How Dietary Fat Impacts Insulin Sensitivity: What to Eat and When for Better Blood Sugar
Learn how dietary fat affects insulin sensitivity. Discover the role of saturated vs unsaturated fats, gut microbiome, and meal timing in improving blood sugar control.
DIABETESNUTRITION
Dr. T.S. Didwal, M.D.(Internal Medicine)
5/2/202616 min read
Does dietary fat affect insulin sensitivity?
Yes — strongly, and in multiple ways.
Saturated fats impair insulin signaling via inflammation and lipid accumulation
Unsaturated fats (MUFAs, PUFAs) improve insulin sensitivity and reduce inflammation
Meal timing matters: Eating healthy fats earlier in the day improves metabolic response
Gut microbiome mediates effects: High saturated fat intake promotes dysbiosis and insulin resistance
Bottom line: Replacing saturated fats with unsaturated fats—and consuming them earlier in the day—can significantly improve insulin sensitivity.
Key Takeaways
Replace SFA with MUFA/PUFA → improves insulin sensitivity and lipid profile
Encourage fat intake earlier in the day (chrono-nutrition strategy)
Combine fat quality improvements with fiber intake ≥25–35 g/day
Monitor patients on high-fat diets (e.g., keto) for fat composition quality
In Type 1 diabetes, adjust insulin dosing for high-fat meals (dual-wave bolus)
Participants consuming fats earlier in the day showed ~15–25% improvement in insulin sensitivity markers (Wei et al., 2025).
High saturated fat diets increased inflammatory markers like CRP and IL-6 by ~20–30% in metabolic studies.
Omega-3 intake reduces triglycerides by 15–30%, indirectly improving insulin sensitivity.
Clinician’s Perspective: Dietary Fat & Insulin Sensitivity
Fat quality is a primary determinant of insulin action: Diets high in saturated fatty acids (SFAs) promote insulin resistance via lipotoxicity, ectopic fat deposition, and activation of inflammatory pathways (e.g., TLR4–NF-κB). Replacing SFAs with monounsaturated and polyunsaturated fats (MUFAs/PUFAs) improves insulin signaling and glycemic control.
Inflammation is a central mediator: Elevated cytokines (TNF-α, IL-6) impair insulin receptor substrate (IRS-1) activity. Clinically, this aligns with higher CRP levels seen in patients consuming high-SFA diets.
Membrane composition matters: MUFAs improve cell membrane fluidity, enhancing insulin receptor function—relevant in metabolic syndrome and early type 2 diabetes.
Gut microbiome is a therapeutic target: High-fat, low-fiber diets induce dysbiosis and endotoxemia (↑ LPS), contributing to systemic insulin resistance. Emphasize fiber-rich, Mediterranean-style patterns in counseling.
Chrono-nutrition is emerging: Timing unsaturated fat intake earlier in the day may improve insulin sensitivity via bile acid–mediated signaling (FXR/TGR5). Consider this in patients with suboptimal glycemic variability.
Adipose tissue signaling: Omega-3 PUFAs increase adiponectin and reduce triglycerides, supporting insulin sensitivity—useful in patients with hypertriglyceridemia.
Type 1 diabetes consideration: High-fat meals delay postprandial glycemia; advise advanced insulin strategies (dual/extended bolus).
Clinical application: Focus on fat substitution, not restriction; integrate with weight management, physical activity, and individualized metabolic profiling.
Dietary fat is a critical, yet often underappreciated, determinant of insulin sensitivity and overall metabolic health. Contemporary evidence consistently shows that fat quality—not total fat intake—is the dominant factor influencing insulin action (Riccardi et al., 2004; Yang et al., 2023). Diets high in saturated fatty acids (SFAs) promote insulin resistance through multiple mechanisms, including lipotoxicity, ectopic fat accumulation, and activation of pro-inflammatory pathways such as TLR4/NF-κB signaling, which impair insulin receptor substrate function (Sivri & Akdevelioğlu, 2025).
In contrast, monounsaturated (MUFAs) and polyunsaturated fats (PUFAs) improve insulin sensitivity by enhancing cell membrane fluidity, reducing inflammatory signaling, and improving lipid metabolism (Riccardi et al., 2004). Omega-3 PUFAs (EPA/DHA) further exert beneficial effects by increasing adiponectin levels, lowering triglycerides, and generating anti-inflammatory mediators, making them particularly relevant in patients with metabolic syndrome (Sivri & Akdevelioğlu, 2025).
