Muscle Quality and Insulin Resistance: Can You Really Reverse It?
Your muscles are key to glucose regulation. Discover how muscle quality influences blood sugar, insulin action, and metabolic flexibility.
DIABETESEXERCISE
Dr. T.S. Didwal, M.D.(Internal Medicine)
4/25/202617 min read
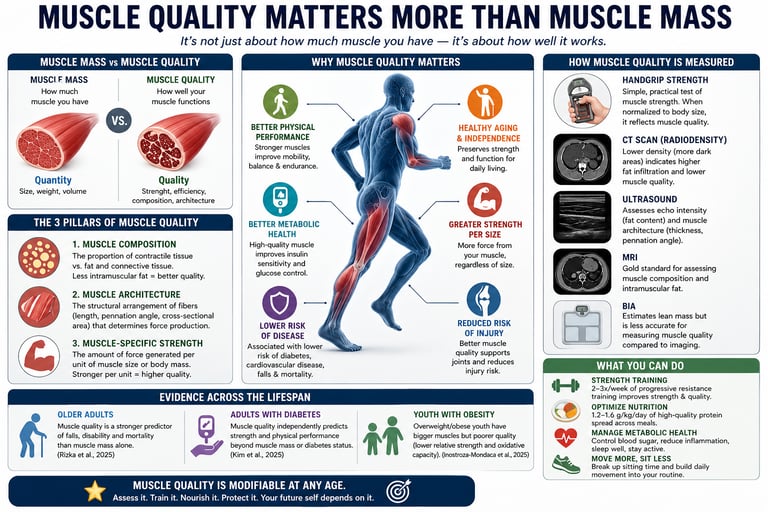

Muscle quality refers to how effectively skeletal muscle regulates metabolism, not just how much muscle is present. High-quality muscle has lower fat infiltration, better mitochondrial function, and greater insulin sensitivity, allowing efficient glucose uptake and energy utilization. Research shows that muscle quality is a stronger predictor of metabolic health, diabetes risk, and longevity than muscle mass alone.
Glucose uptake:
Muscle mass → depends on the total quantity of tissue
Muscle quality → depends on how efficiently the muscle uses glucoseInsulin sensitivity:
Muscle mass → weak or indirect association
Muscle quality → strong, independent predictorMitochondrial function:
Muscle mass → does not reflect energy production capacity
Muscle quality → directly linked to mitochondrial efficiencyFat infiltration (myosteatosis):
Muscle mass → does not capture intramuscular fat
Muscle quality → a key determinant of metabolic healthDiabetes risk:
Muscle mass → provides limited predictive insight
Muscle quality → strongly predicts risk and progression of type 2 diabetes
Clinician’s Perspective: Why Muscle Quality Must Enter Routine Practice
Shift from morphology to function-first assessment: Traditional reliance on lean mass (e.g., DEXA) risks underdiagnosis of clinically meaningful weakness. Current evidence supports prioritizing muscle-specific strength and performance (e.g., grip strength, sit-to-stand, gait speed) as primary screening tools, with mass as a secondary modifier (Kim et al., 2025; Rizka et al., 2025).
Recognize “normal-mass, low-quality” muscle phenotypes: Patients with preserved or even elevated muscle mass—common in obesity and type 2 diabetes—may exhibit reduced contractile efficiency and higher intramuscular fat (myosteatosis). These individuals carry disproportionate risks for disability, insulin resistance, and cardiometabolic events despite “acceptable” body composition profiles (Costa-Pereira et al., 2026).
Integrate muscle quality into metabolic care pathways: Skeletal muscle is a major site of glucose disposal. Declining muscle quality—via mitochondrial dysfunction, lipid infiltration, and inflammation—directly worsens glycemic control and insulin sensitivity. Assessing and targeting muscle quality should be considered part of comprehensive diabetes management (Kim et al., 2025).
Use pragmatic, scalable tools in the clinic:
Handgrip strength normalized to body weight (or BMI)
5× sit-to-stand test
Gait speed (<0.8 m/s as high risk)
Ultrasound echo intensity (where available)
These provide high signal-to-noise functional insights without reliance on advanced imaging.
