dependent enzymes and helps regulate vitamin D activation.
Physiological outcome: Maintains balanced calcium utilization and supports bone formation.
Clinical significance: Magnesium deficiency can impair vitamin D metabolism and disrupt normal calcium handling.
To Summarize
1. The “Calcium Paradox” of Modern Nutrition
Modern diets often provide abundant calcium and increasing levels of vitamin D supplementation, yet rates of osteoporosis and vascular calcification continue to rise globally. This paradox highlights a crucial regulatory factor: calcium must be properly directed within the body. Emerging research suggests that vitamin K2 acts as a molecular traffic controller, guiding calcium into bones while preventing deposition in arteries (Yan et al., 2023).
2. Vitamin K2 as a Cardiovascular Protector
Arterial calcification is no longer viewed as passive mineral accumulation but as an active, regulated biological process. Vitamin K2 activates Matrix Gla Protein (MGP), one of the body’s most potent inhibitors of vascular calcification. When K2 levels are insufficient, MGP remains inactive, allowing calcium crystals to accumulate in arterial walls. Clinical studies and meta-analyses indicate that higher K2 intake may help slow the progression of arterial stiffness and coronary calcification (Zhao et al., 2024).
3. A Critical Partner for Vitamin D
Vitamin D increases calcium absorption from the intestine. However, without sufficient vitamin K2, the body may lack the molecular tools needed to direct that calcium safely into skeletal tissue. This explains why many experts now emphasize the Vitamin D + K2 synergy mechanism, particularly in long-term bone and cardiovascular health strategies (Zhang et al., 2024).
4. Implications for Aging and Brain Health
Beyond cardiovascular and skeletal systems, vitamin K2 is increasingly recognized for roles in neurobiology and gene regulation. The brain contains high concentrations of MK-4, and experimental research suggests K2 may support neuronal survival, reduce neuroinflammation, and influence epigenetic pathways associated with cognitive aging (Roumeliotis et al., 2025).
5. A Nutrient Lost in the Modern Food System
Traditional diets rich in fermented foods and animal products supplied meaningful amounts of vitamin K2. Today, highly processed diets provide far less of this nutrient, making functional deficiency increasingly common.
6. The Preventive Medicine Opportunity
Taken together, the emerging evidence suggests that vitamin K2 may represent a small nutrient with disproportionately large implications for cardiovascular disease, osteoporosis, and possibly neurodegeneration. Ensuring adequate intake—through diet or carefully considered supplementation—may become an increasingly important component of future metabolic and cardiovascular prevention strategies.
Frequently Asked Questions (FAQs)
1. What does vitamin K2 do for the heart?
Vitamin K2 helps protect cardiovascular health by activating matrix Gla protein (MGP), a vitamin K–dependent protein that inhibits calcium deposition in the walls of arteries. When MGP is properly activated, it prevents calcium crystals from forming inside blood vessels, helping maintain arterial flexibility and reducing vascular calcification risk.
2. Can vitamin K2 reduce arterial calcification?
Research suggests that vitamin K2—especially the MK-7 form—may slow the progression of arterial calcification by activating proteins that regulate calcium metabolism. Clinical trials have shown improvements in arterial stiffness and vascular elasticity, although more long-term studies are needed to determine whether K2 can reverse established calcification.
3. What is the difference between vitamin K1 and vitamin K2?
Vitamin K1 (phylloquinone) is primarily involved in blood clotting and is abundant in leafy green vegetables. Vitamin K2 (menaquinone), found in fermented foods and animal products, works mainly outside the liver to regulate calcium metabolism in arteries, bones, and other tissues.
4. What are common symptoms of vitamin K2 deficiency?
Vitamin K2 deficiency often develops silently because there are no immediate symptoms. Over time, however, low K2 status may contribute to arterial calcification, reduced bone mineral density, and impaired calcium metabolism. Elevated levels of undercarboxylated matrix Gla protein (dp-ucMGP) are considered a functional marker of deficiency.
5. Is MK-7 the best form of vitamin K2?
MK-7 is one of the most widely studied forms of vitamin K2. It has a longer half-life in the bloodstream—up to several days—allowing it to remain active longer than MK-4, which is cleared from circulation more rapidly. Because of this, MK-7 is commonly used in dietary supplements.
6. Can vitamin K2 improve brain health?
Emerging research suggests vitamin K2 may support brain health through several mechanisms, including sphingolipid synthesis, anti-inflammatory signaling, and activation of Gas6 proteins that support neuron survival. Early studies also suggest K2 may influence epigenetic pathways involved in aging and neurodegeneration.