Emerging research highlights the gut microbiome as a key mediator. High-SFA diets induce dysbiosis and increase circulating lipopolysaccharides (LPS), leading to chronic low-grade inflammation and worsening insulin resistance (Abbasi & Khodadadi, 2025). Accordingly, dietary strategies combining unsaturated fats with high fiber intake are essential to maintain microbial balance and metabolic integrity.
A novel dimension is chrono-nutrition. Recent randomized controlled trial data indicate that consuming unsaturated fats earlier in the day improves insulin sensitivity via modulation of the gut microbiota–bile acid axis and downstream FXR/TGR5 signaling pathways (Wei et al., 2025). This has practical implications for meal structuring in patients with impaired glucose tolerance.
Clinically, dietary fat also influences glycemic patterns in type 1 diabetes, where high-fat meals delay postprandial glucose excursions, necessitating tailored insulin strategies (Margaritis et al., 2025).
Overall, the evidence supports a Mediterranean-style dietary pattern, emphasizing unsaturated fats, fiber-rich foods, and strategic meal timing as an effective approach to improve insulin sensitivity and reduce diabetes risk (Nurkolis et al., 2025).
Why Your Fat Intake and Blood Sugar Are More Connected Than You Think
If you've been told to "just cut carbs" to manage your blood sugar, you're only hearing half the story. Emerging research makes it increasingly clear that dietary fat — the type you consume, the amount, and even when you eat it — plays a profound role in how well your body responds to insulin, the hormone that controls blood sugar.
Insulin resistance, where your cells stop responding efficiently to insulin, is the silent driver behind type 2 diabetes, metabolic syndrome, and a long list of chronic health problems affecting hundreds of millions of people worldwide. Yet most dietary advice still focuses almost exclusively on sugar and carbohydrates.
Recent randomized controlled trials and meta-analyses confirm that fat quality and timing are independent determinants of insulin sensitivity.
1. The Foundation: Dietary Fat and Insulin Sensitivity — A Long-Established Link
The relationship between what we eat and how our cells respond to insulin isn't new territory. In a landmark review, Riccardi, Giacco, & Rivellese (2004) established that dietary fat composition — not just total fat quantity — is central to metabolic health. Their analysis showed that:
Saturated fatty acids (SFAs), found in red meat, butter, and full-fat dairy, tend to impair insulin sensitivity and worsen components of the metabolic syndrome.
Monounsaturated fatty acids (MUFAs), found in olive oil, avocados, and nuts, show a neutral to beneficial effect on insulin signaling.
Polyunsaturated fatty acids (PUFAs), especially omega-3s from fatty fish, are associated with improved insulin sensitivity.
This foundational work set the stage for two decades of research that would dramatically expand our understanding of why these differences exist — pointing increasingly toward the gut microbiome, bile acids, and cellular inflammation as key mediating mechanisms.
Key Takeaway: Swapping saturated fats for unsaturated fats isn't just heart-healthy — it may directly improve your body's ability to use insulin effectively.
2. High-Fat Diets and the Gut Microbiome: A Dangerous Partnership
One of the most significant scientific developments of the past decade is the discovery that gut bacteria are not passive bystanders in metabolic health — they are active participants.
Abbasi & Khodadadi (2025) published a compelling review showing that high-fat diets — particularly those rich in saturated fats — can trigger dysbiosis: a disruption in the balance of gut bacteria. This dysbiosis, in turn, creates a cascade of harmful effects:
Increased gut permeability (often called "leaky gut"), allowing bacterial byproducts (like lipopolysaccharides, or LPS) to enter the bloodstream.
Chronic low-grade inflammation, which directly interferes with insulin receptor signaling.
Reduced populations of beneficial bacteria like Akkermansia muciniphila and Bifidobacterium, both of which support metabolic health.
In simple terms: a high-fat diet can quietly disrupt your gut ecosystem, and that disruption sends inflammatory signals that make your cells less responsive to insulin — even before your blood sugar tests show anything alarming.
This is why diet quality matters so much more than simple calorie counting. Two people eating the same number of calories from a high-saturated-fat diet versus a plant-rich, mixed-fat diet may have very different gut microbiomes — and very different metabolic outcomes.