Reframe sarcopenia diagnosis and risk stratification: Contemporary models emphasize strength and performance over mass. Incorporating muscle quality metrics improves identification of patients at risk for falls, hospitalization, and loss of independence (Rizka et al., 2025).
Prescribe targeted interventions:
Progressive resistance training (2–3×/week) to enhance neuromuscular efficiency and reduce myosteatosis
Protein optimization (≈1.2–1.6 g/kg/day in older or catabolic states) with leucine-rich sources
Metabolic control (glycemia, inflammation, sleep) to protect mitochondrial function
Monitor longitudinal change, not static values: Declines in relative strength often precede loss of mass. Serial tracking enables early intervention and better outcome prediction.
Adopt a multidisciplinary model: Collaboration with physiotherapists, dietitians, and exercise specialists is essential to operationalize muscle quality–focused care across aging and chronic disease populations.
Muscle health is undergoing a quiet but profound scientific redefinition. For decades, the dominant question in both clinical medicine and fitness science was deceptively simple: how much muscle do you have? From DEXA scans to body composition charts, muscle mass became the central metric used to assess strength, aging, and metabolic health. But emerging evidence from the latest wave of research suggests that this question, while important, is fundamentally incomplete. A more critical—and clinically meaningful—question is now taking center stage: how well does your muscle actually function?
This shift reflects a growing recognition that muscle quality, not just muscle quantity, determines real-world outcomes such as strength, mobility, metabolic resilience, and even survival. Across diverse populations—older adults at risk of frailty, individuals living with type 2 diabetes, and even children with obesity—the same pattern is emerging: individuals with similar muscle mass can have dramatically different levels of strength, endurance, and metabolic health depending on the quality of that muscle (Kim et al., 2025; Inostroza-Mondaca et al., 2025). In other words, two people may look similar on a scan, yet function very differently in daily life.
At a biological level, this divergence is driven by factors that traditional measurements often miss. Muscle tissue is not just inert mass—it is a dynamic organ influenced by fat infiltration, mitochondrial efficiency, neuromuscular coordination, and inflammatory signaling. When these elements are compromised, muscle becomes less efficient, less powerful, and more metabolically dysfunctional, even if its size appears preserved (Costa-Pereira et al., 2026). This helps explain why conditions such as aging, obesity, and diabetes can impair strength and physical performance long before significant muscle loss becomes visible.
The clinical implications are substantial. Poor muscle quality has been linked to reduced physical performance, increased risk of falls, impaired glucose metabolism, and higher mortality—often independent of muscle mass itself (Rizka et al., 2025). This challenges long-standing diagnostic frameworks, particularly in sarcopenia, where reliance on muscle quantity alone may overlook high-risk individuals.
What Is "Muscle Quality," Really? A Concept Being Redefined
The term "muscle quality" has been used loosely in scientific literature for years — and that vagueness has become a real problem. A landmark paper by Costa-Pereira et al. (2026), published in European Geriatric Medicine, directly confronts this issue, arguing that the phrase "muscle quality" is an imprecise umbrella term covering wildly different biological concepts depending on who is using it.
The term is widely used in both research and clinical settings, yet a universally accepted definition currently does not exist. Studies addressing "muscle quality" encompass a broad range of functional and morphological characteristics of skeletal muscle, leading to inconsistent interpretations.
To bring clarity, Costa-Pereira et al. (2026) propose that researchers and clinicians adopt three more precise sub-categories:
1. Muscle Composition — This refers to what your muscle tissue is actually made of. Healthy muscle is mostly contractile protein. But with aging, obesity, metabolic disease, and inactivity, fat begins to infiltrate the muscle fibers — a condition called myosteatosis or intramuscular fat deposition. Higher fat content within the muscle is linked to weaker muscle contractions, impaired insulin signaling, and increased mortality risk across multiple diseases.