7. Should vitamin K2 be taken with vitamin D?
Many researchers recommend taking vitamin K2 with vitamin D because the two nutrients work together in calcium metabolism. Vitamin D increases calcium absorption, while vitamin K2 helps direct that calcium into bones and away from arteries, helping maintain balanced mineral distribution in the body.
Author’s Note
The science surrounding vitamin K2 has evolved rapidly over the past decade, moving this nutrient from the margins of nutritional research into the center of discussions about cardiovascular and metabolic health. Historically, vitamin K was primarily associated with blood clotting, a function largely attributed to vitamin K1. However, advances in molecular biology, nutritional epidemiology, and clinical trials have revealed that vitamin K2 plays distinct and far-reaching roles in human physiology.
In reviewing the literature for this article, I examined multiple peer-reviewed studies published between 2023 and 2025, including systematic reviews, meta-analyses, clinical investigations, and mechanistic laboratory research. Together, these studies provide a compelling scientific narrative: vitamin K2 appears to influence calcium metabolism, vascular biology, bone integrity, and potentially even brain health through mechanisms that are only now becoming fully understood.
It is important, however, to interpret this growing body of evidence with appropriate scientific caution. While observational studies and early clinical trials suggest promising associations between vitamin K2 status and reduced vascular calcification, improved bone metabolism, and potential neuroprotective effects, large long-term randomized trials are still needed to establish definitive clinical guidelines.
From a clinical perspective, the most valuable takeaway may be awareness. Modern dietary patterns—particularly those low in fermented foods and certain animal products—may provide less vitamin K2 than traditional diets. As research progresses, clinicians and patients alike may benefit from paying closer attention to this often overlooked micronutrient.
My goal in writing this article is not to promote supplementation indiscriminately, but rather to present the emerging scientific evidence in a clear, balanced, and clinically meaningful way. Understanding how nutrients interact with metabolic pathways allows us to move closer to the broader aim of preventive medicine: addressing disease risk before it manifests.
Medical disclaimer: This article is for informational and educational purposes only and does not constitute medical advice, diagnosis, or treatment. The information presented is based on peer-reviewed research but is not a substitute for professional medical consultation. Always speak with a qualified healthcare provider before making changes to your supplement regimen, especially if you have a medical condition or take prescription medications.
Related Articles
The Invisible Orchestra: How Calcium, Magnesium, and Vitamin D Work Together | DR T S DIDWAL
Can Omega-3 Boost Muscle Protein Synthesis? What the Latest Research Reveals | DR T S DIDWAL
Beyond the Low-Fat Myth: 6 New Studies Redefining Dietary Fat and Heart Health | DR T S DIDWAL
Can Plant-Based Polyphenols Lower Biological Age? | DR T S DIDWA
References
Ahmed, S. A., Yar, A. A., Ghaith, A. M., Alahmadi, R. N., Almaleki, F. A., Alahmadi, H. S., Almaramhy, W. H., Alsaedi, A. M., Alraddadi, M. K., & Ismail, H. M. (2025). Prevalence of vitamin K2 deficiency and its association with coronary artery disease: A case–control study. Diseases, 13(1), 12. https://doi.org/10.3390/diseases13010012
Roumeliotis, S., Cavallaro, R. A., Kontogiorgos, I., Neofytou, I. E., Maresz, K., Jeanne, J. F., … & Fuso, A. (2025). The epigenetic potential of vitamin K2 in brain health. Epigenomics, 17(10), 681–690. https://doi.org/10.1080/17501911.2025.2518916
Tao, L., Li, H., Wang, J., et al. (2025). Vitamin K2 inhibits PGE2-mediated osteoblast ferroptosis by upregulation of CBR1 via the Nrf2/Keap1 pathway. Communications Biology, 8, 1116. https://doi.org/10.1038/s42003-025-08564-0
Yan, Q., Zhang, T., O'Connor, C., Barlow, J. W., Walsh, J., Scalabrino, G., Xu, F., & Sheridan, H. (2023). The biological responses of vitamin K2: A comprehensive review. Food Science & Nutrition, 11(4), 1634–1656. https://doi.org/10.1002/fsn3.3213
Zhang, T., O'Connor, C., Sheridan, H., & Barlow, J. W. (2024). Vitamin K2 in health and disease: A clinical perspective. Foods, 13(11), 1646. https://doi.org/10.3390/foods13111646
Zhao, Q. Y., Li, Q., Hasan Rashedi, M., Sohouli, M., Rohani, P., & Velu, P. (2024). The effect of vitamin K supplementation on cardiovascular risk factors: A systematic review and meta-analysis. Journal of Nutritional Science, 13, e3. https://doi.org/10.1017/jns.2023.106