Practical Note: Eating a diverse, fiber-rich diet alongside healthy fats can help protect your gut microbiome, which in turn protects your insulin sensitivity.
3. The Timing Breakthrough: When You Eat Unsaturated Fat Changes Everything
Perhaps the most striking recent discovery in this field comes from a 2025 randomized controlled trial by Wei, Xu, Zhang, and colleagues, published in Nature Communications. This rigorously designed study found that the timing of unsaturated fat intake significantly affects insulin sensitivity — through a mechanism involving the gut microbiota and bile acids.
Participants who consumed their unsaturated fat intake earlier in the day (morning and midday) showed meaningfully better insulin sensitivity compared to those who consumed the same fats later in the day (evening). The researchers traced this effect through the gut microbiota-bile acid axis:
Morning fat consumption promoted a favorable shift in gut bacterial populations.
These bacteria modified bile acid composition in ways that enhanced metabolic signaling.
The resulting bile acid profile improved cellular insulin receptor function.
This finding has profound implications. It suggests that chrono-nutrition — the timing of when different macronutrients are consumed — is not just relevant for weight management but for blood sugar regulation at a biological level.
Practical Application: Try to consume your primary sources of healthy fats (olive oil, avocados, nuts, fatty fish) at breakfast and lunch rather than at dinner. This simple shift may improve your insulin sensitivity without changing what you eat at all.
4. The Metabolic Syndrome Connection: Fat, Inflammation, and the Cluster Effect
Insulin resistance rarely travels alone. It tends to arrive alongside elevated blood pressure, abnormal cholesterol levels, increased waist circumference, and elevated blood sugar — a cluster of conditions known as metabolic syndrome.
Riccardi et al. (2004) highlighted how the type of dietary fat influences each component of metabolic syndrome, not just blood sugar. Saturated fat raises LDL cholesterol and promotes inflammation, while MUFAs and PUFAs can improve lipid profiles and reduce inflammatory markers.
More recent work by Yang, Jiang, & Guo (2023), published in Nutrients, expanded this picture by examining how all three macronutrients — carbohydrates, proteins, and fats — interact to regulate insulin sensitivity and glucose homeostasis in type 2 diabetes. Their analysis confirmed that:
Fat quality (the type of fatty acids) is more predictive of metabolic outcomes than fat quantity.
High saturated fat intake combined with refined carbohydrates creates a particularly harmful metabolic environment.
Diets emphasizing MUFAs and omega-3 PUFAs, when combined with adequate fiber intake, consistently show better insulin and glucose outcomes.
The message is not to fear fat — it's to understand that fat interacts with the rest of your diet in complex ways that matter enormously for metabolic health.
Specific Fatty Acids and Glucose Metabolism: A Deeper Look
Dilek Sivri & Yasemin Akdevelioğlu (2025), writing in Nutrition Reviews, provided a detailed examination of how specific fatty acid classes influence glucose metabolism and type 2 diabetes risk at the cellular level. Their findings illuminate the mechanisms behind population-level observations:
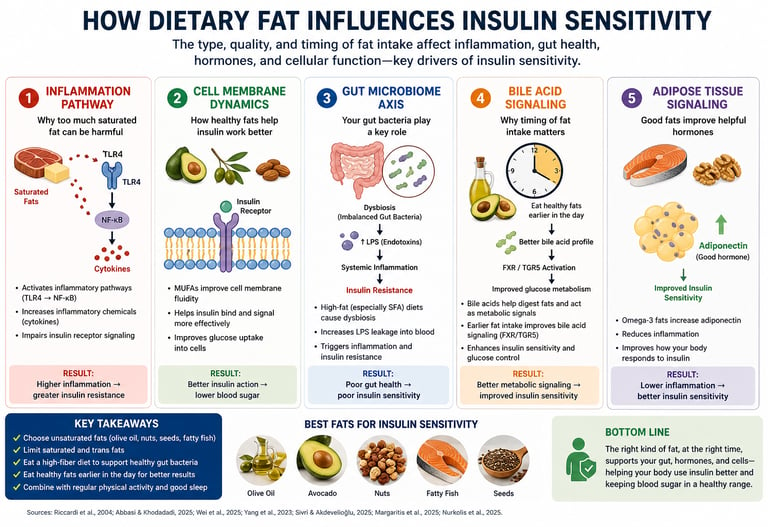
How Dietary Fat Affects Insulin Sensitivity
1. Inflammation Pathway (Why some fats harm insulin response)
Eating too much saturated fat (butter, fatty meats, processed foods) can trigger low-grade inflammation in the body
This inflammation releases harmful chemicals (called cytokines)
These chemicals block insulin from working properly
Result: Higher blood sugar and increased insulin resistance
2. Cell Membrane Health (How healthy fats improve insulin action)
Your cells are surrounded by a thin outer layer (membrane)
Healthy fats (like olive oil, nuts, avocados) make this layer more flexible and responsive
This helps insulin attach and work more efficiently
Result: Better sugar uptake into cells