2. Muscle Architecture — This describes the structural arrangement of muscle fibers, including their length, pennation angle (the angle at which fibers attach to the tendon), and cross-sectional area. These architectural features directly determine how efficiently a muscle can generate force and sustain movement.
3. Muscle-Specific Strength — Also called intrinsic muscle strength or relative strength, this is the amount of force a muscle can generate per unit of its cross-sectional area or body mass. A large muscle that produces relatively little force is, by definition, a low-quality muscle — regardless of its size.
This three-part framework is enormously practical. It moves us from a single blunt measurement (how much muscle do you have?) toward a multi-dimensional picture of how that muscle actually functions. For patients and clinicians alike, this is a game-changer.
Muscle Quality Beyond Muscle Mass: Evidence from Adults with Diabetes
One of the most compelling studies of 2025 comes from Kim et al. (2025), published in the Journal of Cachexia, Sarcopenia and Muscle. Their research examined the impact of muscle quality on physical strength and performance in Korean adults — and critically, it looked at whether muscle quality was an independent predictor above and beyond muscle mass and diabetes status.
The findings are striking. Among participants across a range of body compositions and diabetes diagnoses, muscle quality independently predicted both muscle strength and physical performance — meaning that two people with the same amount of muscle mass could have dramatically different functional outcomes depending on the quality of that muscle. Diabetes status (which powerfully affects muscle metabolism through insulin resistance and inflammatory pathways) also interacted with muscle quality to influence outcomes, but muscle quality retained significant explanatory power even after controlling for it.
This research is especially relevant for the hundreds of millions of people worldwide living with type 2 diabetes — a condition that systematically degrades muscle quality through elevated blood glucose, oxidative stress, and mitochondrial dysfunction. For this population, a focus on preserving and improving muscle quality (not just preventing muscle mass loss) may be among the most important preventive strategies available.
The takeaway for patients: If you have diabetes, metabolic syndrome, or are at risk for either, your clinician should be discussing muscle quality — not just body weight or muscle mass — as a key health marker.
The Youth Obesity Paradox: Bigger Muscles, But Poorer Quality
One of the most counterintuitive findings in recent literature comes from a rigorous systematic review and meta-analysis by Inostroza-Mondaca et al. (2025), published in Scientific Reports. This study analyzed data from 15 studies involving 1,475 young people aged roughly 8 to 17 years, comparing those with normal weight to those who were overweight or obese.
Here's the paradox: Absolute muscle strength and muscle cross-sectional area (CSA) were significantly greater in overweight and obese youth compared to normal-weight peers. However, relative muscle strength tended to be lower in overweight and obese youth, suggesting impaired muscle quality.
In other words, overweight and obese children have physically bigger muscles — almost certainly because their bodies have adapted to carry more weight every day, essentially using their body mass as a constant resistance stimulus. But when strength is normalized to body mass or muscle cross-sectional area (i.e., when you ask "how much force does this muscle generate per unit of its size or per kilogram of body weight?"), the picture reverses. Overweight youth produce less force relative to their muscle size, which is the hallmark of reduced muscle quality.
The study also uncovered another critical finding: Muscle oxidative capacity was significantly greater in normal-weight youth versus overweight and obese youth, which might be indicative of muscle mitochondrial dysfunction and impaired oxygen supply, with a potential negative impact on exercise tolerance.
Mitochondrial health is at the very core of muscle quality. Mitochondria are the energy factories inside muscle cells. When they are dysfunctional — as appears to be the case in overweight youth — muscles tire more quickly, recover more slowly, and accumulate metabolic byproducts faster during exercise. This contributes to the commonly observed pattern where overweight children find physical activity harder and less enjoyable, reinforcing a cycle of reduced activity that further degrades muscle quality over time.
Why this matters for parents and pediatric health: Your child's body weight does not tell the whole story of their muscular health. A child who appears physically strong may still have compromised muscle quality that limits their exercise capacity and places them at long-term metabolic risk. Interventions that improve relative strength and aerobic capacity — not just reduce body weight — are essential for overweight and obese youth.
Sarcopenia, Aging, and the Cornerstone Concept
For older adults, the stakes around muscle quality are particularly high. Rizka et al. (2025), writing in Experimental Gerontology, position muscle quality as "the cornerstone for sarcopenia diagnosis and healthy aging" — a framing that reflects a major conceptual shift in geriatrics.
Sarcopenia — the progressive loss of skeletal muscle mass, strength, and function with aging — has traditionally been diagnosed primarily on the basis of muscle mass measurements. But this approach consistently fails to capture all individuals who suffer from its clinical consequences (falls, fractures, loss of independence, increased mortality). Why? Because muscle mass and muscle function are not the same thing.
An older adult with preserved muscle mass but severely infiltrated, low-quality muscle may fall just as frequently and die just as early as one with frank muscle wasting — yet the mass-only screening would miss them entirely. Conversely, a person with somewhat low muscle mass but high muscle quality (dense, fat-free muscle fibers capable of generating strong, efficient contractions) may function far better than their mass-based classification would suggest.
Rizka et al. (2025) make a compelling case that modern sarcopenia diagnosis must go beyond quantity to incorporate robust measures of muscle composition, muscle-specific strength, and functional performance — the same three domains that Costa-Pereira et al. (2026) have proposed as the legitimate scientific successors to the vague "muscle quality" label.
This shift also has profound implications for treatment. If sarcopenia is about quality as much as quantity, then:
Resistance training must be prioritized not just for hypertrophy (building size) but for improving neuromuscular efficiency and reducing intramuscular fat.
Nutritional strategies must emphasize protein quality and timing to support muscle protein synthesis — not just caloric sufficiency.
Metabolic management (blood glucose control, inflammation reduction) must be recognized as essential components of muscle health programs.
How Muscle Quality Is Measured: What Your Doctor Might Be Looking At
Understanding the science is useful, but patients often want to know: how is this actually measured? Here's a brief, plain-language overview of the main tools used in research and clinical settings:
Handgrip Strength / Dynamometry — A simple, affordable measurement of maximum grip strength. When normalized to body mass or muscle mass (creating a "strength-to-mass ratio"), it becomes one of the most practical proxies for muscle-specific strength. Low handgrip strength relative to body size is a red flag for poor muscle quality and is associated with increased cardiometabolic risk, hospitalization, and mortality.
CT Scan (Radiodensity / Hounsfield Units) — CT imaging can measure the density of muscle tissue. Lower-density muscle contains more fat infiltration. "Muscle radiodensity" has emerged as one of the strongest imaging-based predictors of outcomes in cancer, surgery, and aging. However, it requires radiation exposure and specialized analysis.
Ultrasound — Muscle ultrasound can assess echo intensity (a marker of fat and fibrous tissue within muscle), as well as thickness, pennation angle, and fascicle length. It is non-invasive, widely accessible, and increasingly used in sarcopenia screening.
MRI — The gold standard for soft tissue imaging, MRI can provide exquisitely detailed maps of muscle composition, including intramuscular fat distribution. Currently more of a research tool than a routine clinical one, but increasingly important.
BIA (Bioelectrical Impedance Analysis) — Commonly found in fitness centers and clinics, BIA devices measure how electrical current moves through body tissues. While they can estimate lean mass, they are less reliable for capturing muscle quality specifically. Some newer devices are improving in this regard.
Practical Applications: What You Can Do Starting Today
Science is most valuable when it changes behavior. Here are evidence-based, actionable strategies that directly support muscle quality — drawn from the framework established in the 2025–2026 research reviewed here:
1. Prioritize Resistance Training — But Think Quality Over Quantity
Two to three sessions of progressive resistance training per week, targeting major muscle groups, remains the single most powerful intervention for improving muscle-specific strength and reducing intramuscular fat deposition. Focus on compound movements (squats, deadlifts, rows, presses) that recruit large amounts of muscle tissue and drive neuromuscular adaptation.