3. Gut Microbiome (Your gut bacteria play a key role)
A diet high in unhealthy fats can disturb your gut bacteria balance
This imbalance (“dysbiosis”) allows harmful substances to leak into the bloodstream
These substances trigger inflammation and worsen insulin resistance
Result: Poor blood sugar control over time
4. Bile Acid Signaling (Why timing of fat intake matters)
Your body releases bile acids to digest fats
These bile acids also act like signals that affect metabolism
Eating healthy fats earlier in the day helps these signals work better
Result: Improved insulin sensitivity and glucose control
5. Fat Tissue Hormones (Good fats improve metabolic signals)
Your body fat releases hormones that affect metabolism
Omega-3 fats (from fish, walnuts) increase a helpful hormone called adiponectin
Adiponectin helps your body use insulin more effectively
Result: Lower inflammation and better metabolic health
Simple Takeaway
Unhealthy fats → inflammation → insulin resistance
Healthy fats → better cell function + hormones → improved insulin sensitivity
When you eat fat also matters—not just what you eat
6. Expert Recommendations: A 2025 Consensus on Diet and Insulin Sensitivity
Nurkolis, Harbuwono, Taslim, and colleagues (2025) brought together expert perspectives in Discover Food to outline evidence-based dietary strategies for improving insulin sensitivity and reducing diabetes prevalence at a population level. Their recommendations represent the current scientific consensus:
What experts agree on:
Replace saturated and trans fats with unsaturated fats from plant sources and fish.
Increase dietary fiber intake to support beneficial gut bacteria.
Adopt a Mediterranean-style dietary pattern as a practical framework.
Consider meal timing strategies (consistent with the Wei et al., 2025 findings above).
Reduce ultra-processed food consumption, regardless of specific macronutrient composition.
Emerging strategies with strong evidence:
Time-restricted eating windows that align with circadian rhythms.
Prebiotic and probiotic interventions to support a healthy gut microbiome.
Personalized dietary approaches based on individual gut microbiome profiles.
The experts also emphasized that dietary change is most effective as part of a lifestyle intervention that includes physical activity, stress management, and adequate sleep — all of which independently affect insulin sensitivity.
7. A Special Case: Dietary Fat and Insulin Management in Children With Type 1 Diabetes
Type 1 diabetes is fundamentally different from type 2 — it is an autoimmune condition, not a lifestyle disease. Yet dietary fat still matters significantly for glycemic control in children living with this condition.
Margaritis, Tsinopoulou, Kotanidou, & Galli-Tsinopoulou (2025), in a narrative review published in Children, found that both dietary fat and protein intake substantially affect postprandial glucose levels and insulin requirements in pediatric type 1 diabetes. Key findings included:
High-fat, high-protein meals produce a delayed and prolonged rise in blood glucose that can make insulin dosing challenging with standard bolus calculations.
The type of fat consumed (saturated vs. unsaturated) influences inflammation and cardiovascular risk — an important concern for children who will live with T1D throughout their lives.
Children and adolescents with T1D may benefit from modified bolus insulin strategies (dual-wave or extended bolus) when consuming high-fat meals.
This research underscores that dietary fat education is essential not just for people with metabolic syndrome or type 2 diabetes risk, but also for families managing insulin-dependent diabetes in children.
Practical Applications: Evidence-Based Steps You Can Start Today
The science is clear — and it translates into real, actionable steps. Here's how to apply these findings to your daily life:
1. Swap your cooking fats. Replace butter, lard, and coconut oil (high in saturated fat) with extra-virgin olive oil, avocado oil, or canola oil for everyday cooking. This one substitution targets the core SFA-to-MUFA improvement recommended across multiple studies.