For youth: Age-appropriate resistance exercises (bodyweight, resistance bands, supervised weight training) are safe and critical for building muscle quality during the developmental years. Physical education programs should prioritize relative strength and aerobic fitness, not just muscle bulk.
For older adults: Even low-load resistance training performed to muscular fatigue improves muscle quality significantly. Prioritize this above almost all other exercise modalities if you are over 60.
2. Optimize Protein Intake — Quality and Timing Matter
Muscle protein synthesis requires adequate dietary protein, but research increasingly shows that when and what type of protein you eat matters as much as total quantity. Aim for 25–40g of high-quality protein (containing all essential amino acids) at each major meal. Leucine-rich sources (chicken, fish, eggs, dairy, legumes combined with grains) are particularly effective at stimulating muscle protein synthesis.
For older adults and those with metabolic disease, protein requirements may be higher than conventional recommendations — some experts suggest 1.2–1.6g/kg of body weight per day.
3. Manage Metabolic Health Aggressively
Elevated blood glucose, chronic inflammation, and insulin resistance are among the most potent drivers of muscle quality decline. The Kim et al. (2025) findings underscore that diabetes and metabolic status interact directly with muscle quality outcomes. Strategies that improve metabolic health — including dietary modification, aerobic exercise, weight management, sleep optimization, and medical treatment when appropriate — also directly protect muscle quality.
4. Reduce Sedentary Time
The Inostroza-Mondaca et al. (2025) meta-analysis in youth highlights that impaired muscle oxidative capacity accompanies overweight status — and oxidative capacity is critically dependent on how much you move. Breaking up prolonged sitting with even brief bouts of movement (a few minutes of walking every 30–45 minutes) helps preserve mitochondrial function in muscle tissue.
5. Monitor Relative Strength, Not Just Body Weight
If you have access to handgrip dynamometry (increasingly available in gyms and clinics), track your grip strength relative to body weight over time. A declining strength-to-weight ratio — even with stable body weight — signals deteriorating muscle quality and warrants attention.
Frequently Asked Questions About Muscle Quality
Q1: What is the difference between muscle mass and muscle quality? Muscle mass refers to the total amount of skeletal muscle tissue in your body. Muscle quality refers to how well that muscle functions — including its composition (fat infiltration), structural architecture, and the amount of force it can generate per unit of its size. Two people can have identical muscle mass but dramatically different muscle quality and physical function.
Q2: Can I have good muscle quality even if I have low muscle mass? Yes. Muscle quality and muscle mass are related but distinct. Some individuals — particularly leaner, highly active older adults — maintain excellent muscle quality (dense, efficient, low-fat muscle fibers) despite having modest overall muscle mass. Conversely, larger muscles can be infiltrated with fat and generate relatively little force, representing poor muscle quality.
Q3: How does obesity affect muscle quality in children? Research by Inostroza-Mondaca et al. (2025) found that while overweight and obese youth tend to have physically larger muscles than normal-weight peers (due to chronic mechanical loading), their relative muscle strength (force per unit of body mass or muscle size) tends to be lower, and their muscle oxidative capacity is significantly impaired. This means their muscles are less metabolically efficient and tire more easily — contributing to reduced exercise tolerance and physical activity avoidance.
Q4: Is sarcopenia only about muscle loss? Traditionally, sarcopenia has been diagnosed primarily based on muscle mass loss. However, Rizka et al. (2025) argue that muscle quality — including muscle-specific strength and muscle composition — must be central to sarcopenia diagnosis and monitoring. Individuals with preserved mass but poor quality muscle can suffer the same functional consequences as those with frank muscle wasting.
Q5: Does diabetes affect muscle quality specifically? Yes. Kim et al. (2025) demonstrated that muscle quality independently predicts physical performance above and beyond diabetes status — meaning that diabetes interacts with, but does not fully explain, the variance in muscle quality outcomes. Type 2 diabetes impairs muscle quality through multiple mechanisms, including insulin resistance (which blunts muscle protein synthesis), chronic inflammation, elevated blood glucose (which promotes intramuscular fat deposition), and mitochondrial dysfunction.
Q6: What is the best way to measure muscle quality in a clinical setting? There is currently no single universally accepted clinical measurement. Practical options include grip strength normalized to body mass (as a muscle-specific strength proxy), muscle ultrasound to assess echo intensity and architecture, and CT-derived muscle radiodensity, where imaging is already being performed. Costa-Pereira et al. (2026) advocate for clearer, standardized terminology and measurement frameworks across clinical practice to improve comparability and consistency.
Q7: Can muscle quality be improved at any age? Yes — and this is one of the most encouraging findings across the literature. Progressive resistance training, adequate dietary protein, metabolic health management, and avoidance of prolonged sedentary behavior have all been shown to improve muscle quality markers across the lifespan — from adolescents to adults in their 80s. It is never too early and never too late to invest in muscle quality.
Clinical Pearls:
1. The "Marbling" Effect (Myosteatosis)
Scientific Perspective: Intramuscular adipose tissue (IMAT), or myosteatosis, significantly reduces muscle radiodensity and impairs force production per unit of cross-sectional area. It serves as an independent risk factor for insulin resistance and mobility disability, regardless of total lean mass.
Patient Perspective: Think of your muscle like a steak. High-quality muscle is lean; low-quality muscle is "marbled" with fat. Even if your arms look the same size, if they are "marbled" with fat on the inside, they will be weaker and make your blood sugar harder to control.
2. Relative Strength as a Vital Sign
Scientific Perspective: Absolute strength often scales with body size, but relative strength (strength-to-mass ratio) is the superior predictor of metabolic health. In pediatric and geriatric populations, a deficit in relative strength often signals underlying mitochondrial dysfunction and poor oxidative capacity.
Patient Perspective: It’s not about how much total weight you can lift; it’s about how much weight you can lift compared to your own body size. If you are getting heavier but not stronger, your "muscle quality" is likely dropping, which is a red flag for your future health.
3. The "Hardware vs. Software" Distinction
Scientific Perspective: Muscle quality is dictated not just by contractile tissue (the hardware) but by neuromuscular recruitment efficiency (the software). High muscle quality involves optimal motor unit firing rates and synchronization, which can improve through resistance training even in the absence of hypertrophy.
Patient Perspective: Your muscles are like a machine, but your nerves are the computer that runs them. You can make your "machine" much more powerful by "updating the software"—training your brain and nerves to use the muscle you already have more efficiently.
Shutterstock
4. Sarcopenia’s "Silent" Progression
Scientific Perspective: The "sarcopenia of aging" often begins as a decline in muscle quality and power long before a significant drop in muscle mass is detectable on a DEXA scan. Relying solely on mass measurements can lead to a "false negative" diagnosis in overweight or "skinny fat" (sarcopenic obese) individuals.
Patient Perspective: You can lose the power and health of your muscle long before the muscle actually looks smaller. Don't wait until your muscles look "wasted" to take action; if you feel slower or less stable, your muscle quality may already be declining.
5. Mitochondrial Capacity & Exercise Tolerance
Scientific Perspective: Reduced muscle oxidative capacity is a hallmark of poor muscle quality, particularly in overweight youth. This mitochondrial impairment limits oxygen utilization, leading to early lactate accumulation and perceived exertion that is disproportionately high for the workload.
Patient Perspective: If you find yourself getting exhausted much faster than others during simple activities, it might not just be "poor cardio." It could be that the "energy factories" (mitochondria) inside your muscles aren't working efficiently, making every movement feel like a mountain climb.
Call to Action: Take Charge of Your Muscle Health Today
The science is clear, and it's deeply empowering: you have more control over your muscle health than you may realize. Muscle quality is not simply a genetic gift that fades inevitably with time — it is a dynamic, modifiable biological characteristic that responds to how you move, eat, sleep, and manage your metabolic health.
Here are three simple steps to begin your muscle quality journey right now:
Step 1 — Get assessed. Ask your doctor or physiotherapist about a functional muscle assessment. Even a simple handgrip strength test, normalized to your body weight, can give you a baseline picture of your muscle-specific strength. If you are over 50, ask about a sarcopenia screening.