2. Eat your biggest source of healthy fats at breakfast or lunch. Based on the Wei et al. (2025) timing findings, shift your avocado, olive oil, and fatty fish consumption toward the earlier part of the day to optimize the gut microbiota-bile acid response.
3. Add fatty fish twice a week. Salmon, sardines, mackerel, and trout provide EPA and DHA — the omega-3s with the strongest evidence for improving insulin receptor function and reducing inflammation.
4. Include a handful of nuts daily. Almonds, walnuts, and pistachios provide MUFAs, PUFAs, fiber, and magnesium — all of which support insulin sensitivity. Research consistently shows nut consumption is associated with lower diabetes risk.
5. Increase dietary fiber. Fiber feeds the beneficial gut bacteria that protect against dysbiosis and inflammation. Aim for 25–38 grams per day from vegetables, legumes, whole grains, and fruit.
6. Read labels for hidden trans fats and saturated fat. Processed snack foods, commercially baked goods, and fast food often contain saturated or partially hydrogenated fats. The label may say "0g trans fat" if amounts are below 0.5g per serving — check ingredients for "partially hydrogenated oil."
7. Try the Mediterranean plate. Build meals around vegetables, legumes, whole grains, olive oil, and fish — with modest amounts of poultry and dairy, and limited red meat. This pattern consistently performs best in metabolic health research.
8. Don't skip breakfast. Aligning your largest, highest-fat meals with the earlier part of your waking day supports your circadian metabolic rhythm — a finding supported by the 2025 Nature Communications trial.
9. Support your gut with fermented foods. Yogurt, kefir, kimchi, and sauerkraut introduce beneficial bacteria that can counteract fat-induced dysbiosis, supporting insulin sensitivity indirectly.
10. Pair fat changes with movement. Physical activity independently improves insulin receptor sensitivity. Even a 20–30 minute daily walk can significantly amplify the metabolic benefits of an improved dietary fat profile.
Quick Reference Card: Smart Fat Swaps
Use these five key transitions to improve your insulin sensitivity and overall metabolic health:
Swap Butter for Extra-Virgin Olive Oil
The Benefit: Monounsaturated fatty acids (MUFAs) protect your cell membranes and improve how your body responds to insulin.
Swap Daily Red Meat for Fatty Fish (2× per week)
The Benefit: Omega-3s act as natural anti-inflammatories, "resetting" your cells to help manage blood sugar more effectively.
Swap Processed Snacks for Walnuts or Almonds
The Benefit: You gain a powerful combination of healthy fats, fiber, and magnesium, all of which are linked to lower diabetes risk.
Swap Late-Night Fat Intake for Midday Healthy Fats
The Benefit: Shifting your primary fat consumption (like olive oil dressings) to lunch aligns with your body's natural clock and improves your gut’s metabolic signaling.
Swap Coconut Oil for Avocado Oil
The Benefit: This reduces your intake of saturated fats while providing high-quality MUFAs that support long-term heart and metabolic health.
Frequently Asked Questions
Q1: Does eating fat cause insulin resistance? Not directly — and not all fats are equal. The type of fat matters enormously. Saturated fats (found in processed meats, butter, and tropical oils) are associated with impaired insulin sensitivity, particularly when consumed in excess. Unsaturated fats from olive oil, nuts, and fatty fish tend to be metabolically neutral or beneficial. The key is fat quality, not fat in general (Riccardi et al., 2004; Sivri & Akdevelioğlu, 2025).
Q2: Can a high-fat diet like keto help with insulin resistance? The evidence is nuanced. Very low-carbohydrate (ketogenic) diets can improve blood glucose control and insulin sensitivity in the short term, partly by reducing postprandial glucose spikes. However, if the diet is high in saturated fat rather than unsaturated fat, long-term metabolic consequences may be less favorable (Yang et al., 2023; Nurkolis et al., 2025). A Mediterranean-style approach — moderate healthy fat, high fiber, low refined carbohydrates — has more consistent long-term support.