Step 2 — Start resistance training this week. You don't need a gym. Two to three sessions per week of bodyweight exercises — squats, push-ups, lunges, rows with a resistance band — are enough to begin improving neuromuscular function and reducing intramuscular fat. Progressive difficulty over time is the key.
Step 3 — Review your protein intake. Track your protein consumption for three days. Are you reaching 1.2–1.6g per kilogram of body weight? Are you distributing it across meals rather than consuming most of it in one sitting? Small adjustments here can make a meaningful difference to muscle protein synthesis and quality.
Author’s Note
The concept of muscle health is evolving—and this article reflects a deliberate shift away from traditional, mass-centric thinking toward a more nuanced, function-oriented perspective grounded in emerging evidence from 2025–2026. As clinicians and researchers, we are increasingly recognizing that skeletal muscle is not merely a structural tissue but a dynamic metabolic organ, central to mobility, glucose regulation, and healthy aging.
This piece was written with two parallel audiences in mind:
Clinicians, who must move beyond conventional metrics and integrate muscle quality into routine assessment and management strategies.
Patients and health-conscious readers deserve clear, actionable insights that translate complex science into meaningful daily practice.
Every effort has been made to synthesize current peer-reviewed literature into a format that is both scientifically rigorous and practically relevant. However, the field of muscle quality remains in transition. Definitions are still being refined, measurement techniques are evolving, and consensus guidelines are not yet fully standardized. As such, some concepts discussed here represent the leading edge of research rather than settled clinical doctrine.
Importantly, this article is not intended to replace individualized medical advice. Muscle health exists at the intersection of aging, metabolism, physical activity, and chronic disease, and must be interpreted within the context of each patient’s unique clinical profile.
If there is one central message to take away, it is this: muscle quality is modifiable. Through targeted exercise, optimal nutrition, and metabolic health management, meaningful improvements are achievable at virtually any age. This represents not only a shift in scientific understanding, but a powerful opportunity for prevention, rehabilitation, and long-term health optimization.
— Dr T. S. Didwal, MD (Internal Medicine)
This article is written for educational purposes and reflects the findings of peer-reviewed research published in 2025–2026. It is not intended as medical advice. Please consult a qualified healthcare professional before making changes to your exercise, nutrition, or medical management plan.
Related Articles
Muscle Quality vs Muscle Mass: Why Strength Per Pound Predicts Healthy Aging and Longevity
References
Kim, J., Shin, C., Jung, I., Park, S., Lee, D., Yu, J., Cho, H., Lee, S., Kim, K., Song, E., Kim, K., Kim, N., Yoo, H., Kim, S., Choi, K., Kim, N., & Seo, J. (2025). Impact of muscle quality on muscle strength and physical performance beyond muscle mass or diabetes status. Journal of Cachexia, Sarcopenia and Muscle, 16, e13760. https://doi.org/10.1002/jcsm.13760
Inostroza-Mondaca, M., Valdés, O., Ramirez-Campillo, R., & Granacher, U. (2025). Muscle strength, muscle morphology, and oxidative capacity in normal weight versus overweight and obese youth: A systematic review with meta-analysis. Scientific Reports, 15, 36108. https://doi.org/10.1038/s41598-025-24024-5
Rizka, M., Pohan, R. A., & Andrianie, S. (2025). Beyond quantity: Muscle quality as the cornerstone for sarcopenia diagnosis and healthy aging. Experimental Gerontology, 212, 112956. https://doi.org/10.1016/j.exger.2025.112956
Costa-Pereira, J. P., Gonzalez, M. C., Cruz-Jentoft, A. J., Goodpaster, B. H., Daly, R. M., Fayh, A. P. T., Heymsfield, S. B., & Prado, C. M. (2026). "Muscle quality": Rethinking an imprecise term. European Geriatric Medicine, 17, 11–24. https://doi.org/10.1007/s41999-025-01373-y