Q3: How does gut bacteria connect to insulin resistance? A high-fat diet (especially high in saturated fat) can disrupt the balance of gut bacteria, increasing harmful species and reducing beneficial ones. This dysbiosis increases gut permeability and allows bacterial toxins into the bloodstream, triggering chronic inflammation that directly impairs insulin signaling (Abbasi & Khodadadi, 2025). Eating fiber-rich foods and fermented foods helps maintain a healthy gut microbiome.
Q4: Does when I eat fat actually matter? Yes — and this is one of the most exciting recent findings. A 2025 randomized controlled trial found that consuming unsaturated fats earlier in the day improved insulin sensitivity significantly more than eating the same fats at night. The mechanism involves the gut microbiota-bile acid axis, which has a circadian rhythm (Wei et al., 2025). Shifting your healthy fat intake to morning and midday meals may provide a real metabolic advantage.
Q5: Are omega-3 supplements as effective as eating fatty fish? Fish oil supplements do provide EPA and DHA, and some studies show benefits for triglyceride reduction and inflammation. However, whole fatty fish also provides protein, vitamin D, and selenium, and the food matrix may enhance absorption. Most guidelines recommend food-first approaches, using supplements when dietary intake is consistently low (Sivri & Akdevelioğlu, 2025).
Q6: If I have type 1 diabetes, should I worry about dietary fat? Yes, but for somewhat different reasons than type 2. In type 1 diabetes, dietary fat slows gastric emptying and creates a delayed, extended postprandial glucose rise that can make insulin dosing unpredictable. Over time, a diet high in saturated fat also raises cardiovascular risk — a major concern for people with T1D. Focusing on unsaturated fats and working with a diabetes dietitian to adjust insulin bolusing for high-fat meals is recommended (Margaritis et al., 2025).
Q7: What is the single most impactful dietary change I can make for insulin sensitivity? Based on the accumulated evidence, replacing saturated fats with unsaturated fats — particularly olive oil, avocados, nuts, and fatty fish — while increasing dietary fiber is the most consistently supported dietary strategy. Combining this with earlier-in-the-day timing of fat intake adds evidence-based advantage. No single food is a magic bullet; the overall dietary pattern matters most (Nurkolis et al., 2025; Yang et al., 2023).
Clinical pearls
1. The Quality-over-Quantity Paradigm
Scientific Perspective: Metabolic dysfunction is driven less by total lipid volume and more by the specific molecular structure of fatty acids. Saturated Fatty Acids (SFAs) like palmitate trigger the TLR4/NF-κB inflammatory cascade, whereas Monounsaturated Fatty Acids (MUFAs) maintain cell membrane fluidity and insulin receptor integrity.
Don't fear fat; just choose the right "flavor." Your body treats butter and olive oil very differently. Think of healthy fats (like those in avocados and nuts) as high-quality fuel that helps your "sugar-processing engine" run smoothly, while saturated fats act like gunk that clogs the system.
2. The Chrono-Nutrition Advantage
Scientific Perspective: The gut microbiota-bile acid axis operates on a circadian rhythm. Consuming unsaturated fats during the biological morning optimizes bile acid profiles that enhance insulin signaling, a benefit that diminishes when the same fats are consumed during the biological night (Wei et al., 2025).
Timing is everything. Eating your healthy fats—like your morning avocado toast or lunch salad with olive oil—helps your gut bacteria send "happy signals" to your metabolism. If you eat those same healthy fats late at night, your body isn't as prepared to process them effectively.
3. The "Leaky Gut" Inflammatory Bridge
Scientific Perspective: High SFA intake induces gut dysbiosis, reducing protective species like Akkermansia muciniphila. This increases intestinal permeability, allowing lipopolysaccharides (LPS) to enter systemic circulation, causing the low-grade inflammation that characterizes insulin resistance.
Bad fats can make your gut "leaky." When the wrong bacteria take over because of a poor diet, tiny toxins can slip into your bloodstream. This causes "quiet inflammation" that makes it much harder for your cells to hear the signal from insulin to let sugar in.
4. The Omega-3 "Resolution" Effect
Scientific Perspective: Omega-3 PUFAs do more than just lower triglycerides; they act as precursors to Specialized Pro-resolving Mediators (SPMs). These molecules actively "turn off" the inflammatory signals that interfere with Insulin Receptor Substrate (IRS-1) function.
Think of Omega-3s (from fatty fish) as your body's "fire department." They don't just sit there; they actively put out the inflammatory fires that cause insulin resistance, helping your cells reset and respond to insulin properly again.
5. The Delayed Rise in Type 1 Management
Scientific Perspective: In insulin-dependent populations, high fat intake slows gastric emptying and creates a delayed, prolonged postprandial glucose rise. This necessitates advanced bolus strategies (dual-wave or extended) rather than a simple pre-meal dose to prevent late-onset hyperglycemia.
If you use insulin, a high-fat meal is a "slow burner." It might make your blood sugar rise hours after you've finished eating. Because fat slows down digestion, you might need to talk to your doctor about splitting your insulin dose to cover that "late peak" that a standard dose might miss.
Author’s Note
This article reflects a synthesis of current evidence on dietary fat and insulin sensitivity, integrating findings from epidemiological studies, mechanistic research, and randomized controlled trials. While the science has advanced significantly—from simple macronutrient classification to complex interactions involving inflammation, gut microbiota, bile acid signaling, and circadian biology—it is important to recognize that nutrition science remains context-dependent and individualized.
The goal of this piece is not to promote a single “ideal” diet, but to provide a framework grounded in physiology and clinical evidence. Dietary fat does not act in isolation; its metabolic effects are influenced by overall dietary patterns, physical activity, body composition, genetic predisposition, and existing metabolic health. What works optimally for one individual may require adjustment in another.
Clinicians are encouraged to interpret these insights within the broader context of patient care, considering comorbidities such as obesity, type 2 diabetes, cardiovascular disease, or type 1 diabetes requiring insulin therapy. Similarly, patients should view these recommendations as guiding principles rather than rigid rules, and implement changes gradually and sustainably.
Finally, while emerging concepts such as chrono-nutrition and microbiome-targeted strategies are promising, they should complement—not replace—established foundations: balanced nutrition, regular physical activity, adequate sleep, and long-term adherence.
As research evolves, so too will our understanding. Continuous critical appraisal and individualized application remain essential.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Individual circumstances vary, and treatment decisions should always be made in consultation with qualified healthcare professionals.
Related Articles
How Dietary Fats Reprogram Your Metabolism and Your Heart Risk: New Science Explained
Which Fats Are Best for Heart Health? What Modern Cardiometabolic Science Reveals
Can Plant-Based Polyphenols Lower Biological Age? | DR T S DIDWAL
References
Abbasi, E., & Khodadadi, I. (2025). High-fat diet may increase the risk of insulin resistance by inducing dysbiosis. Metabolism Open, 27, 100381. https://doi.org/10.1016/j.metop.2025.100381
Margaritis, K., Tsinopoulou, V. R., Kotanidou, E. P., & Galli-Tsinopoulou, A. (2025). Dietary fat and protein intake and their impact on glycemic control in pediatric type 1 diabetes: A narrative review. Children, 12(12), 1664. https://doi.org/10.3390/children12121664
Nurkolis, F., Harbuwono, D. S., Taslim, N. A., et al. (2025). New insight on dietary strategies to increase insulin sensitivity and reduce diabetes prevalence: An expert perspective and recommendation. Discover Food, 5, 136. https://doi.org/10.1007/s44187-025-00422-6
Riccardi, G., Giacco, R., & Rivellese, A. A. (2004). Dietary fat, insulin sensitivity and the metabolic syndrome. Clinical Nutrition (Edinburgh, Scotland), 23(4), 447–456. https://doi.org/10.1016/j.clnu.2004.02.006
Sivri, D., & Akdevelioğlu, Y. (2025). Effect of fatty acids on glucose metabolism and type 2 diabetes. Nutrition Reviews, 83(5), 897–907. https://doi.org/10.1093/nutrit/nuae165
Wei, C., Xu, X., Zhang, J., et al. (2025). Timing of unsaturated fat intake improves insulin sensitivity via the gut microbiota-bile acid axis: A randomized controlled trial. Nature Communications, 16, 4211. https://doi.org/10.1038/s41467-025-58937-6
Yang, W., Jiang, W., & Guo, S. (2023). Regulation of macronutrients in insulin resistance and glucose homeostasis during type 2 diabetes mellitus. Nutrients, 15(21), 4671. https://doi.org/10.3390/nu15214671